Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- Exploratory Research | Definition, Guide, & Examples

Exploratory Research | Definition, Guide, & Examples
Published on December 6, 2021 by Tegan George . Revised on November 20, 2023.
Exploratory research is a methodology approach that investigates research questions that have not previously been studied in depth.
Exploratory research is often qualitative and primary in nature. However, a study with a large sample conducted in an exploratory manner can be quantitative as well. It is also often referred to as interpretive research or a grounded theory approach due to its flexible and open-ended nature.
Table of contents
When to use exploratory research, exploratory research questions, exploratory research data collection, step-by-step example of exploratory research, exploratory vs. explanatory research, advantages and disadvantages of exploratory research, other interesting articles, frequently asked questions about exploratory research.
Exploratory research is often used when the issue you’re studying is new or when the data collection process is challenging for some reason.
You can use this type of research if you have a general idea or a specific question that you want to study but there is no preexisting knowledge or paradigm with which to study it.
Here's why students love Scribbr's proofreading services
Discover proofreading & editing
Exploratory research questions are designed to help you understand more about a particular topic of interest. They can help you connect ideas to understand the groundwork of your analysis without adding any preconceived notions or assumptions yet.
Here are some examples:
- What effect does using a digital notebook have on the attention span of middle schoolers?
- What factors influence mental health in undergraduates?
- What outcomes are associated with an authoritative parenting style?
- In what ways does the presence of a non-native accent affect intelligibility?
- How can the use of a grocery delivery service reduce food waste in single-person households?
Collecting information on a previously unexplored topic can be challenging. Exploratory research can help you narrow down your topic and formulate a clear hypothesis and problem statement , as well as giving you the “lay of the land” on your topic.
Data collection using exploratory research is often divided into primary and secondary research methods, with data analysis following the same model.
Primary research
In primary research, your data is collected directly from primary sources : your participants. There is a variety of ways to collect primary data.
Some examples include:
- Survey methodology: Sending a survey out to the student body asking them if they would eat vegan meals
- Focus groups: Compiling groups of 8–10 students and discussing what they think of vegan options for dining hall food
- Interviews: Interviewing students entering and exiting the dining hall, asking if they would eat vegan meals
Secondary research
In secondary research, your data is collected from preexisting primary research, such as experiments or surveys.
Some other examples include:
- Case studies : Health of an all-vegan diet
- Literature reviews : Preexisting research about students’ eating habits and how they have changed over time
- Online polls, surveys, blog posts, or interviews; social media: Have other schools done something similar?
For some subjects, it’s possible to use large- n government data, such as the decennial census or yearly American Community Survey (ACS) open-source data.
How you proceed with your exploratory research design depends on the research method you choose to collect your data. In most cases, you will follow five steps.
We’ll walk you through the steps using the following example.
Therefore, you would like to focus on improving intelligibility instead of reducing the learner’s accent.
Step 1: Identify your problem
The first step in conducting exploratory research is identifying what the problem is and whether this type of research is the right avenue for you to pursue. Remember that exploratory research is most advantageous when you are investigating a previously unexplored problem.
Step 2: Hypothesize a solution
The next step is to come up with a solution to the problem you’re investigating. Formulate a hypothetical statement to guide your research.
Step 3. Design your methodology
Next, conceptualize your data collection and data analysis methods and write them up in a research design.
Step 4: Collect and analyze data
Next, you proceed with collecting and analyzing your data so you can determine whether your preliminary results are in line with your hypothesis.
In most types of research, you should formulate your hypotheses a priori and refrain from changing them due to the increased risk of Type I errors and data integrity issues. However, in exploratory research, you are allowed to change your hypothesis based on your findings, since you are exploring a previously unexplained phenomenon that could have many explanations.
Step 5: Avenues for future research
Decide if you would like to continue studying your topic. If so, it is likely that you will need to change to another type of research. As exploratory research is often qualitative in nature, you may need to conduct quantitative research with a larger sample size to achieve more generalizable results.
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

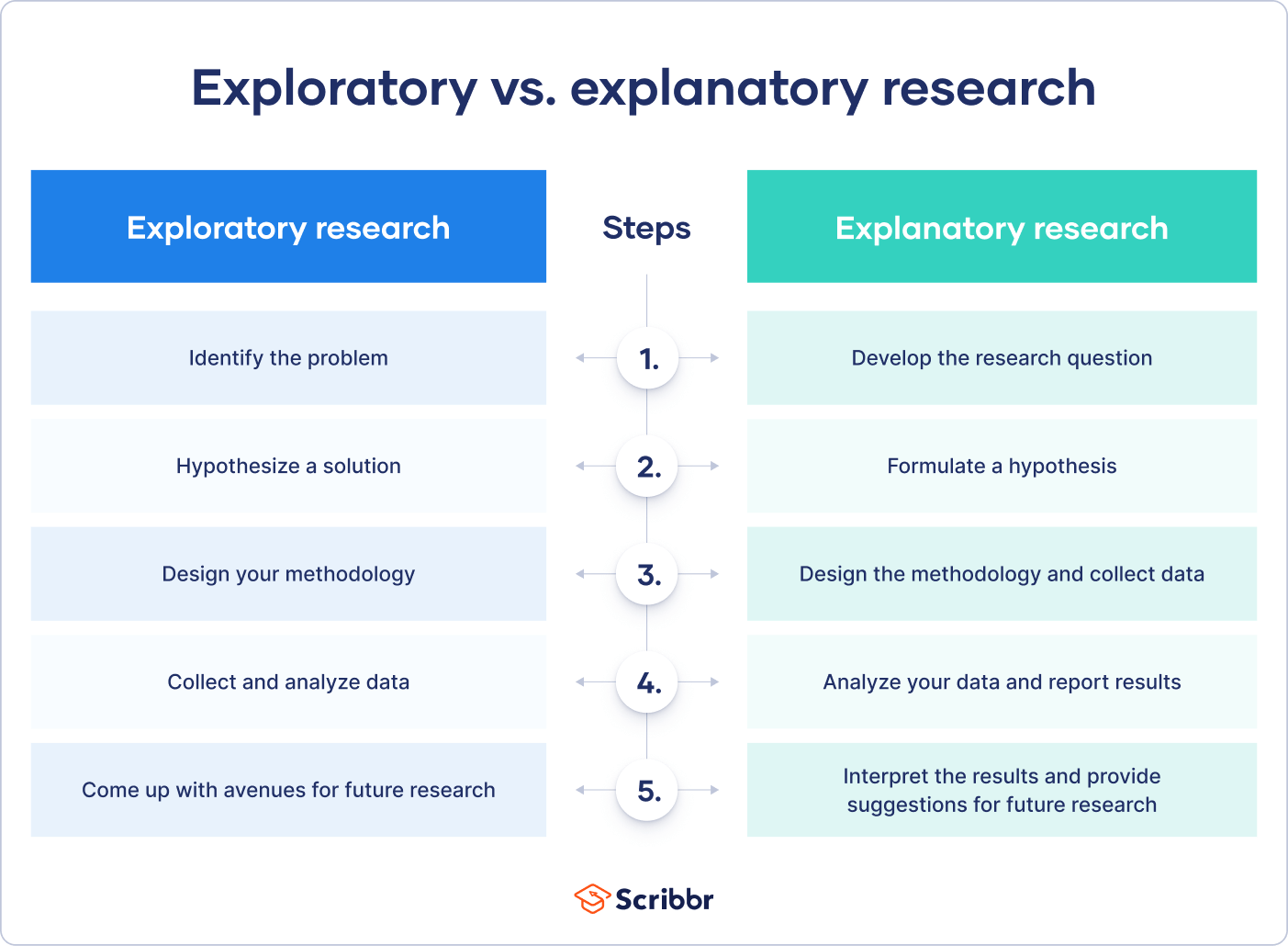
It can be easy to confuse exploratory research with explanatory research. To understand the relationship, it can help to remember that exploratory research lays the groundwork for later explanatory research.
Exploratory research investigates research questions that have not been studied in depth. The preliminary results often lay the groundwork for future analysis.
Explanatory research questions tend to start with “why” or “how”, and the goal is to explain why or how a previously studied phenomenon takes place.
Like any other research design , exploratory studies have their trade-offs: they provide a unique set of benefits but also come with downsides.
- It can be very helpful in narrowing down a challenging or nebulous problem that has not been previously studied.
- It can serve as a great guide for future research, whether your own or another researcher’s. With new and challenging research problems, adding to the body of research in the early stages can be very fulfilling.
- It is very flexible, cost-effective, and open-ended. You are free to proceed however you think is best.
Disadvantages
- It usually lacks conclusive results, and results can be biased or subjective due to a lack of preexisting knowledge on your topic.
- It’s typically not externally valid and generalizable, and it suffers from many of the challenges of qualitative research .
- Since you are not operating within an existing research paradigm, this type of research can be very labor-intensive.
If you want to know more about statistics , methodology , or research bias , make sure to check out some of our other articles with explanations and examples.
- Normal distribution
- Degrees of freedom
- Null hypothesis
- Discourse analysis
- Control groups
- Mixed methods research
- Non-probability sampling
- Quantitative research
- Ecological validity
Research bias
- Rosenthal effect
- Implicit bias
- Cognitive bias
- Selection bias
- Negativity bias
- Status quo bias
Exploratory research is a methodology approach that explores research questions that have not previously been studied in depth. It is often used when the issue you’re studying is new, or the data collection process is challenging in some way.
Exploratory research aims to explore the main aspects of an under-researched problem, while explanatory research aims to explain the causes and consequences of a well-defined problem.
You can use exploratory research if you have a general idea or a specific question that you want to study but there is no preexisting knowledge or paradigm with which to study it.
Quantitative research deals with numbers and statistics, while qualitative research deals with words and meanings.
Quantitative methods allow you to systematically measure variables and test hypotheses . Qualitative methods allow you to explore concepts and experiences in more detail.
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
George, T. (2023, November 20). Exploratory Research | Definition, Guide, & Examples. Scribbr. Retrieved August 29, 2024, from https://www.scribbr.com/methodology/exploratory-research/
Is this article helpful?
Tegan George
Other students also liked, explanatory research | definition, guide, & examples, qualitative vs. quantitative research | differences, examples & methods, what is a research design | types, guide & examples, get unlimited documents corrected.
✔ Free APA citation check included ✔ Unlimited document corrections ✔ Specialized in correcting academic texts
- Methodology
- Open access
- Published: 19 October 2019
Smart literature review: a practical topic modelling approach to exploratory literature review
- Claus Boye Asmussen ORCID: orcid.org/0000-0002-2998-2293 1 &
- Charles Møller 1
Journal of Big Data volume 6 , Article number: 93 ( 2019 ) Cite this article
50k Accesses
220 Citations
3 Altmetric
Metrics details
Manual exploratory literature reviews should be a thing of the past, as technology and development of machine learning methods have matured. The learning curve for using machine learning methods is rapidly declining, enabling new possibilities for all researchers. A framework is presented on how to use topic modelling on a large collection of papers for an exploratory literature review and how that can be used for a full literature review. The aim of the paper is to enable the use of topic modelling for researchers by presenting a step-by-step framework on a case and sharing a code template. The framework consists of three steps; pre-processing, topic modelling, and post-processing, where the topic model Latent Dirichlet Allocation is used. The framework enables huge amounts of papers to be reviewed in a transparent, reliable, faster, and reproducible way.
Introduction
Manual exploratory literature reviews are soon to be outdated. It is a time-consuming process, with limited processing power, resulting in a low number of papers analysed. Researchers, especially junior researchers, often need to find, organise, and understand new and unchartered research areas. As a literature review in the early stages often involves a large number of papers, the options for a researcher is either to limit the amount of papers to review a priori or review the papers by other methods. So far, the handling of large collections of papers has been structured into topics or categories by the use of coding sheets [ 2 , 12 , 22 ], dictionary or supervised learning methods [ 30 ]. The use of coding sheets has especially been used in social science, where trained humans have created impressive data collections, such as the Policy Agendas Project and the Congressional Bills Project in American politics [ 30 ]. These methods, however, have a high upfront cost of time, requiring a prior understanding where papers are grouped by categories based on pre-existing knowledge. In an exploratory phase where a general overview of research directions is needed, many researchers may be dismayed by having to spend a lot of time before seeing any results, potentially wasting efforts that could have been better spent elsewhere. With the advancement of machine learning methods, many of the issues can be dealt with at a low cost of time for the researcher. Some authors argue that when human processing such as coding practice is substituted by computer processing, reliability is increased and cost of time is reduced [ 12 , 23 , 30 ]. Supervised learning and unsupervised learning, are two methods for automatically processing papers [ 30 ]. Supervised learning relies on manually coding a training set of papers before performing an analysis, which entails a high cost of time before a result is achieved. Unsupervised learning methods, such as topic modelling, do not require the researcher to create coding sheets before an analysis, which presents a low cost of time approach for an exploratory review with a large collection of papers. Even though, topic modelling has been used to group large amounts of documents, few applications of topic modelling have been used on research papers, and a researcher is required to have programming skills and statistical knowledge to successfully conduct an exploratory literature review using topic modelling.
This paper presents a framework where topic modelling, a branch of the unsupervised methods, is used to conduct an exploratory literature review and how that can be used for a full literature review. The intention of the paper is to enable the use of topic modelling for researchers by providing a practical approach to topic modelling, where a framework is presented and used on a case step-by-step. The paper is organised as follows. The following section will review the literature in topic modelling and its use in exploratory literature reviews. The framework is presented in “ Method ” section, and the case is presented in “ Framework ” section. “ Discussion ” and “ Conclusion ” sections conclude the paper with a discussion and conclusion.
Topic modelling for exploratory literature review
While there are many ways of conducting an exploratory review, most methods require a high upfront cost of time and having pre-existent knowledge of the domain. Quinn et al. [ 30 ] investigated the costs of different text categorisation methods, a summary of which is presented in Table 1 , where the assumptions and cost of the methods are compared.
What is striking is that all of the methods, except manually reading papers and topic modelling, require pre-existing knowledge of the categories of the papers and have a high pre-analysis cost. Manually reading a large amount of papers will have a high cost of time for the researcher, whereas topic modelling can be automated, substituting the use of the researcher’s time with the use of computer time. This indicates a potentially good fit for the use of topic modelling for exploratory literature reviews.
The use of topic modelling is not new. However, there are remarkably few papers utilising the method for categorising research papers. It has been predominantly been used in the social sciences to identify concepts and subjects within a corpus of documents. An overview of applications of topic modelling is presented in Table 2 , where the type of data, topic modelling method, the use case and size of data are presented.
The papers in Table 2 analyse web content, newspaper articles, books, speeches, and, in one instance, videos, but none of the papers have applied a topic modelling method on a corpus of research papers. However, [ 27 ] address the use of LDA for researchers and argue that there are four parameters a researcher needs to deal with, namely pre-processing of text, selection of model parameters and number of topics to be generated, evaluation of reliability, and evaluation of validity. The uses of topic modelling are to identify themes or topics within a corpus of many documents, or to develop or test topic modelling methods. The motivation for most of the papers is that the use of topic modelling enables the possibility to do an analysis on a large amount of documents, as they would otherwise have not been able to due to the cost of time [ 30 ]. Most of the papers argue that LDA is a state-of-the-art and preferred method for topic modelling, which is why almost all of the papers have chosen the LDA method. The use of topic modelling does not provide a full meaning of the text but provides a good overview of the themes, which could not have been obtained otherwise [ 21 ]. DiMaggio et al. [ 12 ] find a key distinction in the use of topic modelling is that its use is more of utility than accuracy, where the model should simplify the data in an interpretable and valid way to be used for further analysis They note that a subject-matter expert is required to interpret the outcome and that the analysis is formed by the data.
The use of topic modelling presents an opportunity for researchers to add a tool to their tool box for an exploratory and literature review process. Topic modelling has mostly been used on online content and requires a high degree of statistical and technical skill, skills not all researchers possess. To enable more researchers to apply topic modelling for their exploratory literature reviews, a framework will be proposed to lower the requirements for technical and statistical skills of the researcher.
Topic modelling has proven itself as a tool for exploratory analysis of a large number of papers [ 14 , 24 ]. However, it has rarely been applied in the context of an exploratory literature review. The selected topic modelling method, for the framework, is Latent Dirichlet Allocation (LDA), as it is the most used [ 6 , 12 , 17 , 20 , 32 ], state-of-the-art method [ 25 ] and simplest method [ 8 ]. While other topic modelling methods could be considered, the aim of this paper is to enable the use of topic modelling for researchers. For enabling topic modelling for researchers, ease of use and applicability are highly rated, where LDA is easily implemented and understood. Other topic modelling methods could potentially be used in the framework, where reviews of other topic models is presented in [ 1 , 26 ].
The topic modelling method LDA is an unsupervised, probabilistic modelling method which extracts topics from a collection of papers. A topic is defined as a distribution over a fixed vocabulary. LDA analyses the words in each paper and calculates the joint probability distribution between the observed (words in the paper) and the unobserved (the hidden structure of topics). The method uses a ‘Bag of Words’ approach where the semantics and meaning of sentences are not evaluated. Rather, the method evaluates the frequency of words. It is therefore assumed that the most frequent words within a topic will present an aboutness of the topic. As an example, if one of the topics in a paper is LEAN, then it can be assumed that the words LEAN, JIT and Kanban are more frequent, compared to other non-LEAN papers. The result is a number of topics with the most prevalent topics grouped together. A probability for each paper is calculated for each topic, creating a matrix with the size of number of topics multiplied with the number of papers. A detailed description of LDA is found in [ 6 ].
The framework is designed as a step-by-step procedure, where its use is presented in a form of a case where the code used for the analysis is shared, enabling other researchers to easily replicate the framework for their own literature review. The code is based on the open source statistical language R, but any language with the LDA method is suitable for use. The framework can be made fully automated, presenting a low cost of time approach for exploratory literature reviews. An inspiration for the automation of the framework can be found in [ 10 ], who created an online-service, towards processing Business Process Management documents where text-mining approaches such as topic modelling are automated. They find that topic modelling can be automated and argue that the use of a good tool for topic modelling can easily present good results, but the method relies on the ability of people to find the right data, guide the analytical journey and interpret the results.
The aim of the paper is to create a generic framework which can be applied in any context of an exploratory literature review and potentially be used for a full literature review. The method provided in this paper is a framework which is based upon well-known procedures for how to clean and process data, in such a way that the contribution from the framework is not in presenting new ways to process data but in how known methods are combined and used. The framework will be validated by the use of a case in the form of a literature review. The outcome of the method is a list of topics where papers are grouped. If the grouping of papers makes sense and is logical, which can be evaluated by an expert within the research field, then the framework is deemed valid. Compared to other methods, such as supervised learning, the method of measuring validity does not produce an exact degree of validity. However, invalid results will likely be easily identifiable by an expert within the field. As stated by [ 12 ], the use of topic modelling is more for utility than for accuracy.
The developed framework is illustrated in Fig. 1 , and the R-code and case output files are located at https://github.com/clausba/Smart-Literature-Review . The smart literature review process consists of the three steps: pre-processing, topic modelling, and post-processing.
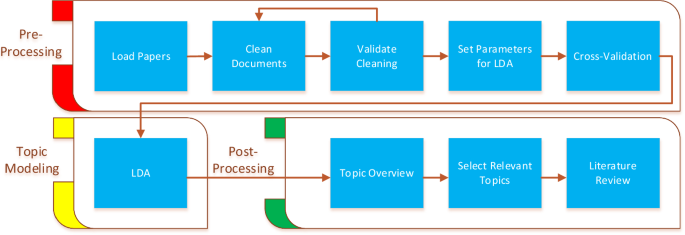
Process overview of the smart literature review framework
The pre-processing steps are getting the data and model ready to run, where the topic-modelling step is executing the LDA method. The post-processing steps are translating the outcome of the LDA model to an exploratory review and using that to identify papers to be used for a literature review. It is assumed that the papers for review are downloaded and available, as a library with the pdf files.
Pre-processing
The pre-processing steps consist of loading and preparing the papers for processing, an essential step for a good analytical result. The first step is to load the papers into the R environment. The next step is to clean the papers by removing or altering non-value-adding words. All words are converted to lower case, and punctuation and whitespaces are removed. Special characters, URLs, and emails are removed, as they often do not contribute to identification of topics. Stop words, misread words and other non-semantic contributing words are removed. Examples of stop words are “can”, “use”, and “make”. These words add no value to the aboutness of a topic. The loading of papers into R can in some instances cause words to be misread, which must either be rectified or removed. Further, some websites add a first page with general information, and these contain words that must be removed. This prevents unwanted correlation between papers downloaded from the same source. Words are stemmed to their root form for easier comparison. Lastly, many words only occur in a single paper, and these should be removed to make computations easier, as less frequent words will likely provide little benefit in grouping papers into topics.
The cleansing process is often an iterative process, as it can be difficult to identify all misread and non-value adding-words a priori. Different papers’ corpora contain different words, which means that an identical cleaning process cannot be guaranteed if a new exploratory review is conducted. As an example, different non-value-adding words exist for the medical field compared to sociology or supply chain management (SCM). The cleaning process is finished once the loaded papers mainly contain value-adding words. There is no known way to scientifically evaluate when the cleaning process is finished, which in some instances makes the cleaning process more of an art than science. However, if a researcher is technically inclined methods, provided in the preText R-package can aid in making a better cleaning process [ 11 ].
LDA is an unsupervised method, which means we do not, prior to the model being executed, know the relationship between the papers. A key aspect of LDA is to group papers into a fixed number of topics, which must be given as a parameter when executing LDA. A key process is therefore to estimate the optimal number of topics. To estimate the number of topics, a cross-validation method is used to calculate the perplexity, as used in information theory, and it is a metric used to evaluate language models, where a low score indicates a better generalisation model, as done by [ 7 , 31 , 32 ]. Lowering the perplexity score is identical to maximising the overall probability of papers being in a topic. Next, test and training datasets are created: the LDA algorithm is run on the training set, and the test set is used to validate the results. The criteria for selecting the right number of topics is to find the balance between a useable number of topics and, at the same time, to keep the perplexity as low as possible. The right number of topics can differ greatly, depending on the aim of the analysis. As a rule of thumb, a low number of topics is used for a general overview and a higher number of topics is used for a more detailed view.
The cross-validation step is used to make sure that a result from an analysis is reliable, by running the LDA method several times under different conditions. Most of the parameters set for the cross-validation should have the same value, as in the final topic modelling run. However, due to computational reasons, some parameters can be altered to lower the amount of computation to save time. As with the number of topics, there is no right way to set the parameters, indicating a trial-and-error process. Most of the LDA implementations have default values set, but in this paper’s case the following parameters were changed: burn-in time, number of iterations, seed values, number of folds, and distribution between training and test sets.
- Topic modelling
Once the papers have been cleaned and a decision has been made on the number of topics, the LDA method can be run. The same parameters as used in the cross-validation should be used as a guidance but for more precise results, parameters can be changed such as a higher number of iterations. The number of folds should be removed, as we do not need a test set, as all papers will be used to run the model. The outcome of the model is a list of papers, a list of probabilities for each paper for each topic, and a list of the most frequent words for each topic.
If an update to the analysis is needed, new papers simply have to be loaded and the post-processing and topic modelling steps can be re-run without any alterations to the parameters. Thus, the framework enables an easy path for updating an exploratory review.
Post-processing
The aim of the post-processing steps is to identify and label research topics and topics relevant for use in a literature review. An outcome of the LDA model is a list of topic probabilities for each paper. The list is used to assign a paper to a topic by sorting the list by highest probability for each paper for each topic. By assigning the papers to the topics with the highest probability, all of the topics contain papers that are similar to each other. When all of the papers have been distributed into their selected topics, the topics need to be labelled. The labelling of the topics is found by identifying the main topic of each topic group, as done in [ 17 ]. Naturally, this is a subjective matter, which can provide different labelling of topics depending on the researcher. To lower the risk of wrongly identified topics, a combination of reviewing the most frequent words for each topic and a title review is used. After the topics have been labelled, the exploratory search is finished.
When the exploratory search has finished, the results must be validated. There are three ways to validate the results of an LDA model, namely statistical, semantic, or predictive [ 12 ]. Statistical validation uses statistical methods to test the assumptions of the model. An example is [ 28 ], where a Bayesian approach is used to estimate the fit of papers to topics. Semantic validation is used to compare the results of the LDA method with expert reasoning, where the results must make semantic sense. In other words, does the grouping of papers into a topic make sense, which ideally should be evaluated by an expert. An example is [ 18 ], who utilises hand coding of papers and compare the coding of papers to the outcome of an LDA model. Predictive validation is used if an external incident can be correlated with an event not found in the papers. An example is in politics where external events, such as presidential elections which should have an impact on e.g. press releases or newspaper coverage, can be used to create a predictive model [ 12 , 17 ].
The chosen method for validation in this framework is semantic validation. The reason is that a researcher will often be or have access to an expert who can quickly validate if the grouping of papers into topics makes sense or not. Statistical validation is a good way to validate the results. However, it would require high statistical skills from the researchers, which cannot be assumed. Predictive validation is used in cases where external events can be used to predict the outcome of the model, which is seldom the case in an exploratory literature review.
It should be noted that, in contrast to many other machine learning methods, it is not possible to calculate a specific measure such as the F-measure or RMSE. To be able to calculate such measures, there must exist a correct grouping of papers, which in this instance would often mean comparing the results to manually created coding sheets [ 11 , 19 , 20 , 30 ]. However, it is very rare that coding sheets are available, leaving the semantic validation approach as the preferred validation method. The validation process in the proposed framework is two-fold. Firstly, the title of the individual paper must be reviewed to validate that each paper does indeed belong in its respective topic. As LDA is an unsupervised method, it can be assumed that not all papers will have a perfect fit within each topic, but if the majority of papers are within the theme of the topic, it is evaluated to be a valid result. If the objective of the research is only an exploratory literature review, the validation ends here. However, if a full literature review is conducted, the literature review can be viewed as an extended semantic validation method. By reviewing the papers in detail within the selected topics of research, it can be validated if the vast majority of papers belong together.
Using the results from the exploratory literature review for a full literature review is simple, as all topics from the exploratory literature review will be labelled. To conduct the full literature review, select the relevant topics and conduct the literature review on the selected papers.
To validate the framework, a case will be presented, where the framework is used to conduct a literature review. The literature review is conducted in the intersection of the research fields analytics, SCM, and enterprise information systems [ 3 ]. As the research areas have a rapidly growing interest, it was assumed that the number of papers would be large, and that an exploratory review was needed to identify the research directions within the research fields. The case used broadly defined keywords for searching for papers, ensuring to include as many potentially relevant papers as possible. Six hundred and fifty papers were found, which were heavily reduced by the use of the smart literature review framework to 76 papers, resulting in a successful literature review. The amount of papers is evaluated to be too time-consuming for a manual exploratory review, which provides a good case to test the smart literature review framework. The steps and thoughts behind the use of the framework are presented in this case section.
The first step was to load the 650 papers into the R environment. Next, all words were converted to lowercase and punctuation, whitespaces, email addresses, and URLs were removed. Problematic words were identified, such as words incorrectly read from the papers. Words included in a publisher’s information page were removed, as they add no semantic value to the topic of a paper. English stop words were removed, and all words were stemmed. As a part of an iterative process, several papers were investigated to evaluate the progress of cleaning the papers. The investigations were done by displaying words in a console window and manually evaluating if more cleaning had to be done.
After the cleaning steps, 256,747 unique words remained in the paper corpus. This is a large number of unique words, which for computational reasons is beneficial to reduce. Therefore, all words that did not have a sparsity or likelihood of 99% to be in any paper were removed. The operation lowered the amount of unique words to 14,145, greatly reducing the computational needs. The LDA method will be applied on the basis of the 14,145 unique words for the 650 papers. Several papers were manually reviewed, and it was evaluated that removal of the unique words did not significantly worsen the ability to identify main topics of the paper corpus.
The last step of pre-processing is to identify the optimal number of topics. To approximate the optimal number of topics, two things were considered. The perplexity was calculated for different amounts of topics, and secondly the need for specificity was considered.
At the extremes, choosing one topic would indicate one topic covering all papers, which will provide a very coarse view of the papers. On the other hand, if the number of topics is equal to the number of papers, then a very precise topic description will be achieved, although the topics will lose practical use as the overview of topics will be too complex. Therefore, a low number of topics was preferred as a general overview was required. Identifying what is a low number of topics will differ depending on the corpus of papers, but visualising the perplexity can often provide the necessary aid for the decision.
The perplexity was calculated over five folds, where each fold would identify 75% of the papers for training the model and leave out the remaining 25% for testing purposes. Using multiple folds reduces the variability of the model, ensuring higher reliability and reducing the risk of overfitting. For replicability purposes, specific seed values were set. Lastly, the number of topics to evaluate is selected. In this case, the following amounts of topics were selected: 2, 3, 4, 5, 10, 20, 30, 40, 50, 75, 100, and 200. The perplexity method in the ‘topicmodels’ R library is used, where the specific parameters can be found in the provided code.
The calculations were done over two runs. However, there is no practical reason for not running the calculations in one run. The first run included all values of number of topics below 100, and the second run calculated the perplexity for 100 and 200 number of topics. The runtimes for the calculations were respectively 9 and 10 h on a standard issue laptop. The combined results are presented in Fig. 2 , and the converged results can be found in the shared repository.
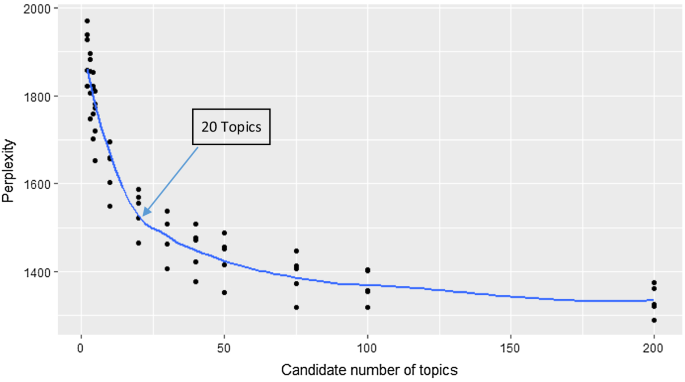
5-Fold cross-validation of topic modelling. Results of cross-validation
The goal in this case is to find the lowest number of topics, which at the same time have a low perplexity. In this case, the slope of the fitted line starts to gradually decline at twenty topics, which is why the selected number of topics is twenty.
Case: topic modelling
As the number of topics is chosen, the next step is to run the LDA method on the entire set of papers. The full run of 650 papers for 20 topics took 3.5 h to compute on a standard issue laptop. An outcome of the method is a 650 by 20 matrix of topic probabilities. In this case, the papers with the highest probability for each topic were used to allocate the papers. The allocation of papers to topics was done in Microsoft Excel. An example of how a distribution of probabilities is distributed across topics for a specific paper is depicted in Fig. 3 . Some papers have topic probability values close to each other, which could indicate a paper belonging to an intersection between two or more topics. These cases were not considered, and the topic with the highest probability was selected.
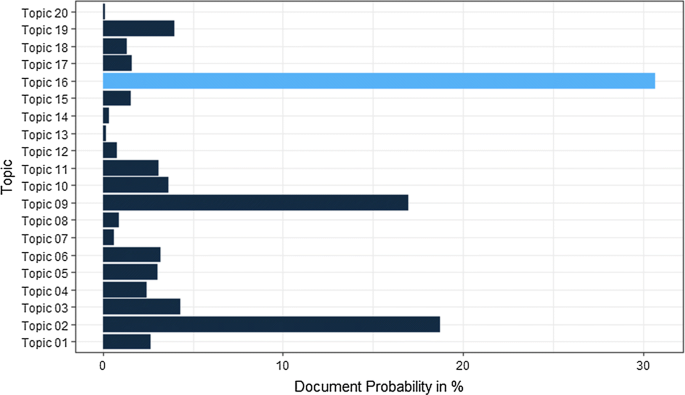
Example of probability distribution for one document (Topic 16 selected)
The allocation of papers to topics resulted in the distribution depicted in Fig. 4 . As can be seen, the number of papers varies for each topic, indicating that some research areas have more publications than others do.
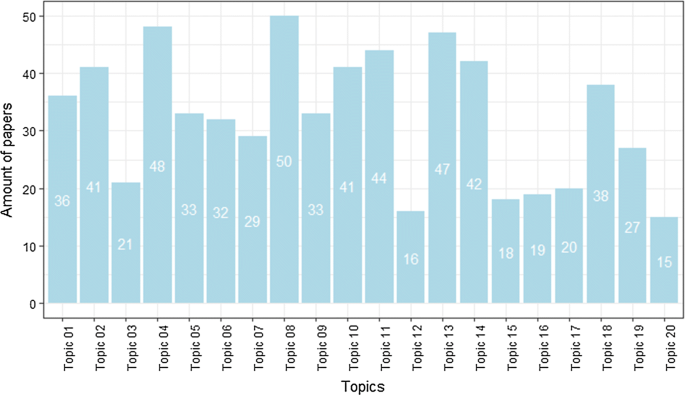
Distribution of papers per topic
Next step is to process the findings and find an adequate description of the topics. A combination of reviewing the most frequent words and a title review was used to identify the topic names. Practically, all of the paper titles and the most frequent words for each topic, were transferred to a separate Excel spreadsheet, providing an easy overview of paper titles. An example for topic 17 can be seen in Table 3 . The most frequent words for the papers in topic 17 are “data”, “big” and “analyt”. Many of the paper titles also indicate usage of big data and analytics for application in a business setting. The topic is named “Big Data Analytics”.
The process was repeated for all other topics. The names of the topics are presented in Tables 4 and 5 .
Based on the names of the topics, three topics were selected based on relevancy for the literature review. Topics 5, 13, and 17 were selected, with a total of 99 papers. In this specific case, it was deemed that there might be papers with a sub-topic that is not relevant for the literature review. Therefore, an abstract review was conducted for the 99 papers, creating 10 sub-topics, which are presented in Table 6 .
The sub-topics RFID, Analytical Methods, Performance Management, and Evaluation and Selection of IT Systems were evaluated to not be relevant for the literature review. Seventy-six papers remained, grouped by sub-topics.
The outcome of the case was an overview of the research areas within the paper corpus, represented by the twenty topics and the ten sub-topics. The selected sub-topics were used to conduct a literature review. The validation of the framework consisted of two parts. The first part addressed the question of whether the grouping of papers, evaluated by the title and keywords, makes sense and the second part addressed whether the literature review revealed any misplaced papers. The framework did successfully place the selected papers into groups of papers that resemble each other. There was only one case where a paper was misplaced, namely that a paper about material informatics was placed among the papers in the sub-topic EIS and Analytics. The grouping and selection of papers in the literature review, based on the framework, did make semantic sense and was successfully used for a literature review. The framework has proven its utility in enabling a faster and more comprehensive exploratory literature review, as compared to competing methods. The framework has increased the speed for analysing a large amount of papers, as well as having increased the reliability in comparison with manual reviews as the same result can be obtained by running the analysis once again. The transparency in the framework is higher than in competing methods, as all steps of the framework are recorded in the code and output files.
This paper presents an approach not often found in academia, by using machine learning to explore papers to identify research directions. Even though the framework has its limitations, the results and ease of use leave a promising future for topic-modelling-based exploratory literature reviews.
The main benefit of the framework is that it provides information about a large number of papers, with little effort on the researcher’s part, before time-costly manual work is to be done. It is possible, by the use of the framework, to quickly navigate many different paper corpora and evaluate where the researchers’ time and focus should be spent. This is especially valuable for a junior researcher or a researcher with little prior knowledge of a research field. If default parameters and cleaning settings can be found for the steps in the framework, a fully automatic grouping of papers could be enabled, where very little work has to be done to achieve an overview of research directions. From a literature review perspective, the benefit of using the framework is that the decision to include or exclude papers for a literature review will be postponed to a later stage where more information is provided, resulting in a more informed decision-making process. The framework enables reproducibility, as all of the steps in the exploratory review process can be reproduced, and enables a higher degree of transparency than competing methods do, as the entire review process can, in detail, be evaluated by other researchers.
There is practically no limit of the number of papers the framework is able to process, which could enable new practices for exploratory literature reviews. An example is to use the framework to track the development of a research field, by running the topic modelling script frequently or when new papers are published. This is especially potent if new papers are automatically downloaded, enabling a fully automatic exploratory literature review. For example, if an exploratory review was conducted once, the review could be updated constantly whenever new publications are made, grouping the publications into the related topics. For this, the topic model has to be trained properly for the selected collection of papers, where it can be assumed that minor additions of papers would likely not warrant any changes to the selected parameters of the model. However, as time passes and more papers are processed, the model will learn more about the collection of papers and provide a more accurate and updated result. Having an automated process could also enable a faster and more reliable method to do post-processing of the results, reducing the post-analysis cost identified for topic modelling by [ 30 ], from moderate to low.
The framework is designed to be easily used by other researchers by designing the framework to require less technical knowledge than a normal topic model usage would entail and by sharing the code used in the case work. The framework is designed as a step-by-step approach, which makes the framework more approachable. However, the framework has yet not been used by other researchers, which would provide valuable lessons for evaluating if the learning curve needs to be lowered even further for researchers to successfully use the framework.
There are, however, considerations that must be addressed when using the smart literature review framework. Finding the optimal number of topics can be quite difficult, and the proposed method of cross-validation based on the perplexity presented a good, but not optimal, solution. An indication of why the number of selected topics is not optimal is the fact that it was not possible to identify a unifying topic label for two of the topics. Namely topics 12 and 20, which were both labelled miscellaneous. The current solution to this issue is to evaluate the relevancy of every single paper of the topics that cannot be labelled. However, in future iterations of the framework, a better identification of the number of topics must be developed. This is a notion also recognised by [ 6 ], who requested that researchers should find a way to label and assign papers to a topic other than identifying the most frequent words. An attempt was made by [ 17 ] to generate automatic labelling on press releases, but it is uncertain if the method will work in other instances. Overall, the grouping of papers in the presented case into topics generally made semantic sense, where a topic label could be found for the majority of topics.
A consideration when using the framework is that not all steps have been clearly defined, and, e.g., the cleaning step is more of an art than science. If a researcher has no or little experience in coding or executing analytical models, suboptimal results could occur. [ 11 , 25 , 27 ] find that especially the pre-processing steps can have a great impact on the validity of results, which further emphasises the importance of selecting model parameters. However, it is found that the default parameters and cleaning steps set in the code provided a sufficiently valid and useable result for an exploratory literature analysis. Running the code will not take much of the researcher’s time, as the execution of code is mainly machine time, and verifying the results takes a limited amount of a researcher time.
Due to the semantic validation method used in the framework, it relies on the availability of a domain expert. The domain expert will not only validate if the grouping of papers into topics makes sense, but it is also their responsibility to label the topics [ 12 ]. If a domain expert is not available, it could lead to wrongly labelled topics and a non-valid result.
A key issue with topic modelling is that a paper can be placed in several related topics, depending on the selected seed value. The seed value will change the starting point of the topic modelling, which could result in another grouping of papers. A paper consists of several sub-topics and depending on how the different sub-topics are evaluated, papers can be allocated to different topics. A way to deal with this issue is to investigate papers with topic probabilities close to each other. Potential wrongly assigned papers can be identified and manually moved if deemed necessary. However, this presents a less automatic way of processing the papers, where future research should aim to improve the assignments of papers to topics or create a method to provide an overview of potentially misplaced papers. It should be noted that even though some papers can be misplaced, the framework provides outcome files than can easily be viewed to identify misplaced papers, by a manual review.
As the smart literature review framework heavily relies on topic modelling, improvements to the selected topic model will likely present better results. The results of the LDA method have provided good results, but more accurate results could be achieved if the semantic meaning of the words would be considered. The framework has only been tested on academic papers, but there is no technical reason to not include other types of documents. An example is to use the framework in a business context to analyse meeting minutes notes to analyse the discussion within the different departments in a company. For this to work, the cleaning parameters would likely have to change, and another evaluation method other than a literature review would be applicable. Further, the applicability of the framework has to be assessed on other streams of literature to be certain of its use for exploratory literature reviews at large.
This paper aimed to create a framework to enable researchers to use topic modelling to, do an exploratory literature review, decreasing the need for manually reading papers and, enabling the possibility to analyse a greater, almost unlimited, amount of papers, faster, more transparently and with greater reliability. The framework is based upon the use of the topic model Latent Dirichlet Allocation, which groups related papers into topic groups. The framework provides greater reliability than competing exploratory review methods provide, as the code can be rerun on the same papers, which will provide identical results. The process is highly transparent, as most decisions made by the researcher can be reviewed by other researchers, unlike, e.g., in the creation of coding sheets. The framework consists of three main phases: Pre-processing, Topic Modelling, and Post-Processing. In the pre-processing stage, papers are loaded, cleaned, and cross-validated, where recommendations to parameter settings are provided in the case work, as well as in the accompanied code. The topic modelling step is where the LDA method is executed, using the parameters identified in the pre-processing step. The post-processing step creates outputs from the topic model and addresses how validity can be ensured and how the exploratory literature review can be used for a full literature review. The framework was successfully used in a case with 650 papers, which was processed quickly, with little time investment from the researcher. Less than 2 days was used to process the 650 papers and group them into twenty research areas, with the use of a standard laptop. The results of the case are used in the literature review by [ 3 ].
The framework is seen to be especially relevant for junior researchers, as they often need an overview of different research fields, with little pre-existing knowledge, where the framework can enable researchers to review more papers, more frequently.
For an improved framework, two main areas need to be addressed. Firstly, the proposed framework needs to be applied by other researchers on other research fields to gain knowledge about the practicality and gain ideas for further development of the framework. Secondly, research in how to automatically identity model parameters could greatly improve the usability for the use of topic modelling for non-technical researchers, as the selection of model parameters has a great impact on the result of the framework.
Availability of data and materials
https://github.com/clausba/Smart-Literature-Review (No data).
Abbreviations
- Latent Dirichlet Allocation
supply chain management
Alghamdi R, Alfalqi K. A survey of topic modeling in text mining. Int J Adv Comput Sci Appl. 2015;6(1):7. https://doi.org/10.14569/IJACSA.2015.060121 .
Article Google Scholar
Ansolabehere S, Snowberg EC, Snyder JM. Statistical bias in newspaper reporting on campaign finance. Public Opin Quart. 2003. https://doi.org/10.2139/ssrn.463780 .
Asmussen CB, Møller C. Enabling supply chain analytics for enterprise information systems: a topic modelling literature review. Enterprise Information Syst. 2019. (Submitted To) .
Atteveldt W, Welbers K, Jacobi C, Vliegenthart R. LDA models topics… But what are “topics”? In: Big data in the social sciences workshop. 2015. http://vanatteveldt.com/wp-content/uploads/2014_vanatteveldt_glasgowbigdata_topics.pdf .
Baum D. Recognising speakers from the topics they talk about. Speech Commun. 2012;54(10):1132–42. https://doi.org/10.1016/j.specom.2012.06.003 .
Blei DM. Probabilistic topic models. Commun ACM. 2012;55(4):77–84. https://doi.org/10.1145/2133806.2133826 .
Blei DM, Lafferty JD. A correlated topic model of science. Ann Appl Stat. 2007;1(1):17–35. https://doi.org/10.1214/07-AOAS114 .
Article MathSciNet MATH Google Scholar
Blei DM, Ng AY, Jordan MI. Latent Dirichlet Allocation. J Mach Learn Res. 2003;3:993–1022. https://doi.org/10.5555/944919.944937 .
Article MATH Google Scholar
Bonilla T, Grimmer J. Elevated threat levels and decreased expectations: how democracy handles terrorist threats. Poetics. 2013;41(6):650–69. https://doi.org/10.1016/j.poetic.2013.06.003 .
Brocke JV, Mueller O, Debortoli S. The power of text-mining in business process management. BPTrends.
Denny MJ, Spirling A. Text preprocessing for unsupervised learning: why it matters, when it misleads, and what to do about it. Polit Anal. 2018;26(2):168–89. https://doi.org/10.1017/pan.2017.44 .
DiMaggio P, Nag M, Blei D. Exploiting affinities between topic modeling and the sociological perspective on culture: application to newspaper coverage of U.S. government arts funding. Poetics. 2013;41(6):570–606. https://doi.org/10.1016/j.poetic.2013.08.004 .
Elgesem D, Feinerer I, Steskal L. Bloggers’ responses to the Snowden affair: combining automated and manual methods in the analysis of news blogging. Computer Supported Cooperative Work: CSCW. Int J. 2016;25(2–3):167–91. https://doi.org/10.1007/s10606-016-9251-z .
Elgesem D, Steskal L, Diakopoulos N. Structure and content of the discourse on climate change in the blogosphere: the big picture. Environ Commun. 2015;9(2):169–88. https://doi.org/10.1080/17524032.2014.983536 .
Evans MS. A computational approach to qualitative analysis in large textual datasets. PLoS ONE. 2014;9(2):1–11. https://doi.org/10.1371/journal.pone.0087908 .
Ghosh D, Guha R. What are we “tweeting” about obesity? Mapping tweets with topic modeling and geographic information system. Cartogr Geogr Inform Sci. 2013;40(2):90–102. https://doi.org/10.1080/15230406.2013.776210 .
Grimmer J. A Bayesian hierarchical topic model for political texts: measuring expressed agendas in senate press releases. Polit Anal. 2010;18(1):1–35. https://doi.org/10.1093/pan/mpp034 .
Grimmer J, Stewart BM. Text as data: the promise and pitfalls of automatic content analysis methods for political texts. Polit Anal. 2013;21(03):267–97. https://doi.org/10.1093/pan/mps028 .
Guo L, Vargo CJ, Pan Z, Ding W, Ishwar P. Big social data analytics in journalism and mass communication. J Mass Commun Quart. 2016;93(2):332–59. https://doi.org/10.1177/1077699016639231 .
Jacobi C, Van Atteveldt W, Welbers K. Quantitative analysis of large amounts of journalistic texts using topic modelling. Digit J. 2016;4(1):89–106. https://doi.org/10.1080/21670811.2015.1093271 .
Jockers ML, Mimno D. Significant themes in 19th-century literature. Poetics. 2013;41(6):750–69. https://doi.org/10.1016/j.poetic.2013.08.005 .
Jones BD, Baumgartner FR. The politics of attention: how government prioritizes problems. Chicago: University of Chicago Press; 2005.
Google Scholar
King G, Lowe W. An automated information extraction tool for international conflict data with performance as good as human coders: a rare events evaluation design. Int Org. 2008;57:617–43. https://doi.org/10.1017/s0020818303573064 .
Koltsova O, Koltcov S. Mapping the public agenda with topic modeling: the case of the Russian LiveJournal. Policy Internet. 2013;5(2):207–27. https://doi.org/10.1002/1944-2866.POI331 .
Lancichinetti A, Irmak Sirer M, Wang JX, Acuna D, Körding K, Amaral LA. High-reproducibility and high-accuracy method for automated topic classification. Phys Rev X. 2015;5(1):1–11. https://doi.org/10.1103/PhysRevX.5.011007 .
Mahmood A. Literature survey on topic modeling. Technical Report, Dept. of CIS, University of Delaware Newark, Delaware. http://www.eecis.udel.edu/~vijay/fall13/snlp/lit-survey/TopicModeling-ASM.pdf . 2009.
Maier D, Waldherr A, Miltner P, Wiedemann G, Niekler A, Keinert A, Adam S. Applying LDA topic modeling in communication research: toward a valid and reliable methodology. Commun Methods Meas. 2018;12(2–3):93–118. https://doi.org/10.1080/19312458.2018.1430754 .
Mimno D, Blei DM. Bayesian checking for topic models. In: EMLP 11 proceedings of the conference on empirical methods in natural language processing. 2011. p 227–37. https://doi.org/10.5555/2145432.2145459
Parra D, Trattner C, Gómez D, Hurtado M, Wen X, Lin YR. Twitter in academic events: a study of temporal usage, communication, sentimental and topical patterns in 16 Computer Science conferences. Comput Commun. 2016;73:301–14. https://doi.org/10.1016/j.comcom.2015.07.001 .
Quinn KM, Monroe BL, Colaresi M, Crespin MH, Radev DR. How to analyze political attention. Am J Polit Sci. 2010;54(1):209–28. https://doi.org/10.1111/j.1540-5907.2009.00427.x .
Xu Z, Raschid L. Probabilistic financial community models with Latent Dirichlet Allocation for financial supply chains. In: DSMM’16 proceedings of the second international workshop on data science for macro-modeling. 2016. https://doi.org/10.1145/2951894.2951900 .
Zhao W, Chen JJ, Perkins R, Liu Z, Ge W, Ding Y, Zou W. A heuristic approach to determine an appropriate number of topics in topic modeling. BMC Bioinform. 2015;16(13):S8. https://doi.org/10.1186/1471-2105-16-S13-S8 .
Download references
Acknowledgements
Not applicable.
Author information
Authors and affiliations.
Department of Materials and Production, Center for Industrial Production, Aalborg University, Fibigerstræde 16, 9220, Aalborg Øst, Denmark
Claus Boye Asmussen & Charles Møller
You can also search for this author in PubMed Google Scholar
Contributions
CBA wrote the paper, developed the framework and executed the case. CM Supervised the research and developed the framework. Both authors read and approved the final manuscript.
Corresponding author
Correspondence to Claus Boye Asmussen .
Ethics declarations
Competing interests.
The authors declare that they have no competing interests.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( http://creativecommons.org/licenses/by/4.0/ ), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Reprints and permissions
About this article
Cite this article.
Asmussen, C.B., Møller, C. Smart literature review: a practical topic modelling approach to exploratory literature review. J Big Data 6 , 93 (2019). https://doi.org/10.1186/s40537-019-0255-7
Download citation
Received : 26 July 2019
Accepted : 02 October 2019
Published : 19 October 2019
DOI : https://doi.org/10.1186/s40537-019-0255-7
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Supply chain management
- Automatic literature review
A systematic exploration of scoping and mapping literature reviews
- Brief Report
- Open access
- Published: 23 May 2024
Cite this article
You have full access to this open access article

- Eirini Christou ORCID: orcid.org/0000-0001-6928-1013 1 ,
- Antigoni Parmaxi ORCID: orcid.org/0000-0002-0687-0176 1 &
- Panayiotis Zaphiris ORCID: orcid.org/0000-0001-8112-5099 1
1314 Accesses
Explore all metrics
Systematic literature mapping can help researchers identify gaps in the research and provide a comprehensive overview of the available evidence. Despite the importance and benefits of conducting systematic scoping and mapping reviews, many researchers may not be familiar with the methods and best practices for conducting these types of reviews. This paper aims to address this gap by providing a step-by-step guide to conducting a systematic scoping or mapping review, drawing on examples from different fields. This study adopts a systematic literature review approach aiming to identify and present the steps of conducting scoping and mapping literature reviews and serves as a guide on conducting scoping or mapping systematic literature reviews. A number of 90 studies were included in this study. The findings describe the steps to follow when conducting scoping and mapping reviews and suggest the integration of the card sorting method as part of the process. The proposed steps for undertaking scoping and mapping reviews presented in this manuscript, highlight the importance of following a rigorous approach for conducting scoping or mapping reviews.
Similar content being viewed by others
A scoping review on the conduct and reporting of scoping reviews.
How methodological frameworks are being developed: evidence from a scoping review

Literature Reviews: An Overview of Systematic, Integrated, and Scoping Reviews
Explore related subjects.
- Artificial Intelligence
Avoid common mistakes on your manuscript.
1 Introduction
An essential component of academic research is literature review. A systematic literature review, also known as a systematic review, is a method for locating, assessing, and interpreting all research related to a specific research question, topic, or phenomenon of interest [ 1 ].
Scoping and mapping reviews are variations of systematic literature mapping [ 2 ]. Both mapping and scoping reviews can help researchers to understand the scope and breadth of the literature in a given field, identify gaps in the research, and provide a comprehensive overview of the available evidence. Systematic literature mapping purposely focuses on a narrower but more general academic or policy issue and does not try to synthesize the results of research to address a particular subject. The scoping review is exploratory in nature, whereas the mapping review can be conclusive in describing the available evidence and identifying gaps. Mapping review includes a thorough, systematic search of a wide field. It identifies the body of literature that is currently available on a subject and points out any glaring gaps in the evidence [ 3 ].
1.1 Rationale
Despite the importance and benefits of conducting systematic scoping and mapping reviews, many researchers may not be familiar with the methods and best practices for conducting these types of reviews. This paper aims to address this gap by providing a step-by-step guide to conducting a systematic scoping or mapping review, drawing on examples from different fields.
This study adopts a systematic literature review approach aiming to identify and present the differences and the steps of conducting scoping and mapping literature review. The paper provides practical guidance on how to address common challenges in conducting systematic scoping or mapping reviews, such as dealing with the volume of studies identified, managing the data extraction and synthesis process, and ensuring rigor and reproducibility in the review methodology. The main research questions that guide this study are:
RQ1: What is a systematic scoping review and how is it conducted?
RQ2: What is a systematic mapping review and how is it conducted?
RQ3: What are the main differences between systematic scoping and systematic mapping reviews?
Overall, this paper will be a valuable resource for researchers who are interested in conducting a systematic scoping or mapping review. By providing clear guidance and practical examples, the paper aims to promote best practices in systematic scoping and mapping review methodology. The study is organized as follows: The following section presents the methodology of the study, followed by the results showing the process of the scoping and mapping literature review and presenting some examples. Finally, suggestions on how to plan and perform a quality scoping and mapping review are presented.
2 Methodology
The methodology of this paper was adopted by Xiao and Watson [ 4 ].
2.1 Literature search
The search was conducted in two well-known online databases, Web of Science and EBSCOHost, across various disciplines. The searched terms combined keywords related to the performance of scoping and mapping literature review, such as “systematic literature review”, “methodology”, “map”, “mapping” and “scoping”. The title of each manuscript was used to determine its initial relevance. If the content of the title suggested that it would explain the method of the literature review process, we obtained the full reference, which included the author, year, title, and abstract, for additional analysis.
2.2 Initial search results
The query string used for the database search is the following: systematic literature review AND methodology AND (“map” OR “mapping” OR “scoping”). Abstract search was conducted in both databases for the last 10 years (2013–2022). A search on EBSCOHost revealed 643 results of which 291 were duplicated and automatically removed. After applying the database filters to limit the articles to peer-reviewed academic journal articles written in English, a number of 102 papers were excluded. Additional 109 papers were duplicated and removed manually. After an initial screening of the titles, a total of 13 studies were identified as relevant to the methodology of the scoping and mapping literature review. A search on Web of Science, revealed 888 results of which 9 were duplicate and removed, and 157 were found to be related to the methodology of scoping or mapping literature reviews after the first title screening. Last search was conducted on the 2nd of November 2022. Both sources revealed 161 related studies, excluding 9 duplicates that were removed.
2.3 Inclusion and exclusion criteria
Only studies that provide instructions on how to perform a scoping or mapping review were included in this paper. Reviews of the literature on certain subjects and in languages other than English were excluded. The study is limited to papers published within the last 10 years, aiming to collect recent information for performing scoping or mapping reviews. Inclusion and exclusion criteria can be found in Table 1 .
2.4 Screening
To further assess the 161 studies’ applicability to the study topic, their abstracts were reviewed. The manuscripts were evaluated independently and in parallel by two researchers. The researchers’ differing opinions were discussed and settled. Then the full-text of a total of 20 studies was acquired for quality evaluation.
2.5 Eligibility and quality evaluation
To further assess the quality and relevance of the studies, the full-text papers were reviewed. Journal articles and books published by prominent publishers were included in the review as they contained high-quality research. Because there is no peer review procedure, the majority of technical reports and online presentations were excluded.
Two researchers worked independently and simultaneously on evaluating eligibility and quality. Any disagreements between them were discussed and resolved. A total of ten (10) studies were excluded after careful review: one study was excluded because it lacked instructions on how the scoping or mapping review methodology was conducted, three studies were excluded because the methodology was not related to scoping or mapping review, while five studies were disregarded because they focused on a particular subject. One of the studies’ full text couldn’t be accessed. This resulted in ten (10) eligible for full-text analysis.
2.6 Iterations
Through backward and forward searching, additional 18 studies were discovered, from which only 10 met the inclusion criteria. The forward and backward search was also used to find manuscripts that applied scoping or mapping literature review methodology. After finding the article that established the scoping or mapping review methodology, articles that had cited the methodology paper to find instances of best practices in different fields were searched. Following consideration of examples’ adherence to the methodology, preference was given to planning-related articles. In total, 90 studies were analyzed in this study, i.e. 10 methodological papers that describe the application of scoping or mapping review, as well as 80 papers that demonstrate the application of the scoping and mapping methodology in different fields, that are used as examples. The PRISMA flow diagram (see Fig. 1 ) depicts the process of the search strategy [ 5 ].
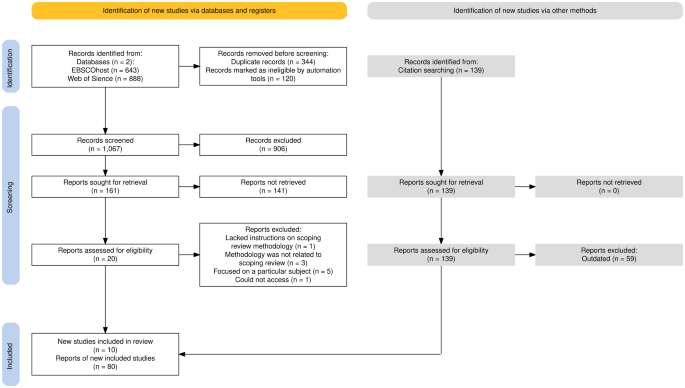
PRISMA flow diagram
2.7 Extraction and analysis of data
Data were extracted in the process of scoping literature reviews, including information with regards to formulating the problem, establishing and validating the review procedure, searching the literature, screening for inclusion, evaluating quality, extracting data, analyzing and synthesizing data, and reporting the findings (Xiao & Watson, 2019). NVivo software was used for all data extraction and coding procedures. Initially, two researchers each took information from articles for cross-checking. The two researchers reached an agreement on what to extract from the publications after reviewing a few articles together. Then the first author classified the data based on the research questions.
In this section we present the findings of our review.
3.1 Defining “Scoping” and “mapping” review
According to [ 2 ], scoping and mapping reviews are variations of systematic literature mapping that focus on narrower but more general academic or policy issues. A scoping review is exploratory in nature, seeking to identify the nature and extent of research on a particular topic, and can be used to identify gaps in the literature. An example of a research question suitable for a scoping review is “What engagement strategies do educators use in classroom settings to facilitate teaching and learning of diverse students in undergraduate nursing programs?“ [ 6 ]. A mapping review, on the other hand, is a thorough and systematic search of a wide field of literature that aims to identify the body of literature currently available on a subject and point out any glaring gaps in the evidence. An example of a research question suitable for a mapping review is “What are the currently available animal models for cystic fibrosis” [ 3 ]. Overall, each type of review has its own specific aims and can be useful for different types of research questions.
3.1.1 Defining scoping review
There is no single definition for scoping reviews in the literature. According to [ 7 ], scoping review is a type of knowledge synthesis that uses a systematic process to map the evidence on a subject and identify key ideas, theories, sources, and knowledge gaps. The goal of a scoping review is to include all relevant information that is available, including ‘grey’ literature, which includes unpublished research findings, therefore including all available literature and evidence, but the reviewers can decide what type of publications they would like to include [ 8 , 9 , 10 , 11 ].
Scoping review process is sometimes used as a preliminary step before a systematic literature review, in cases where the topic or research area in focus has not yet been extensively reviewed or is complicated or heterogeneous in nature and the types of evidence available remain unclear [ 3 ]. For example, while a scoping review might serve as the foundation for a full systematic review, it does not aim to evaluate the quality of the evidence like systematic reviews do [ 8 ]. Moreover, scoping review is also referred to as a “pilot study” [ 12 ], that can be used as a “trial run” of the entire systematic map; it helps to mold the intended approach for the review and inform the protocol development.
Rapid and scoping meta-reviews were also referred as types of scoping reviews. A “rapid review” is a particular kind of scoping review, which aims to provide an answer to a particular query and can shorten the process compared to a full systematic review [ 3 ]. The “scoping meta-review” (SMR) is a scoping evaluation of systematic reviews that offers researchers a flexible framework for field mapping and a way to condense pertinent research activities and findings, similar to a scoping review [ 13 ].
Almost all of the scoping studies identified in the corpus, draw from previews scoping review frameworks, such as the one proposed by [ 14 , 15 ] and the authors’ manual provided by the Joanna Briggs Institute [ 11 , 16 , 17 , 18 ].
3.1.2 Defining mapping review
A mapping review, also referred to as a “systematic map”, is “a high-level review with a broad research question” [ 3 ](p.133). The mapping review includes a thorough, systematic search of a wide field. It identifies the body of literature that is currently available on a subject and points out any gaps in the evidence. The mapping review can be conclusive in describing the available evidence and identifying gaps, whereas the scoping review is exploratory in nature [ 3 ].
The term “mapping” is used to describe the process of synthesizing and representing the literature numerically and thematically in tables, figures, or graphical representations, which can be thought of as the review output. Mapping enables researchers to pinpoint potential areas for further study as well as gaps in the literature [ 19 ].
Systematic mapping uses the same strict procedures as systematic reviews do. However, systematic mapping can be used to address open or closed-framed questions on broad or specific topics, because it is not constrained by the requirement to include fully specified and defined key elements [ 12 ]. Systematic mapping is especially useful for broad, multifaceted questions about an interesting topic that might not be appropriate for systematic review because they involve a variety of interventions, populations, or outcomes, or because they draw on evidence that is not just from primary research [ 12 ].
3.2 Process of conducting mapping and scoping reviews
As noted in the previous sections, mapping reviews and scoping reviews both aim to provide a broad overview of the literature, but the former focuses on the scope of the literature while the latter focuses on the nature and extent of available evidence on a specific research question or topic. In understanding the process for conducting mapping and scoping reviews, we adopted the eight steps proposed by Xiao and Watson [ 4 ] that are common for all types of reviews: (1) Formulate the problem; (2) Establishing and validating the review procedure; (3) Searching the literature; (4) Screening for inclusion; (5) Evaluating quality; (6) Extracting data; (7) Analyzing and synthesizing data; (8) Reporting the findings. The steps are explained in detail below and describe the methodology for both scoping and mapping reviews, distinguishing their differences where applicable. A summary of the review types along with their characteristics and steps as identified from the literature are presented in Table 2 .
3.2.1 Step 1 formulate the problem
The first step for undertaking a mapping or a scoping review is to formulate the problem by setting the research question that should be investigated, taking into account the topic’s scope [ 12 ]. It is important to clearly state the review objectives and specific review questions for the scoping review. The objectives should indicate what the scoping review is trying to achieve [ 10 , 20 ].
In mapping reviews, it can be helpful to create a conceptual framework or model (visual or textual) to describe what will be explored by the map when determining the mapping review’s scope. It should also be determined whether the topic’s scope is broad, specific, or likely to be supported by a substantial body of evidence [ 12 ].
3.2.1.1 Defining the research question(s)
Prior to beginning their search and paper selection process, the authors should typically define their research question(s) [ 3 ]. There are specific formats that are recommended for structuring the research question(s), as well as the exclusion and inclusion criteria of mapping and scoping reviews [ 21 ] (see Table 3 ).
PCC (Population, Concept, and Context) and PICO format (Population, Intervention, Comparator and Outcome) are often used in scoping and mapping reviews. It is recommended that research questions for scoping reviews follow the PCC format and include all of its components [ 17 , 18 , 21 ]. Information about the participants (e.g. age), the principal idea or “concept,” and the setting of the review, should all be included in the research question. The context should be made explicit and may take into account geographical or locational considerations, cultural considerations, and particular racial or gender-based concerns [ 10 ].
Researchers use the PCC format in order to determine the eligibility of their research questions, as well as to define their inclusion criteria (e.g [ 22 , 23 , 24 , 25 , 26 ]). Most scoping reviews have a single main question, but some of them are better served by one or more sub-questions that focus on specific PCC characteristics [ 8 , 18 ].
3.2.2 Step 2. Establishing and validating the review procedure
A protocol is crucial for scoping and mapping reviews because it pre-defines the scoping review’s goals and procedures [ 11 , 17 , 18 , 20 ], it clearly states all methodological decisions since the very beginning [ 2 ], and it also specifies the strategy to be used at each stage of the review process [ 12 ]. Similar to all systematic reviews, scoping reviews start with the creation of an a-priori protocol that includes inclusion and exclusion criteria that are directly related to the review’s objectives and questions [ 7 , 11 , 17 , 18 , 20 ]. In order to decrease study duplication and improve data reporting transparency, the use of formalized, registered protocols is suggested [ 18 , 19 ]. The international prospective register of systematic reviews, known as PROSPERO, states that scoping reviews (and literature reviews) are currently ineligible for registration in the database. While this could change in the future, scoping reviews can currently be registered with the Open Science Framework ( https://osf.io/ ) or Figshare ( https://figshare.com/ ), and their protocols can be published in select publications, including the JBI Evidence Synthesis [ 18 ].
Scoping and mapping reviews should require at least two reviewers in order to minimize reporting bias, as well as to ensure consistency and clarity [ 3 , 16 , 17 , 18 ]. The reviewers should include a plan for the results presentation during the protocol development, such as a draft chart or table that could be improved at the end when the reviewers become more familiar with the information they have included in the review [ 17 , 18 ].
3.2.3 Step 3. Searching the literature
Searching the literature requires to prepare a search strategy, decide on search terms, search databases or journals, and perform a manual search [ 27 ]. For example, deciding on search terms, can follow an iterative process that is further explained in the sub-section below. Thinking about searching in terms of broader to narrower strategies is helpful. Fewer databases and/or journals will be checked out in narrower searches (search only in the title, keywords, and abstract fields), which are frequently used in scoping reviews, while multiple databases can be checked for mapping reviews [ 2 ].
Search strategy
Mapping and scoping review search should aim to be as thorough as possible [ 12 ] to find both published and unpublished evidence. An inclusive approach is frequently preferred for scoping reviews to prevent potential omission of crucial information [ 10 , 17 , 18 ].
According to JBI, there should be a three-step search process for scoping reviews [ 10 , 17 , 18 ]. The first step is a quick search of at least two databases followed by a text word check of the article’s title, abstract, and body of text that are then analyzed. All determined index terms and keywords are used in the second stage across all included databases. In the third stage, additional studies should be looked up in the identified reports and articles’ reference lists [ 10 , 11 , 18 ]. The reviewers may look solely at the reference lists of the studies that were chosen from the full-text and/or included in the review, or they may look at the reference lists of all identified studies. In any case, it needs to be made very clear which group of studies will be looked at [ 8 , 11 , 18 ]. As reviewers gain more familiarity with the body of available evidence, new keywords, sources, and possibly helpful search terms may be found and incorporated into the search strategy, hence the search for a scoping review may be quite iterative. If so, it is crucial that the entire search process and the outcomes are open to scrutiny and audit [ 11 , 18 ].
In the same line, it is recommended for mapping reviews to search multiple databases [ 2 ] in all pertinent searchable fields (e.g., title, abstract, keywords, etc.) [ 3 ]. Thematic keywords, along with all of their synonyms and regional/temporal variations, are joined together to form Boolean strings using Boolean signs. Building looser, multiple Boolean strings instead of well-targeted ones (for example, using OR instead of AND, NOT, and exact phrases, respectively) is preferable. The latter runs the risk of omitting crucial references, whereas the former may return a sizable sample of sparsely relevant references [ 2 ]. Focusing the search on a specific component and then filtering all the results can be more effective for mapping reviews [ 3 ].
3.2.4 Step 4. Screening for inclusion
Screening and choosing the studies to be included in a review are the main objectives of this phase. According to [ 27 ], there are two levels of screening. Titles and abstracts are scanned in the first level to limit the range of the studies to be included, while full texts are scanned in the second level to re-examine the relevance of the studies and to settle disagreements between reviewers regarding the study selection. Discussions, meetings, consulting a third reviewer, and determining inter-rater reliability/agreement (using Cohen’s kappa coefficient or intraclass correlation coefficient) are the most typical ways to resolve disagreements. Soaita et al. (2020) [ 2 ] also support that the sample of retrieved references should be ‘cleaned-up’ once it has been finalized and duplicates have been automatically removed.
Different methodological approaches, including primary research articles, summary articles, opinion pieces, and grey literature, can all be included in the literature that scoping reviews identify and analyze [ 7 , 18 , 19 ], but they may also serve as an exclusion criterion [ 2 ]. Peters, Godfrey, et al. (2020) [ 18 ] advice against limiting source inclusion based on language unless there are compelling justifications for doing so (such as practical considerations).
According to the PRISMA extension for scoping reviews (PRISMA-ScR), a description of the study selection process must be provided in both a narrative and flow diagram format. Including the date of the most recent literature search, enables the reader to assess how current the scoping review is [ 7 ].
3.2.4.1 Inclusion and exclusion criteria
Inclusion criteria offer a framework on which the reviewers can decide which sources to include in the scoping review. To ensure transparency and replicability, the exclusion and inclusion criteria need to be documented [ 7 , 8 , 10 , 11 , 17 ]. Authors should specify any limitations by year, language, publication status, or other factors, and explain why each one was put in place [ 7 ].
When it comes to mapping reviews, criteria should be created whenever possible with participation from stakeholders. Depending on the type of research questions, stakeholders may include practitioners, designers, policy makers, scientists and research funding bodies, but attention should be paid to avoid bias [ 12 ].
3.2.5 Step 5. Evaluating quality
Scoping and mapping reviews are not concerned with quality assessment as a criterion for inclusion [ 2 ]. Assessments of reporting quality and bias risk are typically outside the scope. Although it is possible to extract study characteristics that reflect study and reporting quality, bias cannot be assessed against a specific hypothesis if a mapping review is exploratory [ 3 ].
3.2.6 Step 6. Extracting data
The process of data extraction for a scoping review is also known as “charting the results”. A draft charting table or form needs to be created to capture the key details about the relevance of the included studies to the review question, as well as the characteristics of the included studies. The data extraction process can be iterative, with the charting table being constantly updated.
The reviewers should become familiar with the source results and test the extraction form on two or three studies to ensure that all relevant results are extracted [ 7 , 8 , 10 , 11 , 17 , 18 , 28 ]. In order to increase reporting transparency, authors should explain the main revisions with a justification if the charting process was iterative (i.e., the form was continuously updated). If appropriate, details about the procedures used to collect and verify information from the researchers of the included sources of evidence should be provided [ 7 ]. Author(s), year of publication, source origin, country of origin, objectives, purpose, study population, sample size, methodology, intervention type and comparator, concept, duration of the intervention, how outcomes are measured, and key findings that are related to the review question are all types of information that may be extracted [ 7 , 8 , 10 , 11 , 17 ].
When it comes to data extraction for mapping reviews, it is restricted to important study characteristics and outcomes due to the size of a mapping review [ 3 ]. The process of mapping is intended to produce a practical and organized resource that provides enough detail about studies to be helpful in further work [ 12 ].
To move beyond a straightforward list of citations, it is crucial to maintain a high level of clarity throughout any databases that are created. Studies that are discussed in several papers or that seem to be connected should be marked in the database. In the future, this helps prevent the double counting of research findings in syntheses that might overlook connections between study lines in the databases [ 12 ].
Aiming to capture the key characteristics of the included studies in the scoping and mapping reviews, we suggest the use of a guiding table for extracting data (see Supplementary_Material_1_Guiding_Table).
3.2.7 Step 7. Analyzing and synthesizing data
Authors may extract results and map descriptively. Simple frequency counts of concepts, populations, characteristics, or other fields of data will suffice for many scoping reviews [ 17 , 18 ]. In-depth analysis of quantitative data is not typically required in scoping reviews, although in some cases the authors may take into consideration a more advanced analysis depending on the nature and purpose of their review. A meta-analysis or interpretive qualitative analysis is probably not necessary in scoping reviews [ 17 , 18 ].
When it comes to mapping reviews, no results synthesis is carried out [ 12 ]. Different analytical approaches can be used to map chronological, geographical, conceptual, and thematic trends, which include some form of coding, once the sample has been limited to the pertinent references [ 2 ]. It is possible to identify correlations, trends, gaps, and clusters using simple numerical accounts of frequencies in each category (for example, the number of studies looking at a specific species) and more complex cross-tabulations (for instance, the number of studies looking at the effectiveness of a specific intervention, in a particular farming system, for a named species). Users have access to the map and can query it to find information pertaining to any chosen combinations of the subsets of the meta-data [ 12 ].
3.2.8 Step 8. Reporting the findings
Authors should specify exactly how the evidence will be presented, whether it be in a narrative format, table, or visual representation, such as a map or diagram [ 7 ].
In scoping reviews, a summary of all the relevant information gathered can be presented [ 8 ] using a logical and descriptive summary of the findings based on the research questions [ 10 , 11 , 17 ]. The distribution of studies by year or period of publication, countries of origin, field of intervention, and research methodologies, may be displayed in the tables and charts accompanied with a narrative summary that explains how the results relate to the review’s objectives [ 7 , 11 , 17 , 18 ].
The conclusions should be consistent with the review objective or question based on the findings of the scoping review [ 10 ]. Following the conclusions, specific recommendations for future research based on gaps in knowledge identified by the review results can be presented. Because of the lack of a methodological quality appraisal, recommendations for practice may be unable to be developed; however, suggestions based on the conclusions may be made [ 10 ].
A scoping review’s results section should include a PRISMA flow diagram and details the outcomes of the search strategy and selection procedure [ 7 , 17 ] outlining the grounds for exclusion at the full-text level of screening [ 7 ]. For example, a study [ 29 ] used the PRISMA-ScR extension for scoping reviews to ensure all important sections have been covered in their review.
Mapping reviews may place more emphasis on describing the evidence. The use of pivot tables and pivot charts is helpful for quickly visualizing the amount (and quality, if it is measured) of evidence across a variety of meta-data variables [ 12 ]. Such visualizations can display the quantity of research, the conclusions of a critical appraisal, the sample size across nations, outcomes, populations, or variables. These visualizations can contain categorical variables as additional dimensions. The geographic distribution of study effort and type may be particularly important in mapping reviews with a global or large-scale reach [ 12 ].
4 Discussion
This systematic literature review aimed to describe the process of conducting mapping and scoping literature reviews. In summary, the main difference between the two types of reviews is in their focus and scope. Mapping reviews provide a comprehensive overview of the literature while scoping reviews identify gaps and inconsistencies in the literature and outline potential areas for future research.
A lot of the methodological papers included in this systematic literature review (e.g [ 10 , 19 , 28 ]), referred to the “consultation process” as an additional, optional step that has been suggested by [ 14 ]. In this stage, subject experts or potential review users like practitioners, consumers, and policymakers may be consulted [ 8 ]. Researchers argue that this step should be mandatory [ 15 , 28 ]. In agreement with Levac et al.’s [ 15 ] choice, Daudt et al. [ 28 ] encourage the use of the consultation stage whenever it is practical because it adds richness to the entire research process and, consequently, the findings. Despite the fact that stakeholder consultations can make scoping review planning and execution more difficult, they guarantee that the findings are pertinent to educational practice and/or policies [ 19 ].
Scoping and mapping reviews should require more than one author to eliminate bias and ensure their quality. The card-sorting technique is suggested to be employed within the review process as a means for resolving discrepancies between the stakeholders and come to an agreement on the categorization and evaluation of the data to be included. Other studies (e.g [ 30 , 31 , 32 , 33 ]), propose the card-sorting technique as a method for resolving disagreements between people’s disparities, as well as to evaluate and verify extracted themes from datasets. Card sorting is a quick and reliable sorting method that finds patterns in how users would expect to find content or functionality. Due to the patterns and insights it exposes about how people organize and categorize content, card sorting is a successful approach for resolving categorization disagreements [ 34 ]. According to Wood and Wood [ 35 ], the majority of card sorting projects involve an open sort, where participants receive a list of items and are asked to organize them in the most appropriate way. However, in some cases, a pre-existing set of categories is given to the participants, the so-called closed card sorting project. This assumes that the existing categories are already well-organized, and the goal is to make minor adjustments. Wood and Wood [ 35 ], suggest that it’s best to start with an open sort and analyze the data before conducting a closed sort for validation. If a closed sort is necessary, it should be kept simple, and the results may not be optimal. For example, in a study [ 30 ] that aimed to review the use of makerspaces for educational purposes, the card sorting technique was used for the development of the coding scheme. A three-member academic committee, consisting of three professors took part in the card sorting exercise where they went through the abstracts of the relevant papers and were asked to categorize each manuscript after discussion. They then categorized the manuscripts in the three major themes and 11 subcategories that emerged during the card sorting exercise [ 30 ]. Similarly, the authors of [ 31 ] employed the card sorting technique in their research in order to agree on the main categorization and sub-categorization of the articles identified for inclusion in their review. Card sorting can be integrated as an additional step when conducting scoping and mapping reviews, as it provides useful insights from the experts’ perspective and makes the mapping process more inclusive (see Fig. 2 ).

Proposed steps for conducting scoping and mapping reviews
5 Conclusion
Scoping and mapping reviews need a methodological framework that is rigorous, consistent, and transparent, so that the results can be trusted and the review replicated. This provides enough information for the readers to evaluate the review’s accuracy, relevance, and thoroughness [ 8 ]. Scoping reviews should be carried out in accordance with established methodological guidance and reported using reporting standards (like PRISMA-ScR) guidelines [ 36 ]. The proposed steps for undertaking scoping and mapping reviews presented in this manuscript, highlight the importance of following a rigorous approach for conducting scoping or mapping reviews. Overall, this paper is a valuable resource for researchers who are interested in conducting a systematic scoping or mapping review in different fields and are looking to apply these review methods to their own research questions.
5.1 Limitations and future work
This study does not lack limitations. As specific keywords and specific databases were searched, not all relevant work is included. The study was also limited to the past 10 years, letting out methodologies and frameworks for scoping and mapping literature reviews that were not published within the specific timeframe. The fact that the number of methodological papers identified for inclusion are limited to ten, makes it difficult to clarify the differences between mapping and scoping reviews. Therefore, further research is encouraged in order to clarify and verify the differences and similarities between the two. The application of the proposed process for conducting systematic scoping and mapping reviews on specific topics will verify the process.
Data availability
The data that support the findings of this study are available from the corresponding author, [EC], upon reasonable request.
Kitchenham, B., Charters, S.: Guidelines for performing Systematic Literature Reviews in Software Engineering, (2007). https://doi.org/10.1109/ACCESS.2016.2603219
Soaita, A.M., Serin, B., Preece, J.: A methodological quest for systematic literature mapping. Int. J. Hous. Policy. 20 , 320–343 (2020). https://doi.org/10.1080/19491247.2019.1649040
Article Google Scholar
Leenaars, C., Tsaioun, K., Stafleu, F., Rooney, K., Meijboom, F., Ritskes-Hoitinga, M., Bleich, A.: Reviewing the animal literature: How to describe and choose between different types of literature reviews. Lab. Anim. 55 , 129–141 (2021). https://doi.org/10.1177/0023677220968599
Xiao, Y., Watson, M.: Guidance on conducting a systematic literature review. J. Plan. Educ. Res. 39 , 93–112 (2019). https://doi.org/10.1177/0739456X17723971
Haddaway, N.R., Page, M.J., Pritchard, C.C., McGuinness, L.A.: PRISMA: An R package and Shiny app for producing PRISMA 2020-compliant flow diagrams, with interactivity for optimised digital transparency and Open Synthesis, Campbell Syst. Rev. 18 (2022). (2020). https://doi.org/10.1002/CL2.1230
Iduye, D., Vukic, A., Waldron, I., Price, S., Sheffer, C., McKibbon, S., Dorey, R., Yu, Z.: Educators’ strategies for engaging diverse students in undergraduate nursing education programs: A scoping review protocol. JBI Evid. Synth. 19 , 1178–1185 (2021). https://doi.org/10.11124/JBIES-20-00039
Tricco, A.C., Lillie, E., Zarin, W., O’Brien, K.K., Colquhoun, H., Levac, D., Moher, D., Peters, M.D.J., Horsley, T., Weeks, L., Hempel, S., Akl, E.A., Chang, C., McGowan, J., Stewart, L., Hartling, L., Aldcroft, A., Wilson, M.G., Garritty, C., Lewin, S., Godfrey, C.M., MacDonald, M.T., Langlois, E.V., Soares-Weiser, K., Moriarty, J., Clifford, T., Tunçalp, Ö., Straus, S.E.: PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Ann. Intern. Med. 169 , 467–473 (2018). https://doi.org/10.7326/M18-0850/SUPPL_FILE/M18-0850_SUPPLEMENT.PDF
McKinstry, C., Brown, T., Gustafsson, L.: Scoping reviews in occupational therapy: The what, why, and how to. Aust Occup. Ther. J. 61 , 58–66 (2014). https://doi.org/10.1111/1440-1630.12080 WE - Science Citation Index Expanded (SCI-EXPANDED)
Peterson, J., Pearce, P.F., Ferguson, L.A., Langford, C.A.: Understanding scoping reviews: Definition, purpose, and process. J. Am. Assoc. Nurse Pract. 29 , 12–16 (2017). https://doi.org/10.1002/2327-6924.12380
Khalil, H., Peters, M., Godfrey, C.M., McInerney, P., Soares, C.B., Parker, D.: An evidence-based Approach to Scoping Reviews. Worldviews Evidence-Based Nurs. 13 , 118–123 (2016)
Peters, M.D.J., Godfrey, C., McInerney, P., Munn, Z., Trico, A., Khalil, H.: Chap. 11: Scoping reviews, in: JBI Man. Evid. Synth. JBI. (2017). https://doi.org/10.46658/JBIMES-20-12
James, K.L., Randall, N.P., Haddaway, N.R.: A methodology for systematic mapping in environmental sciences. Environ. Evid. 5 , 1–13 (2016). https://doi.org/10.1186/s13750-016-0059-6
Sarrami-Foroushani, P., Travaglia, J., Debono, D., Clay-Williams, R., Braithwaite, J.: Scoping Meta-review: Introducing a New Methodology. Clin. Transl Sci. 8 , 77–81 (2015). https://doi.org/10.1111/CTS.12188
Arksey, H., O’malley, L.: Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 8 , 19–32 (2005). https://doi.org/10.1080/1364557032000119616
Levac, D., Colquhoun, H., O’Brien, K.K.: Scoping studies: Advancing the methodology. Implement. Sci. 5 , 1–9 (2010). https://doi.org/10.1017/cbo9780511814563.003
Peters, M., Godfrey, C., McInerney, P., Soares, C., Parker, K.H.D.: Chap. 11: Scoping reviews. In: Aromataris, E., Munn, Z. (eds.) JBI Rev. Man. JBI, Adelaide (2015)
Google Scholar
Peters, M.D.J., Marnie, C., Tricco, A.C., Pollock, D., Munn, Z., Alexander, L., McInerney, P., Godfrey, C.M., Khalil, H.: Updated methodological guidance for the conduct of scoping reviews. JBI Evid. Synth. 18 , 2119–2126 (2020). https://doi.org/10.11124/JBIES-20-00167 WE - Emerging Sources Citation Index (ESCI)
Peters, M.D.J., Godfrey, C., McInerney, P., Munn, Z., Trico, A., Khalil, H.: Chap. 11: Scoping Reviews, JBI Man. Evid. Synth. (2020). https://doi.org/10.46658/JBIMES-20-12
Thomas, A., Lubarsky, S., Durning, S.J., Young, M.E.: Knowledge syntheses in medical education: Demystifying scoping reviews. Acad. Med. 92 , 161–166 (2017). https://doi.org/10.1097/ACM.0000000000001452
Peters, M.D.J., Godfrey, C.M., Khalil, H., McInerney, P., Parker, D., Soares, C.B.: Guidance for conducting systematic scoping reviews. Int. J. Evid. Based Healthc. 13 , 141–146 (2015). https://doi.org/10.1097/XEB.0000000000000050
Sager, M., Pistone, I.: Mismatches in the production of a scoping review: Highlighting the interplay of (in)formalities. J. Eval Clin. Pract. 25 , 930–937 (2019). https://doi.org/10.1111/jep.13251
Balsiger, F., Wagner, B., Jende, J.M.E., Marty, B., Bendszus, M., Scheidegger, O., Kurz, F.T.: Methodologies and MR parameters in quantitative magnetic resonance neurography: A scoping review protocol. METHODS Protoc. 5 (2022). https://doi.org/10.3390/mps5030039 WE - Emerging Sources Citation Index (ESCI)
Kesztyus, D., Brucher, S., Kesztyus, T.: Use of infrared thermography in medical diagnostics: A scoping review protocol. BMJ Open. 12 (2022). https://doi.org/10.1136/bmjopen-2021-059833 WE - Science Citation Index Expanded (SCI-EXPANDED)
Olaniyi, A.A., Ncama, B.P., Amod, H.: Mapping evidence of neonatal resuscitation training on the practices of Unskilled Birth attendants in Low-Resource Countries: Protocol for a scoping review. JMIR Res. Protoc. 10 (2021). https://doi.org/10.2196/18935 WE - Emerging Sources Citation Index (ESCI)
Rosca, E.C., Tudor, R., Cornea, A., Simu, M.: Parkinson’s Disease in Romania: A scoping review protocol. BRAIN Sci. 11 (2021). https://doi.org/10.3390/brainsci11020251 WE - Science Citation Index Expanded (SCI-EXPANDED)
Walker, K., Asoodar, M., Rudolph, J., Meguerdichian, M., Yusaf, T., Campbell-Taylor, K., van Merrienboer, J.: Optimising expert dyad performance in acute care settings: A scoping review protocol. BMJ Open. 11 (2021). https://doi.org/10.1136/bmjopen-2020-047260 WE - Science Citation Index Expanded (SCI-EXPANDED)
Chong, S.W., Lin, T.J., Chen, Y.: A methodological review of systematic literature reviews in higher education: Heterogeneity and homogeneity. Educ. Res. Rev. 35 (2022). https://doi.org/10.1016/j.edurev.2021.100426
Daudt, H.M.L., Van Mossel, C., Scott, S.J.: Enhancing the scoping study methodology: A large, inter-professional team’s experience with Arksey and O’Malley’s framework. BMC Med. Res. Methodol. 13 , 1–9 (2013). https://doi.org/10.1186/1471-2288-13-48
Qiu, Y.J., Osadnik, C.R., Team, V., Weller, C.D.: Physical activity as an Adjunct to Compression Therapy on Healing outcomes and recurrence in patients with venous Leg ulcers: A scoping review protocol. Front. Med. 8 (2021). https://doi.org/10.3389/fmed.2021.614059 WE - Science Citation Index Expanded (SCI-EXPANDED)
Konstantinou, D., Parmaxi, A., Zaphiris, P.: Mapping research directions on makerspaces in education, EMI. Educ. Media Int. 58 , 223–247 (2021). https://doi.org/10.1080/09523987.2021.1976826
Pallaris, G., Zaphiris, P., Parmaxi, A.: Mapping the landscape of Makerspaces in higher education: An inventory of research findings. Interact. Technol. Smart Educ. (2022). https://doi.org/10.1108/ITSE-01-2022-0013
Parmaxi, A., Zaphiris, P., Papadima-Sophocleous, S., Ioannou, A.: Mapping the landscape of computer-assisted language learning: An inventory of research. Interact. Technol. Smart Educ. 10 (2013). https://doi.org/10.1108/ITSE-02-2013-0004
Parmaxi, A., Zaphiris, P.: Computer-mediated communication in computer-assisted language learning: Implications for culture-centered design. Univers. Access. Inf. Soc. 15 , 169–177 (2016). https://doi.org/10.1007/S10209-015-0405-4/TABLES/3
Morville, P., Rosenfeld, L.: Information architecture for the World Wide Web: Designing large-scale web sites, (2006). https://books.google.com/books?hl=en&lr=&id=2d2Ry2hZc2MC&oi=fnd&pg=PR5&dq=Morville+%26+Rosenfeld,+2007&ots=opbfyu0ODb&sig=cAyUSw0mmdVRYf5ARSNp6DaYYLA (accessed January 17, 2024)
Wood, J.R., Wood, L.E.: Card sorting: Current practices and beyond. J. Usability Stud. 4 , 1–6 (2008). http://usabilityprofessionals.org/upa_publications/jus/2008november/JUS_Wood_Nov2008.pdf
Munn, Z., Pollock, D., Khalil, H., Alexander, L., Mclnerney, P., Godfrey, C.M., Peters, M., Tricco, A.C.: What are scoping reviews? Providing a formal definition of scoping reviews as a type of evidence synthesis. JBI Evid. Synth. 20 , 950–952 (2022). https://doi.org/10.11124/JBIES-21-00483 WE - Emerging Sources Citation Index (ESCI)
Download references
Acknowledgements
This work has been supported through funding from the Cyprus University of Technology.
Open access funding provided by the Cyprus Libraries Consortium (CLC).
Author information
Authors and affiliations.
Cyprus University of Technology, Limassol, Cyprus
Eirini Christou, Antigoni Parmaxi & Panayiotis Zaphiris
You can also search for this author in PubMed Google Scholar
Contributions
E.C. and A.P. wrote the main manuscript text. All authors contributed and agreed on the methodology to be followed. A.P. and E.C. screened and decided on the papers to be included in the study. All authors reviewed the manuscript.
Corresponding author
Correspondence to Eirini Christou .
Ethics declarations
Competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Christou, E., Parmaxi, A. & Zaphiris, P. A systematic exploration of scoping and mapping literature reviews. Univ Access Inf Soc (2024). https://doi.org/10.1007/s10209-024-01120-3
Download citation
Accepted : 15 May 2024
Published : 23 May 2024
DOI : https://doi.org/10.1007/s10209-024-01120-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Scoping review
- Mapping review
- Review methodology
- Systematic literature mapping
- Card sorting
- Find a journal
- Publish with us
- Track your research
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Int J Med Educ
Factor Analysis: a means for theory and instrument development in support of construct validity
Mohsen tavakol.
1 School of Medicine, Medical Education Centre, the University of Nottingham, UK
Angela Wetzel
2 School of Education, Virginia Commonwealth University, USA
Introduction
Factor analysis (FA) allows us to simplify a set of complex variables or items using statistical procedures to explore the underlying dimensions that explain the relationships between the multiple variables/items. For example, to explore inter-item relationships for a 20-item instrument, a basic analysis would produce 400 correlations; it is not an easy task to keep these matrices in our heads. FA simplifies a matrix of correlations so a researcher can more easily understand the relationship between items in a scale and the underlying factors that the items may have in common. FA is a commonly applied and widely promoted procedure for developing and refining clinical assessment instruments to produce evidence for the construct validity of the measure.
In the literature, the strong association between construct validity and FA is well documented, as the method provides evidence based on test content and evidence based on internal structure, key components of construct validity. 1 From FA, evidence based on internal structure and evidence based on test content can be examined to tell us what the instrument really measures - the intended abstract concept (i.e., a factor/dimension/construct) or something else. Establishing construct validity for the interpretations from a measure is critical to high quality assessment and subsequent research using outcomes data from the measure. Therefore, FA should be a researcher’s best friend during the development and validation of a new measure or when adapting a measure to a new population. FA is also a useful companion when critiquing existing measures for application in research or assessment practice. However, despite the popularity of FA, when applied in medical education instrument development, factor analytic procedures do not always match best practice. 2 This editorial article is designed to help medical educators use FA appropriately.
The Applications of FA
The applications of FA depend on the purpose of the research. Generally speaking, there are two most important types of FA: Explorator Factor Analysis (EFA) and Confirmatory Factor Analysis (CFA).
Exploratory Factor Analysis
Exploratory Factor Analysis (EFA) is widely used in medical education research in the early phases of instrument development, specifically for measures of latent variables that cannot be assessed directly. Typically, in EFA, the researcher, through a review of the literature and engagement with content experts, selects as many instrument items as necessary to fully represent the latent construct (e.g., professionalism). Then, using EFA, the researcher explores the results of factor loadings, along with other criteria (e.g., previous theory, Minimum average partial, 3 Parallel analysis, 4 conceptual meaningfulness, etc.) to refine the measure. Suppose an instrument consisting of 30 questions yields two factors - Factor 1 and Factor 2. A good definition of a factor as a theoretical construct is to look at its factor loadings. 5 The factor loading is the correlation between the item and the factor; a factor loading of more than 0.30 usually indicates a moderate correlation between the item and the factor. Most statistical software, such as SAS, SPSS and R, provide factor loadings. Upon review of the items loading on each factor, the researcher identifies two distinct constructs, with items loading on Factor 1 all related to professionalism, and items loading on Factor 2 related, instead, to leadership. Here, EFA helps the researcher build evidence based on internal structure by retaining only those items with appropriately high loadings on Factor 1 for professionalism, the construct of interest.
It is important to note that, often, Principal Component Analysis (PCA) is applied and described, in error, as exploratory factor analysis. 2 , 6 PCA is appropriate if the study primarily aims to reduce the number of original items in the intended instrument to a smaller set. 7 However, if the instrument is being designed to measure a latent construct, EFA, using Maximum Likelihood (ML) or Principal Axis Factoring (PAF), is the appropriate method. 7 These exploratory procedures statistically analyze the interrelationships between the instrument items and domains to uncover the unknown underlying factorial structure (dimensions) of the construct of interest. PCA, by design, seeks to explain total variance (i.e., specific and error variance) in the correlation matrix. The sum of the squared loadings on a factor matrix for a particular item indicates the proportion of variance for that given item that is explained by the factors. This is called the communality. The higher the communality value, the more the extracted factors explain the variance of the item. Further, the mean score for the sum of the squared factor loadings specifies the proportion of variance explained by each factor. For example, assume four items of an instrument have produced Factor 1, factor loadings of Factor 1 are 0.86, 0.75, 0.66 and 0.58, respectively. If you square the factor loading of items, you will get the percentage of the variance of that item which is explained by Factor 1. In this example, the first principal component (PC) for item1, item2, item3 and item4 is 74%, 56%, 43% and 33%, respectively. If you sum the squared factor loadings of Factor 1, you will get the eigenvalue, which is 2.1 and dividing the eigenvalue by four (2.1/4= 0.52) we will get the proportion of variance accounted for Factor 1, which is 52 %. Since PCA does not separate specific variance and error variance, it often inflates factor loadings and limits the potential for the factor structure to be generalized and applied with other samples in subsequent study. On the other hand, Maximum likelihood and Principal Axis Factoring extraction methods separate common and unique variance (specific and error variance), which overcomes the issue attached to PCA. Thus, the proportion of variance explained by an extracted factor more precisely reflects the extent to which the latent construct is measured by the instrument items. This focus on shared variance among items explained by the underlying factor, particularly during instrument development, helps the researcher understand the extent to which a measure captures the intended construct. It is useful to mention that in PAF, the initial communalities are not set at 1s, but they are chosen based on the squared multiple correlation coefficient. Indeed, if you run a multiple regression to predict say item1 (dependent variable) from other items (independent variables) and then look at the R-squared (R2), you will see R2 is equal to the communalities of item1 derived from PAF.
Confirmatory Factor Analysis
When prior EFA studies are available for your intended instrument, Confirmatory Factor Analysis extends on those findings, allowing you to confirm or disconfirm the underlying factor structures, or dimensions, extracted in prior research. CFA is a theory or model-driven approach that tests how well the data “fit” to the proposed model or theory. CFA thus departs from EFA in that researchers must first identify a factor model before analysing the data. More fundamentally, CFA is a means for statistically testing the internal structure of instruments and relies on the maximum likelihood estimation (MLE) and a different set of standards for assessing the suitability of the construct of interest. 7 , 8
Factor analysts usually use the path diagram to show the theoretical and hypothesized relationships between items and the factors to create a hypothetical model to test using the ML method. In the path diagram, circles or ovals represent factors. A rectangle represents the instrument items. Lines (→ or ↔) represent relationships between items. No line, no relationship. A single-headed arrow shows the causal relationship (the variable that the arrowhead refers to is the dependent variable), and a double-headed shows a covariance between variables or factors.
If CFA indicates the primary factors, or first-order factors, produced by the prior PAF are correlated, then the second-order factors need to be modelled and estimated to get a greater understanding of the data. It should be noted if the prior EFA applied an orthogonal rotation to the factor solution, the factors produced would be uncorrelated. Hence, the analysis of the second-order factors is not possible. Generally, in social science research, most constructs assume inter-related factors, and therefore should apply an oblique rotation. The justification for analyzing the second-order factors is that when the correlations between the primary factors exist, CFA can then statistically model a broad picture of factors not captured by the primary factors (i.e., the first-order factors). 9 The analysis of the first-order factors is like surveying mountains with a zoom lens binoculars, while the analysis of the second-order factors uses a wide-angle lens. 10 Goodness of- fit- tests need to be conducted when evaluating the hypothetical model tested by CFA. The question is: does the new data fit the hypothetical model? However, the statistical models of the goodness of- fit- tests are complex, and extend beyond the scope of this editorial paper; thus,we strongly encourage the readers consult with factors analysts to receive resources and possible advise.
Conclusions
Factor analysis methods can be incredibly useful tools for researchers attempting to establish high quality measures of those constructs not directly observed and captured by observation. Specifically, the factor solution derived from an Exploratory Factor Analysis provides a snapshot of the statistical relationships of the key behaviors, attitudes, and dispositions of the construct of interest. This snapshot provides critical evidence for the validity of the measure based on the fit of the test content to the theoretical framework that underlies the construct. Further, the relationships between factors, which can be explored with EFA and confirmed with CFA, help researchers interpret the theoretical connections between underlying dimensions of a construct and even extending to relationships across constructs in a broader theoretical model. However, studies that do not apply recommended extraction, rotation, and interpretation in FA risk drawing faulty conclusions about the validity of a measure. As measures are picked up by other researchers and applied in experimental designs, or by practitioners as assessments in practice, application of measures with subpar evidence for validity produces a ripple effect across the field. It is incumbent on researchers to ensure best practices are applied or engage with methodologists to support and consult where there are gaps in knowledge of methods. Further, it remains important to also critically evaluate measures selected for research and practice, focusing on those that demonstrate alignment with best practice for FA and instrument development. 7 , 11
Conflicts of Interest
The authors declare that they have no conflicts of interest.

Literature Reviews
- Getting started
What is a literature review?
Why conduct a literature review, stages of a literature review, lit reviews: an overview (video), check out these books.
- Types of reviews
- 1. Define your research question
- 2. Plan your search
- 3. Search the literature
- 4. Organize your results
- 5. Synthesize your findings
- 6. Write the review
- Artificial intelligence (AI) tools
- Thompson Writing Studio This link opens in a new window
- Need to write a systematic review? This link opens in a new window
Guide Owner

Contact a Librarian
Ask a Librarian
Definition: A literature review is a systematic examination and synthesis of existing scholarly research on a specific topic or subject.
Purpose: It serves to provide a comprehensive overview of the current state of knowledge within a particular field.
Analysis: Involves critically evaluating and summarizing key findings, methodologies, and debates found in academic literature.
Identifying Gaps: Aims to pinpoint areas where there is a lack of research or unresolved questions, highlighting opportunities for further investigation.
Contextualization: Enables researchers to understand how their work fits into the broader academic conversation and contributes to the existing body of knowledge.

tl;dr A literature review critically examines and synthesizes existing scholarly research and publications on a specific topic to provide a comprehensive understanding of the current state of knowledge in the field.
What is a literature review NOT?
❌ An annotated bibliography
❌ Original research
❌ A summary
❌ Something to be conducted at the end of your research
❌ An opinion piece
❌ A chronological compilation of studies
The reason for conducting a literature review is to:
| What has been written about your topic? What is the evidence for your topic? What methods, key concepts, and theories relate to your topic? Are there current gaps in knowledge or new questions to be asked? | |
| Bring your reader up to date Further your reader's understanding of the topic | |
| Provide evidence of... - your knowledge on the topic's theory - your understanding of the research process - your ability to critically evaluate and analyze information - that you're up to date on the literature |


Literature Reviews: An Overview for Graduate Students
While this 9-minute video from NCSU is geared toward graduate students, it is useful for anyone conducting a literature review.

Writing the literature review: A practical guide
Available 3rd floor of Perkins

Writing literature reviews: A guide for students of the social and behavioral sciences
Available online!

So, you have to write a literature review: A guided workbook for engineers

Telling a research story: Writing a literature review

The literature review: Six steps to success

Systematic approaches to a successful literature review
Request from Duke Medical Center Library

Doing a systematic review: A student's guide
- Next: Types of reviews >>
- Last Updated: Aug 29, 2024 11:40 AM
- URL: https://guides.library.duke.edu/litreviews

Services for...
- Faculty & Instructors
- Graduate Students
- Undergraduate Students
- International Students
- Patrons with Disabilities
- Harmful Language Statement
- Re-use & Attribution / Privacy
- Support the Libraries


Want to create or adapt books like this? Learn more about how Pressbooks supports open publishing practices.
Chapter 1: Introduction
Learning objectives.
At the conclusion of this chapter, you will be able to:
- Identify the purpose of the literature review in the research process
- Distinguish between different types of literature reviews
1.1 What is a Literature Review?
Pick up nearly any book on research methods and you will find a description of a literature review. At a basic level, the term implies a survey of factual or nonfiction books, articles, and other documents published on a particular subject. Definitions may be similar across the disciplines, with new types and definitions continuing to emerge. Generally speaking, a literature review is a:
- “comprehensive background of the literature within the interested topic area…” ( O’Gorman & MacIntosh, 2015, p. 31 ).
- “critical component of the research process that provides an in-depth analysis of recently published research findings in specifically identified areas of interest.” ( House, 2018, p. 109 ).
- “written document that presents a logically argued case founded on a comprehensive understanding of the current state of knowledge about a topic of study” ( Machi & McEvoy, 2012, p. 4 ).
As a foundation for knowledge advancement in every discipline, it is an important element of any research project. At the graduate or doctoral level, the literature review is an essential feature of thesis and dissertation, as well as grant proposal writing. That is to say, “A substantive, thorough, sophisticated literature review is a precondition for doing substantive, thorough, sophisticated research…A researcher cannot perform significant research without first understanding the literature in the field.” ( Boote & Beile, 2005, p. 3 ). It is by this means, that a researcher demonstrates familiarity with a body of knowledge and thereby establishes credibility with a reader. An advanced-level literature review shows how prior research is linked to a new project, summarizing and synthesizing what is known while identifying gaps in the knowledge base, facilitating theory development, closing areas where enough research already exists, and uncovering areas where more research is needed. ( Webster & Watson, 2002, p. xiii )
A graduate-level literature review is a compilation of the most significant previously published research on your topic. Unlike an annotated bibliography or a research paper you may have written as an undergraduate, your literature review will outline, evaluate and synthesize relevant research and relate those sources to your own thesis or research question. It is much more than a summary of all the related literature.
It is a type of writing that demonstrate the importance of your research by defining the main ideas and the relationship between them. A good literature review lays the foundation for the importance of your stated problem and research question.
Literature reviews:
- define a concept
- map the research terrain or scope
- systemize relationships between concepts
- identify gaps in the literature ( Rocco & Plathotnik, 2009, p. 128 )
The purpose of a literature review is to demonstrate that your research question is meaningful. Additionally, you may review the literature of different disciplines to find deeper meaning and understanding of your topic. It is especially important to consider other disciplines when you do not find much on your topic in one discipline. You will need to search the cognate literature before claiming there is “little previous research” on your topic.
Well developed literature reviews involve numerous steps and activities. The literature review is an iterative process because you will do at least two of them: a preliminary search to learn what has been published in your area and whether there is sufficient support in the literature for moving ahead with your subject. After this first exploration, you will conduct a deeper dive into the literature to learn everything you can about the topic and its related issues.
Literature Review Tutorial

1.2 Literature Review Basics
An effective literature review must:
- Methodologically analyze and synthesize quality literature on a topic
- Provide a firm foundation to a topic or research area
- Provide a firm foundation for the selection of a research methodology
- Demonstrate that the proposed research contributes something new to the overall body of knowledge of advances the research field’s knowledge base. ( Levy & Ellis, 2006 ).
All literature reviews, whether they are qualitative, quantitative or both, will at some point:
- Introduce the topic and define its key terms
- Establish the importance of the topic
- Provide an overview of the amount of available literature and its types (for example: theoretical, statistical, speculative)
- Identify gaps in the literature
- Point out consistent finding across studies
- Arrive at a synthesis that organizes what is known about a topic
- Discusses possible implications and directions for future research
1.3 Types of Literature Reviews
There are many different types of literature reviews, however there are some shared characteristics or features. Remember a comprehensive literature review is, at its most fundamental level, an original work based on an extensive critical examination and synthesis of the relevant literature on a topic. As a study of the research on a particular topic, it is arranged by key themes or findings, which may lead up to or link to the research question. In some cases, the research question will drive the type of literature review that is undertaken.
The following section includes brief descriptions of the terms used to describe different literature review types with examples of each. The included citations are open access, Creative Commons licensed or copyright-restricted.
1.3.1 Types of Review
1.3.1.1 conceptual.
Guided by an understanding of basic issues rather than a research methodology. You are looking for key factors, concepts or variables and the presumed relationship between them. The goal of the conceptual literature review is to categorize and describe concepts relevant to your study or topic and outline a relationship between them. You will include relevant theory and empirical research.
Examples of a Conceptual Review:
- Education : The formality of learning science in everyday life: A conceptual literature review. ( Dohn, 2010 ).
- Education : Are we asking the right questions? A conceptual review of the educational development literature in higher education. ( Amundsen & Wilson, 2012 ).
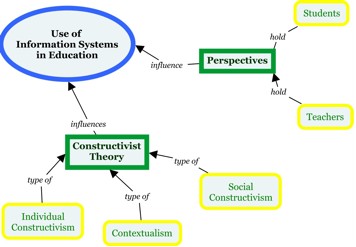
1.3.1.2 Empirical
An empirical literature review collects, creates, arranges, and analyzes numeric data reflecting the frequency of themes, topics, authors and/or methods found in existing literature. Empirical literature reviews present their summaries in quantifiable terms using descriptive and inferential statistics.
Examples of an Empirical Review:
- Nursing : False-positive findings in Cochrane meta-analyses with and without application of trial sequential analysis: An empirical review. ( Imberger, Thorlund, Gluud, & Wettersley, 2016 ).
- Education : Impediments of e-learning adoption in higher learning institutions of Tanzania: An empirical review ( Mwakyusa & Mwalyagile, 2016 ).
1.3.1.3 Exploratory
Unlike a synoptic literature review, the purpose here is to provide a broad approach to the topic area. The aim is breadth rather than depth and to get a general feel for the size of the topic area. A graduate student might do an exploratory review of the literature before beginning a synoptic, or more comprehensive one.
Examples of an Exploratory Review:
- Education : University research management: An exploratory literature review. ( Schuetzenmeister, 2010 ).
- Education : An exploratory review of design principles in constructivist gaming learning environments. ( Rosario & Widmeyer, 2009 ).

1.3.1.4 Focused
A type of literature review limited to a single aspect of previous research, such as methodology. A focused literature review generally will describe the implications of choosing a particular element of past research, such as methodology in terms of data collection, analysis and interpretation.
Examples of a Focused Review:
- Nursing : Clinical inertia in the management of type 2 diabetes mellitus: A focused literature review. ( Khunti, Davies, & Khunti, 2015 ).
- Education : Language awareness: Genre awareness-a focused review of the literature. ( Stainton, 1992 ).
1.3.1.5 Integrative
Critiques past research and draws overall conclusions from the body of literature at a specified point in time. Reviews, critiques, and synthesizes representative literature on a topic in an integrated way. Most integrative reviews are intended to address mature topics or emerging topics. May require the author to adopt a guiding theory, a set of competing models, or a point of view about a topic. For more description of integrative reviews, see Whittemore & Knafl (2005).
Examples of an Integrative Review:
- Nursing : Interprofessional teamwork and collaboration between community health workers and healthcare teams: An integrative review. ( Franklin, Bernhardt, Lopez, Long-Middleton, & Davis, 2015 ).
- Education : Exploring the gap between teacher certification and permanent employment in Ontario: An integrative literature review. ( Brock & Ryan, 2016 ).
1.3.1.6 Meta-analysis
A subset of a systematic review, that takes findings from several studies on the same subject and analyzes them using standardized statistical procedures to pool together data. Integrates findings from a large body of quantitative findings to enhance understanding, draw conclusions, and detect patterns and relationships. Gather data from many different, independent studies that look at the same research question and assess similar outcome measures. Data is combined and re-analyzed, providing a greater statistical power than any single study alone. It’s important to note that not every systematic review includes a meta-analysis but a meta-analysis can’t exist without a systematic review of the literature.
Examples of a Meta-Analysis:
- Education : Efficacy of the cooperative learning method on mathematics achievement and attitude: A meta-analysis research. ( Capar & Tarim, 2015 ).
- Nursing : A meta-analysis of the effects of non-traditional teaching methods on the critical thinking abilities of nursing students. ( Lee, Lee, Gong, Bae, & Choi, 2016 ).
- Education : Gender differences in student attitudes toward science: A meta-analysis of the literature from 1970 to 1991. ( Weinburgh, 1995 ).
1.3.1.7 Narrative/Traditional
An overview of research on a particular topic that critiques and summarizes a body of literature. Typically broad in focus. Relevant past research is selected and synthesized into a coherent discussion. Methodologies, findings and limits of the existing body of knowledge are discussed in narrative form. Sometimes also referred to as a traditional literature review. Requires a sufficiently focused research question. The process may be subject to bias that supports the researcher’s own work.
Examples of a Narrative/Traditional Review:
- Nursing : Family carers providing support to a person dying in the home setting: A narrative literature review. ( Morris, King, Turner, & Payne, 2015 ).
- Education : Adventure education and Outward Bound: Out-of-class experiences that make a lasting difference. ( Hattie, Marsh, Neill, & Richards, 1997 ).
- Education : Good quality discussion is necessary but not sufficient in asynchronous tuition: A brief narrative review of the literature. ( Fear & Erikson-Brown, 2014 ).
- Nursing : Outcomes of physician job satisfaction: A narrative review, implications, and directions for future research. ( Williams & Skinner, 2003 ).
1.3.1.8 Realist
Aspecific type of literature review that is theory-driven and interpretative and is intended to explain the outcomes of a complex intervention program(s).
Examples of a Realist Review:
- Nursing : Lean thinking in healthcare: A realist review of the literature. ( Mazzacato, Savage, Brommels, 2010 ).
- Education : Unravelling quality culture in higher education: A realist review. ( Bendermacher, Egbrink, Wolfhagen, & Dolmans, 2017 ).
1.3.1.9 Scoping
Tend to be non-systematic and focus on breadth of coverage conducted on a topic rather than depth. Utilize a wide range of materials; may not evaluate the quality of the studies as much as count the number. One means of understanding existing literature. Aims to identify nature and extent of research; preliminary assessment of size and scope of available research on topic. May include research in progress.
Examples of a Scoping Review:
- Nursing : Organizational interventions improving access to community-based primary health care for vulnerable populations: A scoping review. ( Khanassov, Pluye, Descoteaux, Haggerty, Russell, Gunn, & Levesque, 2016 ).
- Education : Interdisciplinary doctoral research supervision: A scoping review. ( Vanstone, Hibbert, Kinsella, McKenzie, Pitman, & Lingard, 2013 ).
- Nursing : A scoping review of the literature on the abolition of user fees in health care services in Africa. ( Ridde, & Morestin, 2011 ).
1.3.1.10 Synoptic
Unlike an exploratory review, the purpose is to provide a concise but accurate overview of all material that appears to be relevant to a chosen topic. Both content and methodological material is included. The review should aim to be both descriptive and evaluative. Summarizes previous studies while also showing how the body of literature could be extended and improved in terms of content and method by identifying gaps.
Examples of a Synoptic Review:
- Education : Theoretical framework for educational assessment: A synoptic review. ( Ghaicha, 2016 ).
- Education : School effects research: A synoptic review of past efforts and some suggestions for the future. ( Cuttance, 1981 ).
1.3.1.11 Systematic Review
A rigorous review that follows a strict methodology designed with a presupposed selection of literature reviewed. Undertaken to clarify the state of existing research, the evidence, and possible implications that can be drawn from that. Using comprehensive and exhaustive searching of the published and unpublished literature, searching various databases, reports, and grey literature. Transparent and reproducible in reporting details of time frame, search and methods to minimize bias. Must include a team of at least 2-3 and includes the critical appraisal of the literature. For more description of systematic reviews, including links to protocols, checklists, workflow processes, and structure see “ A Young Researcher’s Guide to a Systematic Review “.
Examples of a Systematic Review:
- Education : The potentials of using cloud computing in schools: A systematic literature review ( Hartmann, Braae, Pedersen, & Khalid, 2017 )
- Nursing : Is butter back? A systematic review and meta-analysis of butter consumption and risk of cardiovascular disease, diabetes, and total mortality. ( Pimpin, Wu, Haskelberg, Del Gobbo, & Mozaffarian, 2016 ).
- Education : The use of research to improve professional practice: a systematic review of the literature. ( Hemsley-Brown & Sharp, 2003 ).
- Nursing : Using computers to self-manage type 2 diabetes. ( Pal, Eastwood, Michie, Farmer, Barnard, Peacock, Wood, Inniss, & Murray, 2013 ).
1.3.1.12 Umbrella/Overview of Reviews
Compiles evidence from multiple systematic reviews into one document. Focuses on broad condition or problem for which there are competing interventions and highlights reviews that address those interventions and their effects. Often used in recommendations for practice.
Examples of an Umbrella/Overview Review:
- Education : Reflective practice in healthcare education: An umbrella review. ( Fragknos, 2016 ).
- Nursing : Systematic reviews of psychosocial interventions for autism: an umbrella review. ( Seida, Ospina, Karkhaneh, Hartling, Smith, & Clark, 2009 ).
For a brief discussion see “ Not all literature reviews are the same ” (Thomson, 2013).
1.4 Why do a Literature Review?
The purpose of the literature review is the same regardless of the topic or research method. It tests your own research question against what is already known about the subject.
1.4.1 First – It’s part of the whole. Omission of a literature review chapter or section in a graduate-level project represents a serious void or absence of critical element in the research process.
The outcome of your review is expected to demonstrate that you:
- can systematically explore the research in your topic area
- can read and critically analyze the literature in your discipline and then use it appropriately to advance your own work
- have sufficient knowledge in the topic to undertake further investigation
1.4.2 Second – It’s good for you!
- You improve your skills as a researcher
- You become familiar with the discourse of your discipline and learn how to be a scholar in your field
- You learn through writing your ideas and finding your voice in your subject area
- You define, redefine and clarify your research question for yourself in the process
1.4.3 Third – It’s good for your reader. Your reader expects you to have done the hard work of gathering, evaluating and synthesizes the literature. When you do a literature review you:
- Set the context for the topic and present its significance
- Identify what’s important to know about your topic – including individual material, prior research, publications, organizations and authors.
- Demonstrate relationships among prior research
- Establish limitations of existing knowledge
- Analyze trends in the topic’s treatment and gaps in the literature
1.4.4 Why do a literature review?
- To locate gaps in the literature of your discipline
- To avoid reinventing the wheel
- To carry on where others have already been
- To identify other people working in the same field
- To increase your breadth of knowledge in your subject area
- To find the seminal works in your field
- To provide intellectual context for your own work
- To acknowledge opposing viewpoints
- To put your work in perspective
- To demonstrate you can discover and retrieve previous work in the area
1.5 Common Literature Review Errors
Graduate-level literature reviews are more than a summary of the publications you find on a topic. As you have seen in this brief introduction, literature reviews are a very specific type of research, analysis, and writing. We will explore these topics more in the next chapters. Some things to keep in mind as you begin your own research and writing are ways to avoid the most common errors seen in the first attempt at a literature review. For a quick review of some of the pitfalls and challenges a new researcher faces when he/she begins work, see “ Get Ready: Academic Writing, General Pitfalls and (oh yes) Getting Started! ”.
As you begin your own graduate-level literature review, try to avoid these common mistakes:
- Accepts another researcher’s finding as valid without evaluating methodology and data
- Contrary findings and alternative interpretations are not considered or mentioned
- Findings are not clearly related to one’s own study, or findings are too general
- Insufficient time allowed to define best search strategies and writing
- Isolated statistical results are simply reported rather than synthesizing the results
- Problems with selecting and using most relevant keywords, subject headings and descriptors
- Relies too heavily on secondary sources
- Search methods are not recorded or reported for transparency
- Summarizes rather than synthesizes articles
In conclusion, the purpose of a literature review is three-fold:
- to survey the current state of knowledge or evidence in the area of inquiry,
- to identify key authors, articles, theories, and findings in that area, and
- to identify gaps in knowledge in that research area.
A literature review is commonly done today using computerized keyword searches in online databases, often working with a trained librarian or information expert. Keywords can be combined using the Boolean operators, “and”, “or” and sometimes “not” to narrow down or expand the search results. Once a list of articles is generated from the keyword and subject heading search, the researcher must then manually browse through each title and abstract, to determine the suitability of that article before a full-text article is obtained for the research question.
Literature reviews should be reasonably complete, and not restricted to a few journals, a few years, or a specific methodology or research design. Reviewed articles may be summarized in the form of tables, and can be further structured using organizing frameworks such as a concept matrix.
A well-conducted literature review should indicate whether the initial research questions have already been addressed in the literature, whether there are newer or more interesting research questions available, and whether the original research questions should be modified or changed in light of findings of the literature review.
The review can also provide some intuitions or potential answers to the questions of interest and/or help identify theories that have previously been used to address similar questions and may provide evidence to inform policy or decision-making. ( Bhattacherjee, 2012 ).

Read Abstract 1. Refer to Types of Literature Reviews. What type of literature review do you think this study is and why? See the Answer Key for the correct response.
Nursing : To describe evidence of international literature on the safe care of the hospitalised child after the World Alliance for Patient Safety and list contributions of the general theoretical framework of patient safety for paediatric nursing.
An integrative literature review between 2004 and 2015 using the databases PubMed, Cumulative Index of Nursing and Allied Health Literature (CINAHL), Scopus, Web of Science and Wiley Online Library, and the descriptors Safety or Patient safety, Hospitalised child, Paediatric nursing, and Nursing care.
Thirty-two articles were analysed, most of which were from North American, with a descriptive approach. The quality of the recorded information in the medical records, the use of checklists, and the training of health workers contribute to safe care in paediatric nursing and improve the medication process and partnerships with parents.
General information available on patient safety should be incorporated in paediatric nursing care. ( Wegner, Silva, Peres, Bandeira, Frantz, Botene, & Predebon, 2017 ).
Read Abstract 2. Refer to Types of Literature Reviews. What type of lit review do you think this study is and why? See the Answer Key for the correct response.
Education : The focus of this paper centers around timing associated with early childhood education programs and interventions using meta-analytic methods. At any given assessment age, a child’s current age equals starting age, plus duration of program, plus years since program ended. Variability in assessment ages across the studies should enable everyone to identify the separate effects of all three time-related components. The project is a meta-analysis of evaluation studies of early childhood education programs conducted in the United States and its territories between 1960 and 2007. The population of interest is children enrolled in early childhood education programs between the ages of 0 and 5 and their control-group counterparts. Since the data come from a meta-analysis, the population for this study is drawn from many different studies with diverse samples. Given the preliminary nature of their analysis, the authors cannot offer conclusions at this point. ( Duncan, Leak, Li, Magnuson, Schindler, & Yoshikawa, 2011 ).
Test Yourself
See Answer Key for the correct responses.
The purpose of a graduate-level literature review is to summarize in as many words as possible everything that is known about my topic.
A literature review is significant because in the process of doing one, the researcher learns to read and critically assess the literature of a discipline and then uses it appropriately to advance his/her own research.
Read the following abstract and choose the correct type of literature review it represents.
Nursing: E-cigarette use has become increasingly popular, especially among the young. Its long-term influence upon health is unknown. Aim of this review has been to present the current state of knowledge about the impact of e-cigarette use on health, with an emphasis on Central and Eastern Europe. During the preparation of this narrative review, the literature on e-cigarettes available within the network PubMed was retrieved and examined. In the final review, 64 research papers were included. We specifically assessed the construction and operation of the e-cigarette as well as the chemical composition of the e-liquid; the impact that vapor arising from the use of e-cigarette explored in experimental models in vitro; and short-term effects of use of e-cigarettes on users’ health. Among the substances inhaled by the e-smoker, there are several harmful products, such as: formaldehyde, acetaldehyde, acroleine, propanal, nicotine, acetone, o-methyl-benzaldehyde, carcinogenic nitrosamines. Results from experimental animal studies indicate the negative impact of e-cigarette exposure on test models, such as ascytotoxicity, oxidative stress, inflammation, airway hyper reactivity, airway remodeling, mucin production, apoptosis, and emphysematous changes. The short-term impact of e-cigarettes on human health has been studied mostly in experimental setting. Available evidence shows that the use of e-cigarettes may result in acute lung function responses (e.g., increase in impedance, peripheral airway flow resistance) and induce oxidative stress. Based on the current available evidence, e-cigarette use is associated with harmful biologic responses, although it may be less harmful than traditional cigarettes. (J ankowski, Brożek, Lawson, Skoczyński, & Zejda, 2017 ).
- Meta-analysis
- Exploratory
Education: In this review, Mary Vorsino writes that she is interested in keeping the potential influences of women pragmatists of Dewey’s day in mind while presenting modern feminist re readings of Dewey. She wishes to construct a narrowly-focused and succinct literature review of thinkers who have donned a feminist lens to analyze Dewey’s approaches to education, learning, and democracy and to employ Dewey’s works in theorizing on gender and education and on gender in society. This article first explores Dewey as both an ally and a problematic figure in feminist literature and then investigates the broader sphere of feminist pragmatism and two central themes within it: (1) valuing diversity, and diverse experiences; and (2) problematizing fixed truths. ( Vorsino, 2015 ).
Image Attributions
Literature Reviews for Education and Nursing Graduate Students Copyright © by Linda Frederiksen is licensed under a Creative Commons Attribution 4.0 International License , except where otherwise noted.
Share This Book
- Locations and Hours
- UCLA Library
- Research Guides
- Biomedical Library Guides
Systematic Reviews
- Types of Literature Reviews
What Makes a Systematic Review Different from Other Types of Reviews?
- Planning Your Systematic Review
- Database Searching
- Creating the Search
- Search Filters and Hedges
- Grey Literature
- Managing and Appraising Results
- Further Resources
Reproduced from Grant, M. J. and Booth, A. (2009), A typology of reviews: an analysis of 14 review types and associated methodologies. Health Information & Libraries Journal, 26: 91–108. doi:10.1111/j.1471-1842.2009.00848.x
| Aims to demonstrate writer has extensively researched literature and critically evaluated its quality. Goes beyond mere description to include degree of analysis and conceptual innovation. Typically results in hypothesis or mode | Seeks to identify most significant items in the field | No formal quality assessment. Attempts to evaluate according to contribution | Typically narrative, perhaps conceptual or chronological | Significant component: seeks to identify conceptual contribution to embody existing or derive new theory | |
| Generic term: published materials that provide examination of recent or current literature. Can cover wide range of subjects at various levels of completeness and comprehensiveness. May include research findings | May or may not include comprehensive searching | May or may not include quality assessment | Typically narrative | Analysis may be chronological, conceptual, thematic, etc. | |
| Mapping review/ systematic map | Map out and categorize existing literature from which to commission further reviews and/or primary research by identifying gaps in research literature | Completeness of searching determined by time/scope constraints | No formal quality assessment | May be graphical and tabular | Characterizes quantity and quality of literature, perhaps by study design and other key features. May identify need for primary or secondary research |
| Technique that statistically combines the results of quantitative studies to provide a more precise effect of the results | Aims for exhaustive, comprehensive searching. May use funnel plot to assess completeness | Quality assessment may determine inclusion/ exclusion and/or sensitivity analyses | Graphical and tabular with narrative commentary | Numerical analysis of measures of effect assuming absence of heterogeneity | |
| Refers to any combination of methods where one significant component is a literature review (usually systematic). Within a review context it refers to a combination of review approaches for example combining quantitative with qualitative research or outcome with process studies | Requires either very sensitive search to retrieve all studies or separately conceived quantitative and qualitative strategies | Requires either a generic appraisal instrument or separate appraisal processes with corresponding checklists | Typically both components will be presented as narrative and in tables. May also employ graphical means of integrating quantitative and qualitative studies | Analysis may characterise both literatures and look for correlations between characteristics or use gap analysis to identify aspects absent in one literature but missing in the other | |
| Generic term: summary of the [medical] literature that attempts to survey the literature and describe its characteristics | May or may not include comprehensive searching (depends whether systematic overview or not) | May or may not include quality assessment (depends whether systematic overview or not) | Synthesis depends on whether systematic or not. Typically narrative but may include tabular features | Analysis may be chronological, conceptual, thematic, etc. | |
| Method for integrating or comparing the findings from qualitative studies. It looks for ‘themes’ or ‘constructs’ that lie in or across individual qualitative studies | May employ selective or purposive sampling | Quality assessment typically used to mediate messages not for inclusion/exclusion | Qualitative, narrative synthesis | Thematic analysis, may include conceptual models | |
| Assessment of what is already known about a policy or practice issue, by using systematic review methods to search and critically appraise existing research | Completeness of searching determined by time constraints | Time-limited formal quality assessment | Typically narrative and tabular | Quantities of literature and overall quality/direction of effect of literature | |
| Preliminary assessment of potential size and scope of available research literature. Aims to identify nature and extent of research evidence (usually including ongoing research) | Completeness of searching determined by time/scope constraints. May include research in progress | No formal quality assessment | Typically tabular with some narrative commentary | Characterizes quantity and quality of literature, perhaps by study design and other key features. Attempts to specify a viable review | |
| Tend to address more current matters in contrast to other combined retrospective and current approaches. May offer new perspectives | Aims for comprehensive searching of current literature | No formal quality assessment | Typically narrative, may have tabular accompaniment | Current state of knowledge and priorities for future investigation and research | |
| Seeks to systematically search for, appraise and synthesis research evidence, often adhering to guidelines on the conduct of a review | Aims for exhaustive, comprehensive searching | Quality assessment may determine inclusion/exclusion | Typically narrative with tabular accompaniment | What is known; recommendations for practice. What remains unknown; uncertainty around findings, recommendations for future research | |
| Combines strengths of critical review with a comprehensive search process. Typically addresses broad questions to produce ‘best evidence synthesis’ | Aims for exhaustive, comprehensive searching | May or may not include quality assessment | Minimal narrative, tabular summary of studies | What is known; recommendations for practice. Limitations | |
| Attempt to include elements of systematic review process while stopping short of systematic review. Typically conducted as postgraduate student assignment | May or may not include comprehensive searching | May or may not include quality assessment | Typically narrative with tabular accompaniment | What is known; uncertainty around findings; limitations of methodology | |
| Specifically refers to review compiling evidence from multiple reviews into one accessible and usable document. Focuses on broad condition or problem for which there are competing interventions and highlights reviews that address these interventions and their results | Identification of component reviews, but no search for primary studies | Quality assessment of studies within component reviews and/or of reviews themselves | Graphical and tabular with narrative commentary | What is known; recommendations for practice. What remains unknown; recommendations for future research |
- << Previous: Home
- Next: Planning Your Systematic Review >>
- Last Updated: Jul 23, 2024 3:40 PM
- URL: https://guides.library.ucla.edu/systematicreviews
Analysis of Literature Review in Cases of Exploratory Research
13 Pages Posted: 24 Mar 2020
Punyashlok Dash
Independent
Date Written: December 17, 2019
As the name suggest a good literature review is always comprehensive and contextualized with respect to the research. It provides the reader or the target audience with a base of the theory base along with a survey of published works that pertain to the investigation of the researcher and further an analysis of that particular work. It is a critical if not factual overview of what has gone before and what has already been researched upon. It mostly contains secondary sources of data, however it maybe done through Primary Data as well. If we consider Exploratory research, as the name implies, intends merely to explore the research questions and does not intend to offer final and conclusive solutions to existing problems.
Keywords: Exploratory Research, Point of Departure, Qualitative Research, Conformity
Suggested Citation: Suggested Citation
Punyashlok Dash (Contact Author)
Independent ( email ), do you have a job opening that you would like to promote on ssrn, paper statistics, related ejournals, criminology ejournal.
Subscribe to this fee journal for more curated articles on this topic
Systematic Reviews and Meta-Analyses: Exploratory Search
- Get Started
Exploratory Search
- Where to Search
- How to Search
- Grey Literature
- What about errata and retractions?
- Eligibility Screening
- Critical Appraisal
- Data Extraction
- Synthesis & Discussion
- Assess Certainty
- Share & Archive

Once you have an initial research question, you can develop and refine your research question and eligibility criteria through exploratory searching . Exploratory searching is also called preliminary, initial, and naive or novice searching. Regardless of what you call it, it is simply a series of searches conducted prior to starting the review with the goal of producing a well-defined scope with clear demonstration of contribution to the field. This is an iterative process as illustrated in the image to the right.
Throughout the exploratory search you should collect A. existing and in-progress reviews and B. seminal articles related to your scope. Ultimately, this phase should help your team produce :
- A clear, well-defined scope
- 2-5 Seminal articles to validate your search later on
- Context of what has been done to address this question, illustrating that this review does not duplicate existing or in-progress publications
At the bottom of this page, we also suggest C. where to start exploratory searching .
A. Existing & in-progress reviews
- Searching Tips
- What if my review exists?
Does your review already exist?
Before starting, make sure a systematic review hasn't already addressed, or is in the process of addressing your research question(s).
You should look for published systematic reviews , but also check out review registries and general purpose repositories (e.g., Open Science Framework ) where you're more likely to find unpublished or in-progress reviews and/or review protocols. Searching registries will give you a glimpse into the work that is being done currently, but isn't yet complete. Remember, this kind of review is a serious time-commitment, and you don't want to unknowingly duplicate efforts.
Existing and in-progress reviews on similar, non-identical topics can be helpful when identifying where to search and developing the search strategy and data extraction forms !
Searching tips
In academic journal databases, you can sometimes find a filter for Systematic Reviews , Meta-Analyses , and/or simply Reviews . If a built-in filter doesn't exist, you can add the term "review" to your search.
|
: Does drinking coffee reduce the likelihood of falling asleep while driving? )
If you get too many results, you can specify the of review: ) |
What if my review already exists?
We pursue systematic reviews and/or meta-analyses to answer a research question. If a review already answers your question, this existing review can be the foundation of your next research project!
Pursuing a different review
Sometimes it is still important to pursue a review, even if your original research question(s) have been answered. What is considered "the same" review is not always clear. Generally speaking, you need to justify that and illustrate how your new review contributes something unique to the field.
If a review already answers your question, and your team would still like to pursue a review, your team can:
- Update reviews that are out of date
- Enhance reviews with significant limitations / quality concerns
- Attempt to replicate the review
- Revise your original question
Updating a Review
According to Garner, et al., (2016) , "The decision [of whether or not to update] needs to take into account whether the review addresses a current question , uses valid methods , and is well conducted ; and whether there are new relevant methods , new studies , or new information on existing included studies. Given this information, the agency, editors, or authors need to judge whether the update will influence the review findings or credibility sufficiently to justify the effort in updating it."
Additional Guidance
Bashir, R., et al. Time-to-update of systematic reviews relative to the availability of new evidence. Syst Rev 7, 195 (2018). https://doi.org/10.1186/s13643-018-0856-9
Garner, P., et al. Panel for updating guidance for systematic reviews (PUGs). (2016). When and how to update systematic reviews: Consensus and checklist . BMJ , i3507. https://doi.org/10.1136/bmj.i3507
Replicating a Review
Review replication is not often pursued due to the amount of time and labor required. However, Pieper, Heß, & Faggion (2021) have developed a framework for replicating, and the replication process is a great learning tool.
What if a restricted / rapid review , or a scoping review exists , but not a systematic review ?
You may find other reviews (e.g., scoping review, restricted (or rapid) review) on your topic exist - that's great, as these might provide further insight to the appropriateness of the systematic review method for your research question(s) and how to frame your own review approach .
B. Seminal Articles
What is 'seminal work'.
In general, seminal work also called pivotal , landmark , or seed studies, are articles that are central to the research topic and have great importance and influence within the discipline. Seminal articles are likely to be cited frequently in different journal articles, books, dissertations etc.
Seminal Articles in Systematic Reviews
In systematic reviews and/or meta-analyses, seminal work are the "seed articles" for your specific review - the articles (or other material) you know need to be included in your final synthesis. These articles may have sparked the teams interest in pursuing a review or may be identified through the exploratory search.
Seminal articles can be helpful when identifying where to search and developing the search strategy !
C. Where to "Exploratory Search"?
- General Searches
- SR-Specific Repositories
Where to Exploratory Search?
In short, where you exploratory search will depend on your research question. In other words, you should consider searching wherever you are likely to find material that answers your research question.
In addition to repositories, you'll want to search academic journal databases that may be relevant to your topic. Consider your topic from perspectives other than your own discipline - it's likely your topic overlaps with several disciplines. For example, if you are examining a public health topic, it may be useful to search databases related to health / medicine and social sciences.
You can also use this exploratory phase to determine whether a database is relevant and should be searched as part of your final comprehensive systematic review search strategy, or not.
Check out the VT libraries "A-Z Database List" , or Librarian curated Library Guides related to your discipline!
Hint: Sort "By Subject" to find relevant guides
Web Browsing
Web browsing in Google or Google Scholar is a great place to start finding seminal works and existing reviews, as well as journals and databases in which you should conduct more robust exploratory searches.
Never rely only on web browsing . While Google Scholar (and Google) are great places to start searching, results are tailored to individual users, are not replicable, and algorithms are not transparent. More guidance for web browsing is located in the "Where to Search" sub-tab of the "Comprehensive Search" section of this guide.
More places to search...
The possibilities of where to exploratory search are endless! Consider searching anywhere that seminal articles or existing/in-progress reviews relevant to your scope may exist. Here are a few more places to get you started.
General Purpose Repositories
Researchers use these sites to share unpublished or in-progress research and reviews, procedural documentation, and other grey literature. For example:
- Open Science Framework (OSF)
Repositories that contain Preprints
Researchers uses these sites to openly share research , some of which is not yet published (or peer-reviewed), also called 'preprints'. For example:
Systematic Review Repositories
There are several systematic review repositories that exist - some contain only published reviews , while others include review registrations and protocols . In the following table, we present and link out to some repositories that specifically house systematic reviews and similar evidence synthesis publications .
Campbell Collaboration Registry
"...all registered titles for systematic reviews or evidence and gap maps that have been accepted by the Editor of a Campbell Coordinating Group. When titles progress to protocol stage, the protocol is published in the Campbell Systematic Reviews journal."
Campbell Systematic Review Journal
Both registry and journal include topics related to Business and Management, Climate Solutions, Crime and Justice, Disability, Education, International Development, Knowledge Translation and Implementation, and Social Welfare
Cochrane Database of Systematic Reviews (CDSR)
"...the leading journal and database for systematic reviews in health care. CDSR includes Cochrane Reviews (systematic reviews) and protocols for Cochrane Reviews as well as editorials and supplements."
Cochrane Library
"Cochrane Collaboration produces high-quality systematic reviews in health disciplines. For more detail and specific fields of research, check out the Cochrane Review Groups and Networks. "
Database of promoting health effectiveness reviews (DoPHER)
"...focussed coverage of systematic and non-systematic reviews of effectiveness in health promotion and public health worldwide. This register currently contains details of over 6,000 reviews of health promotion and public health effectiveness."
Epistemonkios
"...a collaborative, multilingual database of health evidence. It is the largest source of systematic reviews relevant for health-decision making, and a large source of other types of scientific evidence."
Health Evidence
"...quality-rated systematic reviews evaluating the effectiveness and cost-effectiveness of public health interventions, including cost data."
Joanna Briggs Systematic Review
"...a collection of world-class resources driven by the needs of health professionals and consumers worldwide"
"International database of prospectively registered systematic reviews in health and social care, welfare, public health, education, crime, justice, and international development, where there is a health related outcome."
- << Previous: Define Scope
- Next: Protocol >>
- Last Updated: Aug 29, 2024 8:40 AM
- URL: https://guides.lib.vt.edu/SRMA
- Exploratory Analysis
Artificial intelligence innovation in healthcare: Literature review, exploratory analysis, and future research
- Technology in Society 74(4):102321
- 74(4):102321

- Mohammed VI Polytechnic University

Discover the world's research
- 25+ million members
- 160+ million publication pages
- 2.3+ billion citations
No full-text available
To read the full-text of this research, you can request a copy directly from the authors.
- J Nurs Manag
- Atallah Alenezi
- Mohammed Hamdan Alshammari

- Nandhini Mahesh

- Jameel Mustafa
- Ian Horrocks
- Asif Nadeem

- Comput Model Eng Sci

- Mohamed El Kotbi
- Fatima Zahra Achour
- Yong Nam Gwon

- Hyun Soo Chung

- Cogan Nicola
- Rahul Chodhari
- Indranil Chakravorty

- Opeoluwa Akomolafe
- Jane Osareme Ogugua
- Oluwafunmi Adijat Elufioye
- Injla Iqbal
- Mahrukh Iqbal
- Abdulraheem Olaide Babarinde

- Oluwatoyin Ayo-Farai
- Chinedu Paschal Maduka
- Babarinde Abdulraheem Olaide
- Chiamaka Chinaemelum Okongwu

- Indian J Palliat Care
- Prakash Gyandev Gondode
- Vaishali Mahor
- Pooja Yadav
- Sabyasachi Pramanik

- Saravana Mahesan S.

- Zhazira Kusmoldayeva
- Magbat Spanov
- Gulzada Mukhamediyeva
- Gulmira Sugirova
- Harisankar P V
- Sushant Malik

- Jianguo Wang
- Oluwasoye P. Mafimisebi
- Bisola Ariyo
- Ibitayo Adebayo

- Muskan Sharma
- Inderjeet Singh

- Jaspreet Kaur
- CYTOM PART B-CLIN CY
- Goce Bogdanoski
- Fabienne Lucas
- Wolfgang Kern
- Kamila Czechowska

- Mohammed Umar Usmani
- Int Neurourol J

- SOC SCI MED
- Sandra Gillner

- Peter A. Murray

- Fawaz S. Al-Anzi

- Anil Kumar Bandrana

- Med Educ Online

- Amir Madany Mamlouk

- Tessa Sundaram Cook

- Josiane Courteau

- Johnny Dang

- Mingyang Chen
- BRIT J HAEMATOL
- Shang Yuin Chai

- Gerard Flaherty
- BMC HEALTH SERV RES

- BMC PSYCHIATRY

- Michael D Abràmoff
- Cybil Roehrenbeck
- Sylvia Trujillo
- Ezequiel “Zeke” Silva III

- Romain Pirracchio
- Albert Boonstra
- Mente Laven
- ARTIF INTELL MED

- Ioannis Varkarakis

- BMC Med Ethics

- Victor Galaz

- Peter W. Callahan

- Stuart Slavin

- BMC MED INFORM DECIS

- Aurelio Secinaro

- Muhammad Naufal
- Rusni Masnina
- Debdipto Misra

- Felix Gille

- J MED INTERNET RES

- Liam G. McCoy
- Sujay Nagaraj
- Felipe Morgado
- Leo Anthony Celi

- Yannick Auclair

- Rohit Srinivasan
- Ashik Amlani

- Nikhil R Sahni
- George Stein
- Rodney Zemmel
- David M. Cutler
- INT J INFORM MANAGE

- Sujeet Kumar Sharma

- Emna Chikhaoui
- Alanoud Alajmi

- Diana Mincu
- Subhrajit Roy
- Gabrielle Bunney
- Steven Tran
- Scott Dresden
- Xiaohui Liu
- Mengmeng Wang
- Huizhang Shen
- Eur J Innovat Manag

- TECHNOVATION

- Antonio Fusco
- Matilda Shini
- Christian Hugo Hoffmann
- Alan S. Young

- BBA-REV CANCER
- Norman E. Sharpless
- Anthony R. Kerlavage
- INFORM FUSION

- Xiao-Yun Zhou

- Kaveh Memarzadeh
- Recruit researchers
- Join for free
- Login Email Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google Welcome back! Please log in. Email · Hint Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google No account? Sign up
- DOI: 10.1016/j.techsoc.2023.102321
- Corpus ID: 259347766
Artificial intelligence innovation in healthcare: Literature review, exploratory analysis, and future research
- A. Zahlan , Ravi Ranjan , David Hayes
- Published in Technology and Society 1 August 2023
- Medicine, Computer Science
22 Citations
Debunking palliative care myths: assessing the performance of artificial intelligence chatbots (chatgpt vs. google gemini), perceptions and attitudes of nurse practitioners toward artificial intelligence adoption in health care, managing healthcare innovation activities in kazakhstan for optimal effectiveness, championing health systems management with digital innovation and applications in the age of artificial intelligence: protocol for a research program, determinants of artificial intelligence-assisted diagnostic system adoption intention: a behavioral reasoning theory perspective, the use of generative ai for scientific literature searches for systematic reviews: chatgpt and microsoft bing ai performance evaluation, analyzing the impact of ai on knowledge acquisition of students, hospital innovations for the next decade, fintech frenzy: an engaging review of the transforming financial services, investigating the influence of stakeholders' collaboration on open innovation in healthcare, 110 references, artificial intelligence (ai)-enabled crm capability in healthcare: the impact on service innovation, chatbots for future docs: exploring medical students’ attitudes and knowledge towards artificial intelligence and medical chatbots, machine learning to improve frequent emergency department use prediction: a retrospective cohort study, the potential impact of artificial intelligence on healthcare spending, developing robust benchmarks for driving forward ai innovation in healthcare, understanding the acceptance of emotional artificial intelligence in japanese healthcare system: a cross-sectional survey of clinic visitors’ attitude, changes in radiology due to artificial intelligence that can attract medical students to the specialty, using machine learning to predict hospital disposition with geriatric emergency department innovation intervention., acceptance of clinical artificial intelligence among physicians and medical students: a systematic review with cross-sectional survey, integrating artificial intelligence into haematology training and practice: opportunities, threats and proposed solutions, related papers.
Showing 1 through 3 of 0 Related Papers
- Download PDF
- Share X Facebook Email LinkedIn
- Permissions
Weight Gain After Adenotonsillectomy in Children With Mild Obstructive Sleep-Disordered Breathing : Exploratory Analysis of the PATS Randomized Clinical Trial
- 1 Department of Otolaryngology–Head and Neck Surgery, University of Michigan, Ann Arbor
- 2 Division of Otolaryngology, Head and Neck Surgery, School of Medicine and Public Health, University of Wisconsin, Madison
- 3 Department of Otolaryngology, Eastern Virginia Medical School, Children’s Hospital of The King’s Daughters, Norfolk
- 4 Deputy Editor, JAMA Otolaryngology–Head & Neck Surgery
- 5 Department of Otolaryngology–Head and Neck Surgery and Neurology Sleep Disorders Center, University of Texas Southwestern Medical Center, Dallas
- 6 Department of Pediatrics, University of Texas Southwestern Medical Center, Dallas
- 7 Department of Pediatrics, Children’s Hospital of Philadelphia, Perelman School of Medicine, University of Pennsylvania, Philadelphia
- 8 Division of Pediatric Otolaryngology, Children’s Hospital of Philadelphia, Perelman School of Medicine, University of Pennsylvania, Philadelphia
- 9 Sleep Disorders Center and Department of Pediatrics and Communicable Diseases, University of Michigan, Ann Arbor
- 10 Department of Pediatrics, University Hospitals Rainbow Babies & Children’s Hospital, Cleveland, Ohio
- 11 Department of Population Medicine, Harvard Pilgrim Health Care Institute and Harvard Medical School, Boston, Massachusetts
- 12 Department of Biostatistics, Harvard T. H. Chan School of Public Health, Boston, Massachusetts
- 13 Department of Medicine, Brigham and Women’s Hospital, Harvard Medical School, Boston, Massachusetts
- 14 Sleep Disorders Center and Department of Neurology, University of Michigan, Ann Arbor
- Invited Commentary Untangling Pediatric Obstructive Sleep Apnea, Adenotonsillectomy, and Weight—Beyond the Surgery Nikhila P. Raol, MD, MPH; David F. Smith, MD, PhD; Derek J. Lam, MD, MPH JAMA Otolaryngology–Head & Neck Surgery
Question Does adenotonsillectomy increase the risk of undesirable weight gain in children with mild obstructive sleep-disordered breathing?
Findings This exploratory analysis of data from the Pediatric Adenotonsillectomy Trial for Snoring (PATS) randomized clinical trial included 375 children with mild obstructive sleep-disordered breathing and did not demonstrate an increased risk of undesirable weight gain during the first 12 months after adenotonsillectomy vs observation.
Meaning These findings indicate that clinicians can reassure parents that adenotonsillectomy alone is unlikely to result in undesirable weight gain in children.
Importance It is unknown whether adenotonsillectomy causes undesirable weight gain in children with mild obstructive sleep-disordered breathing (oSDB).
Objective To compare changes in anthropometric measures in children with mild oSDB treated with adenotonsillectomy vs watchful waiting.
Design, Setting, and Participants This was an exploratory analysis of the Pediatric Adenotonsillectomy Trial for Snoring (PATS) randomized clinical trial of adenotonsillectomy vs watchful waiting for mild oSDB (snoring with obstructive apnea-hypopnea index of <3 events/hour) that took place at 7 pediatric tertiary care centers across the US and included 458 children aged 3.0 to 12.9 years with mild oSDB. Participants were recruited from June 29, 2016, to February 1, 2021. Anthropomorphic measures taken at baseline and 12 months after randomization were standardized for age and sex, including each participant’s percentage of the 95th body mass index percentile (%BMIp95). Data analyses were performed from March 15, 2023, to April 1, 2024.
Intervention Early adenotonsillectomy (eAT) vs watchful waiting with supportive care (WWSC).
Main Outcomes and Measures Twelve-month change in %BMIp95 from baseline and undesirable weight gain (defined as any weight gain in a child who already had overweight or obesity or an increase from baseline normal weight/underweight to overweight/obesity) at follow-up assessment.
Results The study analysis included 375 children (mean [SD] age, 6.1 [2.3] years; 188 [50.2%] females), of whom 143 (38%) had overweight or obesity at baseline. At 12 months, children in the eAT group experienced a 1.25-point increase in %BMIp95 compared with a 0.59-point increase in the WWSC group (mean difference, 0.93; 95% CI, −0.39 to 2.25). Undesirable weight gain was also similar between the eAT (n = 120; 32%) and WWSC (n = 101; 27%) groups (mean difference, 4%; 95% CI, 5% to 14%).
Conclusions and Relevance The findings of this exploratory analysis of the PATS trial indicate that adenotonsillectomy was not independently associated with an increased risk of undesirable weight gain in children with mild oSDB. However, one-third of the children gained undesirable weight during the study, which suggests that there is an opportunity to address healthy weight management during the evaluation and treatment of children with mild oSDB.
Trial Registration ClinicalTrials.gov Identifier: NCT02562040
- Invited Commentary Untangling Pediatric Obstructive Sleep Apnea, Adenotonsillectomy, and Weight—Beyond the Surgery JAMA Otolaryngology–Head & Neck Surgery
Read More About
Kirkham EM , Ishman S , Baldassari CM, et al. Weight Gain After Adenotonsillectomy in Children With Mild Obstructive Sleep-Disordered Breathing : Exploratory Analysis of the PATS Randomized Clinical Trial . JAMA Otolaryngol Head Neck Surg. Published online August 22, 2024. doi:10.1001/jamaoto.2024.2554
Manage citations:
© 2024
Artificial Intelligence Resource Center
Otolaryngology in JAMA : Read the Latest
Browse and subscribe to JAMA Network podcasts!
Others Also Liked
Select your interests.
Customize your JAMA Network experience by selecting one or more topics from the list below.
- Academic Medicine
- Acid Base, Electrolytes, Fluids
- Allergy and Clinical Immunology
- American Indian or Alaska Natives
- Anesthesiology
- Anticoagulation
- Art and Images in Psychiatry
- Artificial Intelligence
- Assisted Reproduction
- Bleeding and Transfusion
- Caring for the Critically Ill Patient
- Challenges in Clinical Electrocardiography
- Climate and Health
- Climate Change
- Clinical Challenge
- Clinical Decision Support
- Clinical Implications of Basic Neuroscience
- Clinical Pharmacy and Pharmacology
- Complementary and Alternative Medicine
- Consensus Statements
- Coronavirus (COVID-19)
- Critical Care Medicine
- Cultural Competency
- Dental Medicine
- Dermatology
- Diabetes and Endocrinology
- Diagnostic Test Interpretation
- Drug Development
- Electronic Health Records
- Emergency Medicine
- End of Life, Hospice, Palliative Care
- Environmental Health
- Equity, Diversity, and Inclusion
- Facial Plastic Surgery
- Gastroenterology and Hepatology
- Genetics and Genomics
- Genomics and Precision Health
- Global Health
- Guide to Statistics and Methods
- Hair Disorders
- Health Care Delivery Models
- Health Care Economics, Insurance, Payment
- Health Care Quality
- Health Care Reform
- Health Care Safety
- Health Care Workforce
- Health Disparities
- Health Inequities
- Health Policy
- Health Systems Science
- History of Medicine
- Hypertension
- Images in Neurology
- Implementation Science
- Infectious Diseases
- Innovations in Health Care Delivery
- JAMA Infographic
- Law and Medicine
- Leading Change
- Less is More
- LGBTQIA Medicine
- Lifestyle Behaviors
- Medical Coding
- Medical Devices and Equipment
- Medical Education
- Medical Education and Training
- Medical Journals and Publishing
- Mobile Health and Telemedicine
- Narrative Medicine
- Neuroscience and Psychiatry
- Notable Notes
- Nutrition, Obesity, Exercise
- Obstetrics and Gynecology
- Occupational Health
- Ophthalmology
- Orthopedics
- Otolaryngology
- Pain Medicine
- Palliative Care
- Pathology and Laboratory Medicine
- Patient Care
- Patient Information
- Performance Improvement
- Performance Measures
- Perioperative Care and Consultation
- Pharmacoeconomics
- Pharmacoepidemiology
- Pharmacogenetics
- Pharmacy and Clinical Pharmacology
- Physical Medicine and Rehabilitation
- Physical Therapy
- Physician Leadership
- Population Health
- Primary Care
- Professional Well-being
- Professionalism
- Psychiatry and Behavioral Health
- Public Health
- Pulmonary Medicine
- Regulatory Agencies
- Reproductive Health
- Research, Methods, Statistics
- Resuscitation
- Rheumatology
- Risk Management
- Scientific Discovery and the Future of Medicine
- Shared Decision Making and Communication
- Sleep Medicine
- Sports Medicine
- Stem Cell Transplantation
- Substance Use and Addiction Medicine
- Surgical Innovation
- Surgical Pearls
- Teachable Moment
- Technology and Finance
- The Art of JAMA
- The Arts and Medicine
- The Rational Clinical Examination
- Tobacco and e-Cigarettes
- Translational Medicine
- Trauma and Injury
- Treatment Adherence
- Ultrasonography
- Users' Guide to the Medical Literature
- Vaccination
- Venous Thromboembolism
- Veterans Health
- Women's Health
- Workflow and Process
- Wound Care, Infection, Healing
- Register for email alerts with links to free full-text articles
- Access PDFs of free articles
- Manage your interests
- Save searches and receive search alerts

- International Gas Turbine Institute
- Previous Paper
A Literature Review on Data Sources and Methodologies for Enriching Gas Path Analysis With Earth Observation Data
- Article contents
- Figures & tables
- Supplementary Data
- Peer Review
- Cite Icon Cite
- Permissions
- Search Site
Seume, E, Göing, J, & Friedrichs, J. "A Literature Review on Data Sources and Methodologies for Enriching Gas Path Analysis With Earth Observation Data." Proceedings of the ASME Turbo Expo 2024: Turbomachinery Technical Conference and Exposition . Volume 1: Aircraft Engine . London, United Kingdom. June 24–28, 2024. V001T01A015. ASME. https://doi.org/10.1115/GT2024-122772
Download citation file:
- Ris (Zotero)
- Reference Manager
Aero engine performance and condition deterioration are a function of operational severity. Operational severity is determined by various aspects such as airborne contaminants, derates, ambient temperature, humidity, and precipitation. More severe operating environments induce cost, which should be managed by using earth observation (EO) data in engine health monitoring. This paper presents an analytical approach that incorporates a broad set of EO data into engine health management and subsequent maintenance planning. Current approaches to gas path analysis are extended by incorporating EO data. The analytical approach is presented in combination with a literature review. The literature review covers the following topics: flight trajectory modeling, EO/environmental condition data, as well as engine performance, condition, and deterioration modeling. Methods and data sources in these different areas are reviewed while simultaneously presenting the currently researched analytical approach. The researched analytical approach creates high-resolution contamination profiles for a flight trajectory on a global scale. Weather conditions and the ingestion of aerosols and sand are monitored and correlated with aero engine condition and performance. A wide range of data sources are presented, which however only partly cater to the needs of the Maintenance, Repair and Overhaul community.
Purchase this Content
Product added to cart., email alerts, related proceedings papers, related articles, related chapters, affiliations.
- ASME Conference Publications and Proceedings
- Conference Proceedings Author Guidelines
- Indexing and Discovery
ASME Journals
- About ASME Journals
- Information for Authors
- Submit a Paper
- Call for Papers
- Title History
ASME Conference Proceedings
- About ASME Conference Publications and Proceedings
ASME eBooks
- About ASME eBooks
- ASME Press Advisory & Oversight Committee
- Book Proposal Guidelines
- Frequently Asked Questions
- Publication Permissions & Reprints
- ASME Membership
Opportunities
- Faculty Positions
- ASME Instagram

- Accessibility
- Privacy Statement
- Terms of Use
- Get Adobe Acrobat Reader
This Feature Is Available To Subscribers Only
Sign In or Create an Account
Content Search
Literature review: emerging innovations and best practices in social research - key takeaways for humanitarian and development action (july 2024).
- IMPACT Initiatives
Attachments

Introduction
Applied social research is a field of study which aims to understand and address real-world problems, through the application of research methods in sociology, psychology, anthropology and related fields, to gain insights into specific phenomena and inform decision-making in public policy and similar practical contexts. Over recent decades, the field has experienced transformative changes driven by technological advancements, globalization, and evolving methodologies. Moreover, social research has become essential in shaping humanitarian and development action, providing crucial insights that guide interventions, policies, and resource allocation, across different contexts of crisis.
As one of the largest independent research actors currently operating in crisis contexts, IMPACT Initiatives (IMPACT), with support from the USAID Bureau of Humanitarian Assistance (BHA), launched an in-depth literature review at the beginning of 2024 to understand what the emerging innovations and best practices in the field of social research are, and how these can be applied for research efforts within the humanitarian and development sector.
This paper summarises the key findings from this literature review, broken down into four chapters. In chapter 2, the most important evolutions from the last decades will be discussed, from digital transformation, Open Access, globalization, and the emergence of more interdisciplinary and participatory research approaches. In chapter 3, some common applications of social research for humanitarian and development contexts from recent years will be discussed, including key innovations in terms of new technologies, methods and tools. In chapter 4, the relationship between social research and policymaking will be analysed, exploring how research influences policy decisions and the key challenges and enablers in this process. Case studies to illustrate successful integrations of research into policymaking will also be discussed within this chapter. Finally, chapter 5 will be dedicated to the conclusions and recommendations, summarizing key takeaways, offering suggestions and highlighting remaining information gaps that need to be addressed for future research efforts, by IMPACT or similar organisations.
Related Content
Data-driven digital agriculture, ai in emergency response: not the time for experiments.
World + 22 more
Informe de la Representante Especial del Secretario General para la Cuestión de los Niños y los Conflictos Armados (A/79/245)
Bureau de la représentante spéciale du secrétaire général pour la question des enfants et des conflits armés (a/79/245).
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Limited evidence for the benefits of exercise in older adults with hematological malignancies: a systematic review and meta-analysis.

Simple Summary
1. introduction, 2. materials and methods, 2.1. information sources and search strategy, 2.2. eligibility criteria, 2.3. data collection process, 2.4. outcomes, 2.5. risk of bias assessment, 2.6. certainty of evidence, 2.7. data synthesis and analysis, 3.1. study characteristics, 3.2. exercise interventions, 3.3. effects of exercise interventions on primary outcomes, 3.4. effects of exercise interventions on secondary outcomes, 3.5. feasibility, adverse events, adherence and exclusion criteria, 3.6. risk of bias in individual studies and across studies, 3.7. quality of evidence (grade), 3.8. ongoing studies registered in clinical trials, 4. discussion, strengths and limitations, 5. conclusions, supplementary materials, author contributions, institutional review board statement, informed consent statement, acknowledgments, conflicts of interest.
- Fitzmaurice, C.; Akinyemiju, T.F.; Al Lami, F.H.; Alam, T.; Alizadeh-Navaei, R.; Allen, C.; Alsharif, U.; Alvis-Guzman, N.; Amini, E.; Anderson, B.O.; et al. Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-Years for 29 Cancer Groups, 1990 to 2016: A Systematic Analysis for the Global Burden of Disease Study. JAMA Oncol. 2019 , 5 , 1749–1768. [ Google Scholar ]
- Zhang, N.; Wu, J.; Wang, Q.; Liang, Y.; Li, X.; Chen, G.; Ma, L.; Liu, X.; Zhou, F. Global burden of hematologic malignancies and evolution patterns over the past 30 years. Blood Cancer J. 2023 , 13 , 82. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Howlader, N.A.; Krapcho, M.; Miller, D.; Brest, A.; Yu, M.; Ruhl, J.; Tatalovich, Z.; Mariotto, A.; Lewis, D.R.; Chen, H.S.; et al. (Eds.) SEER Cancer Statistics Review, 1975–2018, National Cancer Institute. Bethesda, MD. Based on November 2020 SEER Data Submission, Posted to the SEER Web Site. Available online: https://seer.cancer.gov/csr/1975_2018/ (accessed on 21 April 2021).
- Krok-Schoen, J.L.; Fisher, J.L.; Stephens, J.A.; Mims, A.; Ayyappan, S.; Woyach, J.A.; Rosko, A.E. Incidence and survival of hematological cancers among adults ages ≥75 years. Cancer Med. 2018 , 7 , 3425–3433. [ Google Scholar ] [ CrossRef ]
- Cordoba, R.; A Eyre, T.; Klepin, H.D.; Wildes, T.M.; Goede, V. Haematological Malignancies in Older People 1 A comprehensive approach to therapy of haematological malignancies in older patients. Lancet Haematol. 2021 , 8 , E840–E852. [ Google Scholar ] [ CrossRef ]
- Handforth, C.; Clegg, A.; Young, C.; Simpkins, S.; Seymour, M.T.; Selby, P.J.; Young, J. The prevalence and outcomes of frailty in older cancer patients: A systematic review. Ann. Oncol. 2015 , 26 , 1091–1101. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Cheng, K.K.; Lee, D.T. Effects of pain, fatigue, insomnia, and mood disturbance on functional status and quality of life of elderly patients with cancer. Crit. Rev. Oncol. Hematol. 2011 , 78 , 127–137. [ Google Scholar ] [ CrossRef ]
- Su, W.Y.E.; Chen, H.; Wu, M.; Lai, Y. Fatigue among older advanced cancer patients. Int. J. Gerontol. 2011 , 5 , 84–88. [ Google Scholar ] [ CrossRef ]
- Soones, T.; Ombres, R.; Escalante, C. An update on cancer-related fatigue in older adults: A narrative review. J. Geriatr. Oncol. 2022 , 13 , 125–131. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Wall, S.A.; Stevens, E.; Vaughn, J.; Bumma, N.; Rosko, A.E.; Borate, U. Multidisciplinary Approach to Older Adults with Hematologic Malignancies—A Paradigm Shift. Curr. Hematol. Malign- Rep. 2022 , 17 , 31–38. [ Google Scholar ] [ CrossRef ]
- Coelho, A.; Parola, V.; Cardoso, D.; Bravo, M.E.; Apóstolo, J. Use of non-pharmacological interventions for comforting patients in palliative care: A scoping review. JBI Database Syst. Rev. Implement Rep. 2017 , 15 , 1867–1904. [ Google Scholar ] [ CrossRef ]
- Abdelbasset, W.K.; Nambi, G.; Elsayed, S.H.; Osailan, A.M.; Eid, M.M. Falls and potential therapeutic interventions among elderly and older adult patients with cancer: A systematic review. Afr. Health Sci. 2021 , 21 , 1776–1783. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Brick, R.; Turner, R.; Bender, C.; Douglas, M.; Eilers, R.; Ferguson, R.; Leland, N.; Lyons, K.D.; Toto, P.; Skidmore, E. Impact of non-pharmacological interventions on activity limitations and participation restrictions in older breast cancer survivors: A scoping review. J. Geriatr. Oncol. 2022 , 13 , 132–142. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Cardoso, C.S.; Matos, J.R.; Prazeres, F.; Gomes, B. Non-pharmacological interventions in primary care to improve the quality of life of older patients with palliative care needs: A systematic review of randomised controlled trials. BMJ Open 2023 , 13 , e073950. [ Google Scholar ] [ CrossRef ]
- Pedersen, M.; Engedal, M.S.; Tolver, A.; Larsen, M.T.; Kornblit, B.T.; Lomborg, K.; Jarden, M. Effect of non-pharmacological interventions on symptoms and quality of life in patients with hematological malignancies—A systematic review. Crit. Rev. Oncol. 2024 , 196 , 104327. [ Google Scholar ] [ CrossRef ]
- Yang, Y.-P.; Pan, S.-J.; Qiu, S.-L.; Tung, T.-H. Effects of physical exercise on the quality-of-life of patients with haematological malignancies and thrombocytopenia: A systematic review and meta-analysis. World J. Clin. Cases 2022 , 10 , 3143–3155. [ Google Scholar ] [ CrossRef ]
- Großek, A.; Großek, K.; Bloch, W. Safety and feasibility of exercise interventions in patients with hematological cancer undergoing chemotherapy: A systematic review. Support. Care Cancer 2023 , 31 , 335. [ Google Scholar ] [ CrossRef ]
- Knips, L.; Bergenthal, N.; Streckmann, F.; Monsef, I.; Elter, T.; Skoetz, N. Aerobic physical exercise for adult patients with haematological malignancies. Cochrane Database Syst. Rev. 2019 , 2019 , CD009075. [ Google Scholar ] [ CrossRef ]
- Xu, W.; Yang, L.; Wang, Y.; Wu, X.; Wu, Y.; Hu, R. Effects of exercise interventions for physical fitness, fatigue, and quality of life in adult hematologic malignancy patients without receiving hematopoietic stem cell transplantation: A systematic review and meta-analysis. Support. Care Cancer 2022 , 30 , 7099–7118. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Abo, S.; Denehy, L.; Ritchie, D.; Lin, K.-Y.; Edbrooke, L.; McDonald, C.; Granger, C.L. People With Hematological Malignancies Treated With Bone Marrow Transplantation Have Improved Function, Quality of Life, and Fatigue Following Exercise Intervention: A Systematic Review and Meta-Analysis. Phys. Ther. 2021 , 101 , pzab130. [ Google Scholar ] [ CrossRef ]
- Moore, M.; Northey, J.M.; Crispin, P.; Semple, S.; Toohey, K. Effects of Exercise Rehabilitation on Physical Function in Adults With Hematological Cancer Receiving Active Treatment: A Systematic Review and Meta-Analysis. Semin. Oncol. Nurs. 2023 , 39 , 151504. [ Google Scholar ] [ CrossRef ]
- Izquierdo, M.; Merchant, R.A.; Morley, J.E.; Anker, S.D.; Aprahamian, I.; Arai, H.; Aubertin-Leheudre, M.; Bernabei, R.; Cadore, E.L.; Cesari, M.; et al. International Exercise Recommendations in Older Adults (ICFSR): Expert Consensus Guidelines. J. Nutr. Health Aging 2021 , 25 , 824–853. [ Google Scholar ] [ CrossRef ]
- Chodzko-Zajko, W.J.; Proctor, D.N.; Fiatarone Singh, M.A.; Minson, C.T.; Nigg, C.R.; Salem, G.J.; Skinner, J.S. Exercise and Physical Activity for Older Adults. Med. Sci. Sports Exerc. 2009 , 41 , 1510–1530. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Kilari, D.; Soto-Perez-De-Celis, E.; Mohile, S.G.; Alibhai, S.M.; Presley, C.J.; Wildes, T.M.; Klepin, H.D.; Demark-Wahnefried, W.; Jatoi, A.; Harrison, R.; et al. Designing exercise clinical trials for older adults with cancer: Recommendations from 2015 Cancer and Aging Research Group NCI U13 Meeting. J. Geriatr. Oncol. 2016 , 7 , 293–304. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Campbell, K.L.; Winters-Stone, K.M.; Wiskemann, J.; May, A.M.; Schwartz, A.L.; Courneya, K.S.; Zucker, D.S.; Matthews, C.E.; Ligibel, J.A.; Gerber, L.H.; et al. Exercise Guidelines for Cancer Survivors: Consensus Statement from International Multidisciplinary Roundtable. Med. Sci. Sports Exerc. 2019 , 51 , 2375–2390. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Klepin, H.D.; Mohile, S.G.; Exterman, S.M.M.; Karger, S. (Eds.) Cancer and Aging: From Bench to Clinics. Exercise for Older Cancer Patients: Feasible and Helpful? 2012; Available online: https://karger.com/books/book/241/chapter-abstract/5166165/Exercise-for-Older-Cancer-Patients-Feasible-and?redirectedFrom=PDF (accessed on 11 July 2024).
- Higgins, J.P.T.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.J.; Welch, V.A.; Cochrane (Eds.) Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 ; 2023; Available online: https://training.cochrane.org/handbook (accessed on 11 July 2024).
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetz-laff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021 , 372 , 71. [ Google Scholar ] [ CrossRef ]
- Rethlefsen, M.L.; Kirtley, S.; Waffenschmidt, S.; Ayala, A.P.; Moher, D.; Page, M.J.; Koffel, J.B.; PRISMA-S Group. PRISMA-S: An extension to the PRISMA Statement for Reporting Literature Searches in Systematic Reviews. Syst. Rev. 2021 , 10 , 39. [ Google Scholar ] [ CrossRef ]
- Schardt, C.; Adams, M.B.; Owens, T.; Keitz, S.; Fontelo, P. Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med. Inform. Decis. Mak. 2007 , 7 , 16. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Sterne, J.A.C.; Savović, J.; Page, M.J.; Elbers, R.G.; Blencowe, N.S.; Boutron, I.; Cates, C.J.; Cheng, H.Y.; Corbett, M.S.; Eldridge, S.M.; et al. RoB 2: A revised tool for assessing risk of bias in randomised trials. BMJ 2019 , 366 , l4898. [ Google Scholar ] [ CrossRef ]
- Ryan, R.H.S. How to GRADE the Quality of the Evidence. Cochrane Consumers and Communication Group Version 3.0. Available online: http://cccrg.cochrane.org/author-resources (accessed on 1 January 2020).
- Garber, C.E.; Blissmer, B.; Deschenes, M.R.; Franklin, B.A.; LaMonte, M.J.; Lee, I.-M.; Nieman, D.C.; Swain, D.P. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: Guidance for prescribing exercise. Med. Sci. Sport. Exerc. 2011 , 43 , 1334–1359. [ Google Scholar ] [ CrossRef ]
- Andersen, H.H.; Vinther, A.; Lund, C.M.; Paludan, C.; Jørgensen, C.T.; Nielsen, D.; Juhl, C.B. Effectiveness of different types, delivery modes and extensiveness of exercise in patients with breast cancer receiving systemic treatment—A systematic review and meta-analysis. Crit. Rev. Oncol. 2022 , 178 , 103802. [ Google Scholar ] [ CrossRef ]
- Ramírez-Vélez, R.; Zambom-Ferraresi, F.; García-Hermoso, A.; Kievisiene, J.; Rauckiene-Michealsson, A.; Agostinis-Sobrinho, C. Evidence-Based Exercise Recommendations to Improve Mental Wellbeing in Women with Breast Cancer during Active Treatment: A Systematic Review and Meta-Analysis. Cancers 2021 , 13 , 264. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Accogli, M.A.; Denti, M.; Costi, S.; Fugazzaro, S. Therapeutic education and physical activity are feasible and safe in hematologic cancer patients referred to chemotherapy: Results of a randomized controlled trial. Support. Care Cancer 2022 , 31 , 61. [ Google Scholar ] [ CrossRef ]
- Alibhai, S.M.H.; O’neill, S.; Fisher-Schlombs, K.; Breunis, H.; Timilshina, N.; Brandwein, J.M.; Minden, M.D.; Tomlinson, G.A.; Culos-Reed, S.N. A pilot phase II RCT of a home-based exercise intervention for survivors of AML. Support. Care Cancer 2014 , 22 , 881–889. [ Google Scholar ] [ CrossRef ]
- Alibhai, S.; Durbano, S.; Breunis, H.; Brandwein, J.; Timilshina, N.; Tomlinson, G.; Oh, P.; Culos-Reed, S. A phase II exercise randomized controlled trial for patients with acute myeloid leukemia undergoing induction chemotherapy. Leuk. Res. 2015 , 39 , 1178–1186. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Baumann, F.T.; Kraut, L.; Schüle, K.; Bloch, W.; A Fauser, A. A controlled randomized study examining the effects of exercise therapy on patients undergoing haematopoietic stem cell transplantation. Bone Marrow Transplant. 2010 , 45 , 355–362. [ Google Scholar ] [ CrossRef ]
- Baumann, F.T.; Zopf, E.M.; Nykamp, E.; Kraut, L.; Schüle, K.; Elter, T.; Fauser, A.A.; Bloch, W. Physical activity for patients undergoing an allogeneic hematopoietic stem cell transplantation: Benefits of a moderate exercise intervention. Eur. J. Haematol. 2011 , 87 , 148–156. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Bayram, S.; Barğı, G.; Çelik, Z.; Güçlü, M.B. Effects of pulmonary rehabilitation in hematopoietic stem cell transplantation recipients: A randomized controlled study. Support. Care Cancer 2024 , 32 , 72. [ Google Scholar ] [ CrossRef ]
- Bird, L.; Arthur, A.; Niblock, T.; Stone, R.; Watson, L.; Cox, K. Rehabilitation programme after stem cell transplantation: Randomized controlled trial. J. Adv. Nurs. 2010 , 66 , 607–615. [ Google Scholar ] [ CrossRef ]
- Bryant, A.L.; Deal, A.M.; Battaglini, C.L.; Phillips, B.; Pergolotti, M.; Coffman, E.; Foster, M.C.; Wood, W.A.; Bailey, C.; Hackney, A.C.; et al. The Effects of Exercise on Patient-Reported Outcomes and Performance-Based Physical Function in Adults With Acute Leukemia Undergoing Induction Therapy: Exercise and Quality of Life in Acute Leukemia (EQUAL). Integr. Cancer Ther. 2018 , 17 , 263–270. [ Google Scholar ] [ CrossRef ]
- Chang, P.-H.; Lai, Y.-H.; Shun, S.-C.; Lin, L.-Y.; Chen, M.-L.; Yang, Y.; Tsai, J.-C.; Huang, G.-S.; Cheng, S.-Y. Effects of a Walking Intervention on Fatigue-Related Experiences of Hospitalized Acute Myelogenous Leukemia Patients Undergoing Chemotherapy: A Randomized Controlled Trial. J. Pain Symptom Manag. 2008 , 35 , 524–534. [ Google Scholar ] [ CrossRef ]
- Chen, F.; Mao, L.; Wang, Y.; Xu, J.; Li, J.; Zheng, Y. The Feasibility and Efficacy of Self-help Relaxation Exercise in Symptom Distress in Patients With Adult Acute Leukemia: A Pilot Randomized Controlled Trial. Pain Manag. Nurs. 2021 , 22 , 791–797. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Chow, E.J.; Doody, D.R.; Di, C.; Armenian, S.H.; Baker, K.S.; Bricker, J.B.; Gopal, A.K.; Hagen, A.M.; Ketterl, T.G.; Lee, S.J.; et al. Feasibility of a behavioral intervention using mobile health applications to reduce cardiovascular risk factors in cancer survivors: A pilot randomized controlled trial. J. Cancer Surviv. 2021 , 15 , 554–563. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Chuang, T.-Y.; Yeh, M.-L.; Chung, Y.-C. A nurse facilitated mind-body interactive exercise (Chan-Chuang qigong) improves the health status of non-Hodgkin lymphoma patients receiving chemotherapy: Randomised controlled trial. Int. J. Nurs. Stud. 2017 , 69 , 25–33. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Cohen, L.; Warneke, C.; Fouladi, R.T.; Rodriguez, M.A.; Chaoul-Reich, A. Psychological adjustment and sleep quality in a randomized trial of the effects of a Tibetan yoga intervention in patients with lymphoma. Cancer 2004 , 100 , 2253–2260. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Coleman, E.A.; Coon, S.; Hall-Barrow, J.; Richards, K.; Gaylor, D.; Stewart, B. Feasibility of Exercise During Treatment for Multiple Myeloma. Cancer Nurs. 2003 , 26 , 410–419. [ Google Scholar ] [ CrossRef ]
- Coleman, E.A.; Goodwin, J.A.; Kennedy, R.; Coon, S.K.; Richards, K.; Enderlin, C.; Stewart, C.B.; McNatt, P.; Lockhart, K.; Anaissie, E.J. Effects of Exercise on Fatigue, Sleep, and Performance: A Randomized Trial. Oncol. Nurs. Forum 2012 , 39 , 468–477. [ Google Scholar ] [ CrossRef ]
- Courneya, K.S.; Sellar, C.M.; Stevinson, C.; McNeely, M.L.; Peddle, C.J.; Friedenreich, C.M.; Tankel, K.; Basi, S.; Chua, N.; Mazurek, A.; et al. Randomized Controlled Trial of the Effects of Aerobic Exercise on Physical Functioning and Quality of Life in Lymphoma Patients. J. Clin. Oncol. 2009 , 27 , 4605–4612. [ Google Scholar ] [ CrossRef ]
- DeFor, T.E.; Burns, L.J.; Gold, E.-M.A.; Weisdorf, D.J. A Randomized Trial of the Effect of a Walking Regimen on the Functional Status of 100 Adult Allogeneic Donor Hematopoietic Cell Transplant Patients. Biol. Blood Marrow Transplant. 2007 , 13 , 948–955. [ Google Scholar ] [ CrossRef ]
- Eckert, R.; Huberty, J.; Kurka, J.; Laird, B.; Mesa, R.; Palmer, J. A Randomized Pilot Study of Online Hatha Yoga for Physical and Psychological Symptoms Among Survivors of Allogenic Bone Marrow Transplant. Int. J. Yoga Ther. 2022 , 32 , 12. [ Google Scholar ] [ CrossRef ]
- Furzer, B.J.; Ackland, T.R.; Wallman, K.E.; Petterson, A.S.; Gordon, S.M.; Wright, K.E.; Joske, D.J.L. A randomised controlled trial comparing the effects of a 12-week supervised exercise versus usual care on outcomes in haematological cancer patients. Support. Care Cancer 2016 , 24 , 1697–1707. [ Google Scholar ] [ CrossRef ]
- Gallardo-Rodríguez, A.G.; Fuchs-Tarlovsky, V.; Ocharán-Hernández, M.E.; Ramos-Peñafiel, C.O. Cross-Training and Resistance Training in Adults with Type B Acute Lymphoblastic Leukemia during the Induction Phase: A Randomized Blind Pilot Study. J. Clin. Med. 2023 , 12 , 5008. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hacker, E.D.; Collins, E.; Park, C.; Peters, T.; Rondelli, D. Strength training to enhance early recovery after hematopoietic stem cell transplantation. J. Clin. Oncol. 2016 , 34 , 190. [ Google Scholar ] [ CrossRef ]
- Hacker, E.D.P.; Richards, R.L.; Abu Zaid, M.; Chung, S.-Y.; Perkins, S.; Farag, S.S. STEPS to Enhance Physical Activity After Hematopoietic Cell Transplantation for Multiple Myeloma. Cancer Nurs. 2022 , 45 , 211–223. [ Google Scholar ] [ CrossRef ]
- Hathiramani, S.; Pettengell, R.; Moir, H.; Younis, A. Relaxation versus exercise for improved quality of life in lymphoma survivors—A randomised controlled trial. J. Cancer Surviv. 2021 , 15 , 470–480. [ Google Scholar ] [ CrossRef ]
- Huberty, J.; Eckert, R.; Dueck, A.; Kosiorek, H.; Larkey, L.; Gowin, K.; Mesa, R. Online yoga in myeloproliferative neoplasm patients: Results of a randomized pilot trial to inform future research. BMC Complement. Altern. Med. 2019 , 19 , 121. [ Google Scholar ] [ CrossRef ]
- Hung, Y.-C.; Bauer, J.D.; Horsely, P.; Coll, J.; Bashford, J.; A Isenring, E. Telephone-delivered nutrition and exercise counselling after auto-SCT: A pilot, randomised controlled trial. Bone Marrow Transplant. 2014 , 49 , 786–792. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Jacobsen, P.B.; Le-Rademacher, J.; Jim, H.; Syrjala, K.; Wingard, J.R.; Logan, B.; Wu, J.; Majhail, N.S.; Wood, W.; Rizzo, J.D.; et al. Exercise and Stress Management Training Prior to Hematopoietic Cell Transplantation: Blood and Marrow Transplant Clinical Trials Network (BMT CTN) 0902. Biol. Blood Marrow Transplant. 2014 , 20 , 1530–1536. [ Google Scholar ] [ CrossRef ]
- Jarden, M.; Baadsgaard, M.T.; Hovgaard, D.J.; Boesen, E.; Adamsen, L. A randomized trial on the effect of a multimodal intervention on physical capacity, functional performance and quality of life in adult patients undergoing allogeneic SCT. Bone Marrow Transplant. 2009 , 43 , 725–737. [ Google Scholar ] [ CrossRef ]
- Jarden, M.; Møller, T.; Christensen, K.B.; Kjeldsen, L.; Birgens, H.S.; Adamsen, L. Multimodal intervention integrated into the clinical management of acute leukemia improves physical function and quality of life during consolidation chemotherapy: A randomized trial ‘PACE-AL. Haematologica 2016 , 101 , e316–e319. [ Google Scholar ] [ CrossRef ]
- Kim, S.-D.; Kim, H.-S. Effects of a Relaxation Breathing Exercise on Anxiety, Depression, and Leukocyte in Hemopoietic Stem Cell Transplantation Patients. Cancer Nurs. 2005 , 28 , 79–83. [ Google Scholar ] [ CrossRef ]
- Knols, R.H.; de Bruin, E.D.; Uebelhart, D.; Aufdemkampe, G.; Schanz, U.; Stenner-Liewen, F.; Hitz, F.; Taverna, C.; Aaronson, N.K. Effects of an outpatient physical exercise program on hematopoietic stem-cell transplantation recipients: A randomized clinical trial. Bone Marrow Transplant. 2011 , 46 , 1245–1255. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Kobayashi, D.; Watanabe, R.; Yamamoto, M.; Kizaki, M. Efficacy of physical exercise using the balance board game on physical and psychological function in patients with hematological malignancies confined to a bioclean room. Phys. Ther. Res. 2020 , 23 , 172–179. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Koutoukidis, D.A.; Land, J.; Hackshaw, A.; Heinrich, M.; McCourt, O.; Beeken, R.J.; Philpott, S.; DeSilva, D.; Rismani, A.; Rabin, N.; et al. Fatigue, quality of life and physical fitness following an exercise intervention in multiple myeloma survivors (MASCOT): An exploratory randomised Phase 2 trial utilising a modified Zelen design. Br. J. Cancer 2020 , 123 , 187–195. [ Google Scholar ] [ CrossRef ]
- McCourt, O.; Fisher, A.; Ramdharry, G.; Land, J.; Roberts, A.L.; Rabin, N.; Yong, K. Exercise prehabilitation for people with myeloma undergoing autologous stem cell transplantation: Results from PERCEPT pilot randomised controlled trial. Acta Oncol. 2023 , 62 , 696–705. [ Google Scholar ] [ CrossRef ]
- Mello, M.; Tanaka, C.; Dulley, F.L. Effects of an exercise program on muscle performance in patients undergoing allogeneic bone marrow transplantation. Bone Marrow Transplant. 2003 , 32 , 723–728. [ Google Scholar ] [ CrossRef ]
- Oechsle, K.; Aslan, Z.; Suesse, Y.; Jensen, W.; Bokemeyer, C.; de Wit, M. Multimodal exercise training during myeloablative chemotherapy: A prospective randomized pilot trial. Support. Care Cancer 2014 , 22 , 63–69. [ Google Scholar ] [ CrossRef ]
- Pahl, A.; Wehrle, A.; Kneis, S.; Gollhofer, A.; Bertz, H. Feasibility of whole body vibration during intensive chemotherapy in patients with hematological malignancies—A randomized controlled pilot study. BMC Cancer 2018 , 18 , 920. [ Google Scholar ] [ CrossRef ]
- Pahl, A.; Wehrle, A.; Kneis, S.; Gollhofer, A.; Bertz, H. Whole body vibration training during allogeneic hematopoietic cell transplantation—The effects on patients’ physical capacity. Ann. Hematol. 2020 , 99 , 635–648. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Persoon, S.; ChinAPaw, M.J.M.; Buffart, L.M.; Liu, R.D.K.; Wijermans, P.; Koene, H.R.; Minnema, M.C.; Lugtenburg, P.J.; Marijt, E.W.A.; Brug, J.; et al. Randomized controlled trial on the effects of a supervised high intensity exercise program in patients with a hematologic malignancy treated with autologous stem cell transplantation: Results from the EXIST study. PLoS ONE 2017 , 12 , e0181313. [ Google Scholar ] [ CrossRef ]
- Potiaumpai, M.; Cutrono, S.; Medina, T.; Koeppel, M.; Pereira, D.L.; Pirl, W.F.; Jacobs, K.A.; Eltoukhy, M.; Signorile, J.F. Multidirectional Walking in Hematopoietic Stem Cell Transplant Patients. Med. Sci. Sports Exerc. 2021 , 53 , 258–266. [ Google Scholar ] [ CrossRef ]
- Safran, E.E.; Mutluay, F.; Uzay, A. Effects of neuromuscular electrical stimulation combined with resistance exercises on muscle strength in adult hematological cancer patients: A randomized controlled study. Leuk. Res. 2022 , 121 , 106932. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Schumacher, H.; Stüwe, S.; Kropp, P.; Diedrich, D.; Freitag, S.; Greger, N.; Junghanss, C.; Freund, M.; Hilgendorf, I. A prospective, randomized evaluation of the feasibility of exergaming on patients undergoing hematopoietic stem cell transplantation. Bone Marrow Transplant. 2018 , 53 , 584–590. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Shelton, M.L.; Lee, J.Q.; Morris, G.S.; Massey, P.R.; Kendall, D.G.; Munsell, M.F.; Anderson, K.O.; Simmonds, M.J.; Giralt, S.A. A randomized control trial of a supervised versus a self-directed exercise program for allogeneic stem cell transplant patients. Psycho-Oncol. 2009 , 18 , 353–359. [ Google Scholar ] [ CrossRef ]
- Streckmann, F.; Kneis, S.; Leifert, J.A.; Baumann, F.T.; Kleber, M.; Ihorst, G.; Herich, L.; Grüssinger, V.; Gollhofer, A.; Bertz, H. Exercise program improves therapy-related side-effects and quality of life in lymphoma patients undergoing therapy. Ann. Oncol. 2014 , 25 , 493–499. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Vallerand, J.R.; Rhodes, R.E.; Walker, G.J.; Courneya, K.S. Feasibility and preliminary efficacy of an exercise telephone counseling intervention for hematologic cancer survivors: A phase II randomized controlled trial. J. Cancer Surviv. 2018 , 12 , 357–370. [ Google Scholar ] [ CrossRef ]
- Waked, I.S. A Randomized Controlled Trial of the Effects of Supervised Aerobic Training Program on Anthropometry, Lipid Profile and Body Composition in Obese Adult Leukemic Patients. Iran. J. Blood Cancer 2019 , 11 , 26–32. [ Google Scholar ]
- Wehrle, A.; Kneis, S.; Dickhuth, H.-H.; Gollhofer, A.; Bertz, H. Endurance and resistance training in patients with acute leukemia undergoing induction chemotherapy—A randomized pilot study. Support. Care Cancer 2019 , 27 , 1071–1079. [ Google Scholar ] [ CrossRef ]
- Wiskemann, J.; Dreger, P.; Schwerdtfeger, R.; Bondong, A.; Huber, G.; Kleindienst, N.; Ulrich, C.M.; Bohus, M. Effects of a partly self-administered exercise program before, during, and after allogeneic stem cell transplantation. Blood 2011 , 117 , 2604–2613. [ Google Scholar ] [ CrossRef ]
- Wood, W.A.; Weaver, M.; Smith-Ryan, A.E.; Hanson, E.D.; Shea, T.C.; Battaglini, C.L. Lessons learned from a pilot randomized clinical trial of home-based exercise prescription before allogeneic hematopoietic cell transplantation. Support. Care Cancer 2020 , 28 , 5291–5298. [ Google Scholar ] [ CrossRef ]
- Yeh, M.-L.; Chung, Y.-C. A randomized controlled trial of qigong on fatigue and sleep quality for non-Hodgkin’s lymphoma patients undergoing chemotherapy. Eur. J. Oncol. Nurs. 2016 , 23 , 81–86. [ Google Scholar ] [ CrossRef ]
- Jarden, M.; Møller, T.; Christensen, K.B.; Buchardt, A.; Kjeldsen, L.; Adamsen, L. Longitudinal symptom burden in adult patients with acute leukaemia participating in the PACE-AL randomised controlled exercise trial—An explorative analysis. Eur. J. Cancer Care 2021 , 30 , e13462. [ Google Scholar ] [ CrossRef ]
- Wiskemann, J.; Kuehl, R.; Dreger, P.; Schwerdtfeger, R.; Huber, G.; Ulrich, C.M.; Jaeger, D.; Bohus, M. Efficacy of exercise training in SCT patients-who benefits most? Bone Marrow Transplant. 2014 , 49 , 443–448. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Knowles, R.; Kemp, E.; Miller, M.; Davison, K.; Koczwara, B. Physical activity interventions in older people with cancer: A review of systematic reviews. Eur. J. Cancer Care 2022 , 31 , e13637. [ Google Scholar ] [ CrossRef ]
- Mikkelsen, M.K.; Juhl, C.B.; Lund, C.M.; Jarden, M.; Vinther, A.; Nielsen, D.L. The effect of exercise-based interventions on health-related quality of life and physical function in older patients with cancer receiving medical antineoplastic treatments: A systematic review. Eur. Rev. Aging Phys. Act. 2020 , 17 , 18. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Sheill, G.; Guinan, E.; Brady, L.; Hevey, D.; Hussey, J. Exercise interventions for patients with advanced cancer: A systematic review of recruitment, attrition, and exercise adherence rates. Palliat. Support. Care 2019 , 17 , 686–696. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Allen, N.E.; Sherrington, C.; Suriyarachchi, G.D.; Paul, S.S.; Song, J.; Canning, C.G. Exercise and motor training in people with Parkinson’s disease: A systematic review of participant characteristics, intervention delivery, retention rates, adherence, and adverse events in clinical trials. Park. Dis. 2011 , 2012 , 854328. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Jansons, P.S.; Haines, T.P.; O’brien, L. Interventions to achieve ongoing exercise adherence for adults with chronic health conditions who have completed a supervised exercise program: Systematic review and meta-analysis. Clin. Rehabil. 2017 , 31 , 465–477. [ Google Scholar ] [ CrossRef ]
- Larsen, R.F.; Jarden, M.; Minet, L.R.; Frølund, U.C.; Abildgaard, N. Supervised and home-based physical exercise in patients newly diagnosed with multiple myeloma-a randomized controlled feasibility study. Pilot Feasibility Stud. 2019 , 5 , 130. [ Google Scholar ] [ CrossRef ]
- Rosko, A.; Huang, Y.; Jones, D.; Presley, C.J.; Jaggers, J.; Owens, R.; Naughton, M.; Krok-Schoen, J.L. Feasibility of implementing an exercise intervention in older adults with hematologic malignancy. J. Geriatr. Oncol. 2022 , 13 , 234–240. [ Google Scholar ] [ CrossRef ]
- Mazzoni, A.-S.; Brooke, H.L.; Berntsen, S.; Nordin, K.; Demmelmaier, I. Exercise Adherence and Effect of Self-Regulatory Behavior Change Techniques in Patients Undergoing Curative Cancer Treatment: Secondary Analysis from the Phys-Can Randomized Controlled Trial. Integr. Cancer Ther. 2020 , 19 , 1534735420946834. [ Google Scholar ] [ CrossRef ]
- Collado-Mateo, D.; Lavín-Pérez, A.; Peñacoba, C.; Del Coso, J.; Leyton-Román, M.; Luque-Casado, A.; Gasque, P.; Fernández-Del-Olmo, M.; Amado-Alonso, D. Key Factors Associated with Adherence to Physical Exercise in Patients with Chronic Diseases and Older Adults: An Umbrella Review. Int. J. Environ. Res. Public Health 2021 , 18 , 2023. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Colton, A.; Smith, M.A.; Broadbent, S.; Rune, K.T.; Wright, H.H. Perceptions of Older Adults with Hematological Cancer on Diet and Exercise Behavior and Its Role in Navigating Daily Tasks. Int. J. Environ. Res. Public Health 2022 , 19 , 15044. [ Google Scholar ] [ CrossRef ] [ PubMed ]
Click here to enlarge figure
| Author, Year, Country | Diagnose | Study Design | Sample Size, n IG/CG Female (%) | Age Mean, (Range) Median, (Range) | Exclusion Criteria | Timing of Intervention | Intervention Group | Control Group | |
|---|---|---|---|---|---|---|---|---|---|
| Type: T Intensity: I Length: L Duration: D | Extensiveness | Type: T Intensity: I Length: L Duration: D | |||||||
| Accogli 2022 Italy [ ] | Lymph, Leuk, MM | RCT | 46 (23/23) (47.8) | Mean 59.9 Median IG: 66.7 (51.3–72.1) CG: 60.4 (49.9–67.5) | Poor prognosis (<12 months) and clinical conditions hindering participation (e.g., dementia, psychiatric pathology, blindness) | Before, during and after chemotherapy | Supervised, hospital-based: T: Therapeutic education I: Individual intensity L: 2 × 60 min (group) and face-to-face (individual) 6 × 20 min 1x/week or every 2 weeks Unsupervised, homebased: T: Individual physical exercise D: 8 weeks | Less | T: Educational therapeutic group sessions L: 2x in total |
| Alibhai 2014 Canada [ ] | AML | RCT Feasibility | 38 (21/17) (55.3) | Mean 56.1 IG: 53.9 CG: 58.8 | Another active malignancy, life expectancy < 3 months, severe or unstable cardiorespiratory or musculoskeletal disease, awaiting HSCT and regular participation in a moderate-vigorous PA program | After HSCT or chemotherapy | Supervised, hospital-based: T: Workout and education (group) L: 1.5 h/week Unsupervised, home-based: T: Aerobic, resistance and flexibility components I: Moderate intensity L: 30 min, 3–5x/week D: 12 weeks | Moderate | T: UC, Usual level of PA |
| Alibhai 2015 Canada [ ] | AML | RCT | 81 (57/24) (45.7) | Mean 57 (23–80) IG: 58 CG: 52 Median 59 >60: IG, n = 32 CG, n = 7 | Another active malignancy, life expectancy < 1-month, significant medical comorbidity that would preclude exercise, uncontrolled pain, hemo-dynamic instability | During chemotherapy | , hospital-based: T: Individualized aerobic (treadmill, hall walking, stationary cycling), resistance (body weight, bands, free weights) and flexibility training I: RPE of 3–6, equivalent to 50–75% of HRR L: 30–60 min, 4–5x/week | Moderate | T: UC, Suggestions to walk regularly and weekly document on tracking sheets |
| Baumann 2010 Germany [ ] | AML, ALL, CML, MM, NHL/CLL, MDS/MPS, Solid tumor, Immuno-deficiency | RCT Pilot | 64 32/32 (45.4) | Mean IG: 44.9 CG: 44.1 | Severe orthopaedic illness of legs, severe heart failure (NYHA III-IV), metastatic bone disease, thrombocytopenia (≤30 × 10 /L) and/or acute somatic complaint (e.g., infection, fever, acute bleeding) | During ASCT, allo-HSCT or chemotherapy | hospital-based: T: Aerobic (ergometer) and ADL training (walking, stepping, stretching) I: Aerobic: 80% of achieved watt load in WHO-test, ADL-training: Borg scale: “slighty strenuous”-“strenuous” L: Aerobic 10–20 min + ADL 20 min/2x daily, ADL 5x/week D: Mean: 26.6 days | Moderate | T: UC, Standard mobilization program |
| Baumann 2011 Germany [ ] | AML ALL, CML, CLL, MPS, MDS, CMML, MM, PID | RCT | 47 (24/23) (51.5) | Mean IG: 41.4 CG: 42.8 | Severe cardiac disease (NYHA III-IV) or orthopaedic illness of the legs, bone metastases, thrombocytopenia (≤10 × 10 /L) or acute bleeding, respectively, and/or acute health or somatic complaints (e.g., infection, fever) | During allo-HSCT | hospital-based: T: Aerobic (ergometer) and ADL training (walking, stepping, stretching) I: Aerobic: 80% of achieved watt load in WHO-test, ADL-training: Borg scale: “slighty strenuous”-”strenuous L: Aerobic: 10–20 min + ADL 20 min, 1–2x/day D: Mean: 56.1 days | Moderate | T: UC, Standard PT |
| Bayram 2024 Turkey [ ] | ALL, AML, Biphenotypic Leuk, MDS, NHL, Burkitt Lymph, CNS Lymph, Myelofibrosis, Thalassemia major, MM | RCT | 30 (15/15) (26.7) | Mean IG: 45.67 CG: 52.07 | Orthopaedic, neurological, or cognitive disease affecting functional capacity, psychiatric disorders, pneumonia, acute infections, sepsis, and pulmonary diseases | During HSCT | hospital-based: T: Aerobic (arm ergometer), resistance (free weights) and inspiratory muscle (inspiratory pressure device) exercises I: Aerobic: 50–80% of HR. Resistance: 4–6 on modified Borg scale, 3 sets of 10 reps. Inspiratory: 30% of max inspiratory pressure L: Aerobic: 10–30 min, 1x/day, 5 days/week. Resistance: 10–15 min, 5 days/week. Inspiratory: 15 min, 2x/day, 5 days/week D: During inpatient period. Mean: 25.2 days | Extensive | T: Aerobic and resistance exercises I: As IG L: As IG D: During inpatient period. Mean: 21.33 days |
| Bird 2010 UK [ ] | Leuk, Lymph, MM, other | RCT | 58 (29/29) (34.5) | Median 55 IG: 57 CG:52 | NR | After ASCT or allo-HSCT | hospital-based: T: Circuit training exercise, relaxation, and information (group) I: NR L: 1x/week D: 10 weeks | Less | T: UC, Self-managed program: information leaflets and home-based exercise program |
| Bryant 2018 USA [ ] | AML, ALL | RCT Pilot | 18 (9/9) (29.4) | Mean IG: 52 (34–67) CG: 49 (28–69) Median IG: 58 (34–67) CG: 48 (28–69) | Cardiovasc. disease, acute or chronic respiratory disease, acute or chronic bone, muscle, or joint abnormalities, altered mental state, dementia or any other psychological condition, another active malignancy, active bleeding, acute thrombosis, ischemia, hemodynamic instability, or uncontrolled pain | During chemotherapy | hospital-based: T: Aerobic (walking or stationary bike) and resistance training (resistance band) I: Aerobic: 50–70% of HRR. Resistance: Increased from lighter to heavier resistance, 10 RM L: 20–40 min, 2x/day, 4x/week D: 4 weeks | Moderate | T: UC |
| Chang 2008 Taiwan [ ] | AML | RCT | 24 (12/12) (45.5) | Mean IG: 49.4 CG: 53.3 | NR | During chemotherapy | hospital-based: T: Walking exercise program I: A speed to reach target HR (resting heart rate plus 30) L: 12 min, 5x/week D: 3 weeks | Less | T: Nurse-led control L/D: 1x/day, 5 days/week, 3 weeks |
| Chen 2021 China [ ] | AML, ALL | RCT Pilot | 30 (15/15) (58.6) | Mean IG: 40.2 CG: 37.6 | Medical conditions in arms, legs, or abdomen, paralysis, or disability and intended to receive HSCT in the next 3 months | During chemotherapy | , hospital-based T: Individualized self-help relaxation exercises I: NR L: 30 min, 2x daily D: 4 weeks | Less | T: UC |
| Chow 2020 USA [ ] | Leuk, Lymph, other | RCT Pilot | 41 (24/17) (48.8) | Median 45.1 (20.2–54.8) IG: 44.0 (20.9–54.0) CG: 46.0 (20.2–54.8) | Pre-existing ischemic heart disease or ongoing symptomatic cardiomyopathy, active cGvHD, pregnant | After ASCT, allo-HSCT | , home-based: T: Individualized, multiple mHealth app-based lifestyle counselling and goal-setting intervention, step count goals based on the past week’s daily average steps I: NR L: 16 weeks | Less | T: Fitbit tracker and Healthwatch360 app, no goal setting or peer support |
| Chuang 2017 Taiwan [ ] | NHL | RCT | 100 (50/50) (45.0) | Mean IG: 55.9 CG: 64.5 | Major medical disease, MM, or bone metastasis with medical contra-indications for exercise and already practicing qigong or other exercise regular | During chemotherapy | , home-based: T: Chan-Chuang qigong program with weekly telephone calls I: NR L: 25 min, 2–3x/day D: 21 consecutive days | Less | T: UC, Nursing on side effects of chemotherapy and care |
| Cohen 2004 USA [ ] | Lymph, HL, NHL | RCT | 39 (20/19) (30.8) | Mean 51 | Major psychotic illness, <18 years | During and after chemotherapy | , hospital-based: T: Group-based Tibetan yoga program I: NR L: 7x/week D: 7 weeks | Less | T: UC |
| Coleman 2003 USA [ ] | MM | RCT Pilot Feasibility | 24 (14/10) (41.7) | Mean 55 (42–74) | NR | During chemotherapy and ASCT | , home-based: T: Aerobic (walking, running, or cycling) and strength training (exercise bands), exercise log I: Borg Scale 12–15 L: Approx. 50 min, individual frequency D: 26 weeks | Moderate | T: UC, Encouragement to remain active and walk |
| Coleman 2012 USA [ ] | MM | RCT | 187 (95/92) (41.7) | Mean IG: 56.0 (25–76) CG: 56.4 (35–76) | Unable to understand intent of the study, major psychiatric illness, or presence of microcytic or macrocytic anaemia, uncontrolled hypertension, RBC transfusions within two weeks of study enrolment, or recombinant epoetin alfa within eight weeks of study enrolment | During unspecified intensive treatment (PBSCT) | , home-based: T: Individualized combination of stretching, aerobic exercise (walk, jog on treadmills) and strength resistance training (exercise bands), exercise log I: Aerobic:65–80% max HR, Borg Scale 11–13. Strength: 60–80% of 1 RM L: Individual length and frequency D: 15 weeks | Moderate | T: UC, Recommendation to walk L: 20 min, 3x/week |
| Courneya 2009 Canada [ ] | Lymph, NHL indolent, NHL aggressive, HL | RCT | 122 (60/62) (41) | Mean 53.2 (18–80) >60: n = 49 | Uncontrolled hypertension, cardiac illness, resides >80 km from facility, not approved by oncologist | Before, during and after chemotherapy | , hospital-based: T: Aerobic (ergometer) I: Initial 60% of VO peak, progressing 75% L: 15–45 min, 3x/week D: 12 weeks | Moderate | T: UC, Supervised exercise L: 12 sessions, 1 month, after postintervention assessments |
| Defor 2007 USA [ ] | AA, ALL, AML, MDS, CML, NHL/HL, other malignancies | RCT | 100 (51/49) (39.0) | Median 47 (18–68) IG: 46 (18–68) CG: 49 (22–64) | Unavailable treadmills at hospital admission (n = 21 excluded) | During and after allo-HSCT From transplant admission to day 100 posttransplant | Supervised, hospital-based: T: Individualized treadmill I: Comfortable speed L: 15 min, 2x/day , homebased: T: Walking I: Comfortable speed L: 30 min, 1x/day | Moderate | T: UC, Not asked to perform any formal exercise |
| Eckert 2022 USA [ ] | BMT patients | RCT Feasibility | 72 (33/39) (55.6) | NR | Engaged in yoga in past year, history of recurrent falls (>two falls in 2 months), residency outside USA, participation in a previous study with the research team, ECOG 3 questionnaire score > 3, pregnant | After ASCT | , home-based: T: Online Hatha yoga program I: NR L: Min. 60 min/week D: 12 weeks | Less | T: Online cancer health education podcasts L: 60 min/week D: 12 weeks |
| Furzer 2016 Australia [ ] | NHL, HL, MM | RCT | 37 (18/19) (NR) | Mean 48.9 (22–68) IG: 48.2 (22–64) CG: 49.6 (25–68) | Hematologist did not approve exercise due to identified risks | After chemotherapy or radiation or HSCT | , in local gyms and clinics: T: Aerobic (individual) and resistance training (machines and dumbbells) I: Cardio: 50–85% of HRmax, RPE of 10–16. Resistance: Initial 3 sets of 10–15 rep at 50% of 1 RM to 2–3 sets of 6–8 rep at 80% of 1 RM L: Max. 30 min, 3x/week D: 12 weeks | Moderate | T: Diary and general healthy lifestyle advice |
| Gallardo-Rodriquez 2023 Mexico [ ] | ALL | RCT Pilot 3-arm | 33 (11/11/11) (66.7) | Mean 23.7 (18–45) CEG: 20.5 (18–36) REG: 22.5 (18–36) CG: 28.0 (18–45) | Neutropenia, infections, bleeding at admission, were nonmotile or unable to carry out exercise; with a CNS disease preventing movement, alterations of heart function, with bone marrow or CNS relapse, with a referral from another hospital | During chemotherapy treatment | , hospital- and home-based: T: Cross-training or resistance (weights) exercises I: RPE of 3–6 (50–75% of HRR), 3–5 sets of 8–15 reps L: 30–50 min, 3–5x/week D: During inpatient period | Moderate | T: Mobilization I: Low L: 30 min, daily |
| Hacker 2017 USA [ ] | ALL, AML, CLL, CML, HL, NHL, MM, MDS | RCT | 67 (33/34) (38.8) | Mean 53.3 IG: 51.9 CG: 54.6 | Significant comorbidity, like impending pathological fracture, making exercise potentially unsafe | During and after ASCT or allo-HSCT | Supervised, hospital-based: T: Progressive resistance training (elastic resistance bands and body weights) I: Moderate intensity, Borg scale 13 L: 2–3x/week, D: During inpatient period Unsupervised, home-based: T: Progressive resistance training (elastic resistance bands and body weights) I: Moderate intensity, Borg scale 13 L: 2–3x/week D: 6 weeks after discharge | Moderate | T: UC, Attention control with health education |
| Hacker 2022 USA [ ] | MM | RCT Pilot | 32 (17/15) (34.4) | Mean 62.78 IG: 62.21 CG: 63.44 | NR | After ASCT and after discharge | Supervised, hospital-based: T: Weekly goal setting, daily step tracking, and individualized coaching I: NR L: Daily Unsupervised, home-based: T: Free-living PA, step trackers I: NR L: Daily D: 6 weeks | Moderate | T: UC, Recommendations regarding rest, PA, and exercise |
| Hathiramani 2020 UK [ ] | Lymph | RCT | 46 (23/23) (63) | Mean 61 IG: 61.5 CG: 60.4 | Active disease, unstable angina or unexplained electrocardiogram, poor PS (ECOG 3 or more), pregnancy, difficulty breathing at rest, persistent cough, fever or illness, or any cognitive impairment limiting the ability to give informed consent or complete questionnaires | During and after chemotherapy | , home-based: T: Individual elements of aerobic (walking), resistance training (resistance bands, body weight), core stability and stretches I: Aerobic: Moderate intensity Resistance: ACSM guidelines with 3 sets for 8–12 rep L: 50 min, 3x/week D: 12 weeks | Moderate | T: Bed or chair-based program, mindfulness-based. CD audio guidance to relaxation techniques: mindfulness meditation, breathing exercises, guided visualization and progressive muscle relaxation. I: No advice to exercise outside of normal habits, nor asked to avoid activity L: 50 min, 3x/week |
| Huberty 2019 USA [ ] | MPN: Polycythaemia Vera, Essential, Thrombocythemia, Myelofibrosis | RCT Pilot | 62 (34/28) (93.7) | Mean 56.9 IG: 58.3 CG: 55.0 | Reported performing tai chi, qi gong, or yoga for ≥60 min/week, reported engaging in ≥150 min/week of PA, utilized the study’s online yoga site: Udaya.com, (accessed on 21 August 2024) syncope in the last two months, recurrent falls: ≥2 in past two months, score of ≥15 on the PHQ-9, score of >3 on the ECOG-3, pregnant, residency outside USA | During or after chemotherapy | , home-based: T: Online homebased Hatha/Vinyasa yoga I: NR L: 5–30 min, 60 min/week D: 12 weeks | Less | T: UC, Maintain usual activity |
| Hung 2014 Australia [ ] | Lymph, ML | RCT Pilot | 37 (18/19) (46) | Mean IG: 57.5 CG: 59.9 | Undergoing allo-HSCT, deemed unsuitable for study participation by physicians | After ASCT | , home-based: T: Individual telephone-delivered nutrition and exercise counselling, unsupervised aerobic (walking or cycling) and resistance (sit-to-stand or free weight) I: Recommendations based on ACSM guidelines for cancer survivors L: Various length, 3–7x/week D: 12 weeks | Moderate | T: UC |
| Jacobsen 2014 USA [ ] | ALL, CML, CLL, MDS, MM, Lymph | RCT 4-arm | 711 (180/178/178/175) (43) | Median IG E: 58 (20–76) IG SM: 58 (20–75) IG E/SM: 57 (18–75) CG: 55 (19–76) >65, n = 154 (21.6%) | Orthopaedic, neurological, or other problems that prevented safe ambulation or protocol adherence, participation in another clinical trial with QoL or functional status as a primary endpoint, planned anticancer therapies other than tyrosine kinase inhibitor or rituximab within 100 days after HSCT, planned donor lymphocyte infusion within 100 days after HSCT, planned tandem transplantation | Before, during and after allo-HSCT or ASCT | , home-based: T: Self-directed exercise program, a DVD reinforcing the program, tracking of participation in exercise and/or stress management. Exercise component: Calculation of target HR and pedometer. The stress management component also included provision of a relaxation CD I: 50–75% of estimated HRR L: 20–30 min, 3–5x/week D: 180 dayS | Moderate | T: DVD with general instruction about HSCT L: 45 min |
| Jarden 2009 Denmark [ ] | CML, AML, ALL, AA, MDS, WM, PNH, MF | RCT | 42 (21/21) (38.1) | Mean 39.2 (18–60) IG: 40.9 (18–60) CG: 37.4 (18–55) Median 40.5 IG: 45.0 CG: 38.0 | Prior HSCT, recent cardiovascular, or pulmonary disease, abnormal EKG, psychiatric disorder, and motor, musculoskeletal or neurological dysfunction requiring walking aids and bony metastasis. Prior to testing: Signs of infection, anaemia, neutropenia, or thrombocytopenia, disqualified or testing postponed | During allo-HSCT | , hospital-based: T: Multimodal program of aerobic (ergometer), resistance (machines and weights) and active exercises, progressive relaxation, and psychoeducation I: Aerobic: Low to moderate, 50–75% HR max. RPE: 10–13. Dynamic and stretching 1–2 sets, 10–12 reps. Static: 1 set, hold for 15–30 s. Resistance: Low to moderate, 1–2 sets of 10–12 reps. Progressive relaxation: low L: 60–70 min, 3–5x/week D: 4–6 weeks | Moderate | T: UC, Conventional treatment and care, standard care for PA, PT is individualized, not providing a stationary cycle unless requested L: PT < 1½ hour/week, after allogeneic HSCT (day +1) |
| Jarden 2016 Denmark [ ] Jarden 2021 Denmark [ ] | Acute Leuk, AML de novo, AML following MDS, APL, ALL | RCT | 70 (34/36) (41.4) | Mean 53.1 (19.8–73.7) IG: 51.1 (19.8–70.0) CG: 55.0 (20.3–73.7) | Severe or unstable psychological, cardio-respiratory, neurological, or musculoskeletal disease, secondary active malignancy, abnormal EKG | During chemotherapy | , hospital-based: T: Multimodal intervention of aerobic (ergometer), strength (weights) and relaxation exercise, nutrition support, pedometer, and health counselling I: Aerobic: 75–80% of HRmax. Dynamic resistance: Moderate to hard, 2 sets, 12 reps L: 60 min, 3x/week D: 12 weeks | Extensive | T: UC |
| Kim 2005 South Korea [ ] | AML, ALL, SAA | RCT | 35 (18/17) (51.4) | Mean IG: 32.9 CG: 34.3 (20–48) | Medicated for anxiety or depression | After allo-HSCT | , hospital-based: T: Individual physical exercises combined with relaxation breathing I: NR L: 30 min/daily D: 6 weeks | Less | T: UC, Routine care |
| Knols 2011 Switzerland [ ] | AML, CLL, ALL, HL, NHL, MM, Osteo-myelofibrosis, Leuk, Amyloidosis, Testicular C. | RCT | 131 64/67 (41.2) | Mean 46.7 IG: 46.6 (18–75) CG: 46.6 (20–67) | GvHD except for grade I not requiring treatment, painful joints, unstable osteolysis, chronic pain, lesions of the central or peripheral nervous system, uncontrolled cardiovascular disease, thyroid disease, or diabetes | After allo-HSCT or ASCT | , physiotherapy practice or fitness centre: T: Individual, physical exercises with both endurance aerobic (ergometer or walking tread mill) and resistance strength (machines and dumbbells) exercises I: Individual HR (from 50–60%, increasing to 70–80% of estimated HR max) L: 30 min, 2x/week D: 12 weeks | Moderate | T: UC |
| Kobayashi 2020 Japan [ ] | AML, DLBCL, ALL | RCT Crossover | 33 (13/20) (18.2) | Mean Wii PT/Therapist PT: 44.9 Therapist PT/Wii PT: 44.6 | Grade 2 or worse CTC for Adverse Events version 4.0 | During chemotherapy | , hospital-based: T: Individual aerobic and resistance exercises using the Wii Fit balance board I: NR L: 30 min, 5x/week D: 1 week (and then crossover) | Less | T: Individual aerobic and resistance exercises. I: Aerobic: 40–60%. Resistance: Borg 11–13 L: 30 min, 5x/week D: 1 week and then crossover |
| Koutoukidis 2020 UK [ ] | MM, Myeloma IgG, Myeloma IgA, Myeloma Light chain, non-sec/oligo-sec. | RCT | 131 (89/42) (45) | Median IG: 64 (35–86) CG: 63 (40–80) | Spinal instability. Recent spinal or other surgery for pathological fractures within 4 weeks. Abnormal EKG with unexplained clinical indication after cardiological work-up. At risk of pathological fracture based on Mirel’s score. Currently enrolled in research exercise study. Unstable angina. Musculoskeletal mobility limitations. Cognitive impairment hindering completion of questionnaire | After auto-HSCT, radiotherapy or chemotherapy | Supervised, hospital-based: T: Individual aerobic (treadmill walking, ergometer, cross-trainer or stepping) and resistance (weightlifting, body weight or resistance bands) training, exercise diaries, goal setting with physiotherapist I: Aerobic: 50–75% of predicted HR max-Resistance: 10 RM L: 1x/week D: 6 months Unsupervised, home-based: T: Individual aerobic training and resistance training, exercise diaries, goal setting with PT I: Aerobic: 50–75% of predicted HR max. Resistance: 10 RM L: Max 30 min, 2–3x/week D: 6 months | Moderate | T: UC |
| McCourt 2023 UK [ ] | MM | RCT Pilot | 50 (23/27) (38) | Mean 60.4 (37–72) IG: 59.3 (37–72) CG: 61.3 (40–72) | Declined or not suitable for auto-HSCT or too close to transplantation, restricted mobility, non-English language | Before, during and after ASCT | Supervised, hospital-based: T: Aerobic (treadmill walking or ergometer) and resistance (machines and resistance bands) exercise and behaviour change support I: Aerobic: 60–80% of HRR. Resistance: 10 RM and individually tailored to progress and/or adapt to bone disease. L: 1x/week Unsupervised, home-based: T: Aerobic (walking) and resistance (resistance bands) exercise and behaviour change support, virtual I: Aerobic: 60–80% of HRR. Resistance: 10 RM and individually tailored to progress and/or adapt to bone disease L: Aerobic exercise (Phase 1 and 3): 15–40 min, 3x/week. Resistance exercise (Phase 1 and 3): 3x/week. During phase 2 (transplant admission) | Extensive | T: UC |
| Mello 2003 Brazil [ ] | CML, AML, SAA, NHL, MDS | RCT | 18 (9/9) (55.6) | Mean IG: 27.9 (18–39) CG: 30.2 (18–44) | NR | During and after allo-HSCT | , hospital-based: T: Individualized exercise program with active exercise, muscle stretching and treadmill walking I: Progressing, no higher than 70% of HR max L: 40 min, 5x/week D: 6 weeks | Moderate | NR |
| Oechsle 2014 Germany [ ] | AML, NHL, MM, Germ cell | RCT Pilot | 58 (29/29) (29.2) | Mean IG: 51.7 CG: 52.9 | Symptomatic cardiovascular diseases, tumor infiltration of the skeletal system with risk of pathologic fractures or compression of spinal cord, epilepsy, rheumatologic diseases, BMI < 18, BMI > 30, insufficient cognitive function, inadequate knowledge of German language for questionnaire analysis | During chemotherapy | , hospital-based: T: Aerobic (ergometer) and strength (body weights and resistance bands) training I: Ergometer individually adjusted Strength training: Up to 20 min at 40–60% of estimated 1 RM, sets of 16–25 repetitions L: 30–40 min, 5x/week D: Median: 21 days | Moderate | T: UC, Standard PT |
| Pahl 2018 Germany [ ] | Leuk, AML, ALL, APL, NHL, HL, T-cell lymph, WM, MM, PMF | RCT Pilot | 17 (10/7) (30) | Median 55 (47–63) IG: 47 (19–62) CG: 56 (32–63) | Unstable bone metastasis, knee or hip endoprosthesis, epilepsy, pacemaker, severe cardiovascular disease and threshold blood-count values below safety criteria, stents, or former joint injuries | During chemotherapy | , hospital-based: T: Whole body vibration (Galileo Sport vibration platform), including three sets of two to four different exercises (body weight) I: Borg scale 14–16 L: 20 min, 3x/week D: Median: 27 days | Moderate | T: Aerobic exercise; ergometer I: Borg scale 14–16 L: 20 min. |
| Pahl 2020 Germany [ ] | AML, ALL, CLL, CMML, MDS, Lymph, MM, MF, Septic granulomatosis Immuno-deficiency, SAA | RCT | 44 (18/26) (31.8) | Median IG: 55 (50–63) CG: 56 (32–63) | Unstable bone metastasis, endoprosthesis of knee or hip, epilepsy, pacemaker, and severe cardiovascular disease | During allo-HSCT | , hospital-based: T: Whole body vibration (Galileo Sport vibration platform) I: NR L: 20 min, 5x/week D: 35–44 days | Moderate | T: Mobilization and stretching L: 5x/week |
| Persoon 2017 Netherlands [ ] | MM, (N)HL, Lymph | RCT | 109 (54/55) (36.7) | Median 55 (19–67) IG: 53.5 (20–67) CG: 56 (19–67) | NR | After ASCT | , at local physiotherapy practices: T: Aerobic interval (cycling) and resistance (machines) training, counselling sessions (5x) I: Resistance: High intensity. Week 1–12 2 × 10 rep at 65–80% of 1 RM, week 12–18 2 × 20 rep at 35–40% of 1 RM L: 60 min, 1–2x/week D: 18 weeks | Extensive | T: UC, Not encouraged to exercise, participate in sports, PT, or rehabilitation programs |
| Potiaumpai 2021 USA [ ] | AML, ALL, CML, MDS, MM, other Lymph | RCT | 35 (19/16) (45.7) | Mean 58.8 IG: 59.3 CG: 58.2 | Dementia, altered mental status, severe psychiatric conditions, pre-existing comorbid conditions that would contraindicate exercise testing, concurrent non-transplant-related chemotherapy, or radiation | Before and after allo-HSCT or ASCT | , hospital-based: T: Multidirectional drills and walking program I: Exertion level of moderate intensity during the multidirectional drills and a high intensity during the walking portion L: 5–30 min, 3x/weeks D: Varied | Moderate | T: UC |
| Safran 2022 Turkey [ ] | AML, B-cell ALL, T-cell ALL, MDS, NHL, MF | RCT | 43 (21/22) (51.6) | Mean IG: 38 (23–63) CG: 40.5 (24–58) | <18 years, ECOG > 3, comorbidities causing fatigue (e.g., multiple sclerosis, Parkinson’s disease, heart failure), rapid deterioration of general condition (sudden uncontrolled weight loss, confused consciousness, high CRP values), brain metastases or metastases to the femur, DVT within last 6 months, neuropathy, and rejecting NMES intervention or exercise therapy | During chemotherapy, after allo-HSCT | , hospital-based: T: Resistance exercise (body weights and resistance bands) combined with neuromuscular electrical stimulation I: Borg scale: Initial recommended RPE is 12–13 and is increased to about 15–16. The intensity was adjusted to a target score of 12–14 (moderate level) using the RPE scale. Intensity (~RPE 15–16) and resistance were gradually increased L: 60–90 min, 2–3x/week D: 4 weeks | Moderate | T: Resistance exercise L: 40–60 min, 2–3 days/week |
| Schumacher 2018 Germany [ ] | MM, AML/MDS, NHL Teratoma, CML, CLL | RCT feasibility | 42 (19/23) (40.5) | Median IG: 56.0 (21–65) CG: 56.5 (21–65) | Lack of compliance. Intercurrent diseases, like pulmonary and cardiac insufficiency or uncontrolled infections | During and after allo-HSCT or ASCT | , hospital-based: T: Exergaming on Nintendo Wii for exercising ping pong, tennis, boxing, frisbee, or aerobics and balance I: NR L: 30 min, 5x/week D: During and 30 days post HSCT | Moderate | T: PT program, eccentric and concentric movements, from supine to standing, walking, stepping or treadmill walking, stretching, strength exercise i.e., elastic bands and body weight |
| Shelton 2009 USA [ ] | Lymph, Leuk | RCT | 53 (26/27) (37.7) | Mean IG: 43.7 (22–68) CG: 48.9 (29–70) | <18 years, psychiatric disorder, significant cardiovascular disease, paraplegic or hemiplegic, unable to speak or understand English | After allo-HSCT | , hospital-based: T: Aerobic (treadmill and ergometer) and resistance (weights and machines) exercises I: Aerobic: 60–75% of age-predicted HR max. Strength: 1–3 sets of 10 reps L: 20–30 min aerobic, resistance individual, 3x/week D: 4 weeks | Moderate | T: multidisciplinary, inpatient, educational session incl. focus on staying active, information to exercise safely |
| Streckmann 2014 Germany [ ] | HL, B-NHL, T-NHL, MM | RCT | 56 (28/28) (25) | Mean IG: 44 (20–67) CG: 48 (19–73) | Unstable osteolysis, severe acute infections, severe cardiac and pulmonary impairments, restrictions for PA | During chemotherapy | , hospital-based: T: Aerobic (treadmill and ergometer), sensorimotor and strength (resistance bands) training I: Initial 60–70% HR max. At the end of session 70–80%. Sensorimotor training: Progressively increasing task difficulty. Strength training: 1 min at max force L: 60 min, 2x/week D: 36 weeks | Extensive | T: UC, Standard clinical care, incl. PT |
| Vallerand 2018 Canada [ ] | Leuk., HL, NHL | RCT | 51 (26/25) (60.8) | Mean 52.6 <60: n = 33 >60: n = 18 | Chronic medical condition precluding from aerobic exercise, plan of being away from home > 2 weeks, baseline exercise levels of ≥240 min. weekly | During or after chemotherapy, radiation, HSCT | , home-based: T: Tele counselling with PA guidance with a goal of increasing aerobic exercise (walking, group fitness) levels by at least 60 min/week up to 300 min/week of moderate-vigorous aerobic exercise I: Aerobic exercise: Moderate-vigorous L: Tele-health calls: Mean: 17 min, 1x/week. Aerobic: 60–300 min/week. D: 12 weeks | Moderate | T: UC, PT guidelines, goal setting of increasing aerobic exercise levels I: Aerobic exercise: moderate-vigorous L: 60–300 min/week |
| Waked 2019 Egypt [ ] | ALL | RCT | 54 (27/27) (34) | Mean IG: 33.4 CG: 32.4 | Antecedent neurological, developmental, or genetic disorder. Relapsed or secondary ALL. Received testicular, mediastinal, or craniospinal irradiation. Growth hormone insufficiency, hormone therapy. Medications that interfere with lipid metabolism. Diseases affecting cholesterol metabolism such as diabetes mellitus, thyroid dysfunction, or nephrotic syndrome | After treatment | , hospital-based: T: Aerobic training (ergometer) I: 60% of predictive age HR max L: 30–40 min, 3x/week D: 12 weeks | Moderate | T: UC, Normal daily activities |
| Wehrle 2019 Germany [ ] | AML, ALL | RCT Pilot 3-arm | 29 (9/10/10) (41) | Median EG: 47.7 (21.9–63.4) RG: 47.4 (41.2–62.2) CG: 50.6 (35.0–58.1) | Karnofsky score < 60, uncontrolled hypertension, cardiac illness (NYHA III-IV), instable bone metastases, lack of informed consent after screening | During chemotherapy | , hospital-based: T: Either aerobic (ergometer or treadmill) or resistance (body weight) training I: Endurance: 60–70% of HRmax, RPE of 12–14 Resistance: RPE 12–14 L: 30–45 min, 3x/week D: 5 weeks (median) | Moderate | T: Mobilization and stretching program, I: low intensity |
| Wiskemann 2011 Germany [ ] Wiskemann 2014 Germany [ ] | AML, ALL, CML, CLL, MDS, Sec. AML, MPS, MM, other Lymph, AA | RCT | 105 (52/53) (32.4) | Mean 48.8 (18–71) IG: 47.6 (18–70) CG: 50 (20–71) | NR | Before, during and after allo-HSCT | , hospital-based and home-based: T: Aerobic (ergometer/treadmill or walking) and resistance (resistance bands) exercises I: Tailored intensity. Endurance: Borg scale: 12–14. Resistance: Borg scale: 14–16 w/8–20 rep × 2–3 sets L: 20–40 min, 2–5x/week. Endurance: 3–5x/week. Resistance: 2x/week | Moderate | T/I: Recommend moderate PA, received step counters L: Same frequency of social contact as in IG. PT up to 3x/week |
| Wood 2020 USA [ ] | AML, MDS, ALL, CML, HL, MM, MF, AA, MCL, HLH | RCT Pilot | 34 (17/17) (43) | Median 52 (28–73) | Transplant ineligibility, uncertain transplant candidacy, comorbid illness that would preclude maximal effort during exercise testing or participation in regular exercise determined by the treating physician or study exercise physiologist | Before allo-HSCT | , home-based: T: Aerobic exercise (walking, jogging, running, cycling, cross trainer or stair climbing) I: 80% HR max. From week 2 Interval, 2 min 80%, 3 min low recovery L: 30 min, 3–4x/week D: Mean: 11 weeks | Moderate | T: Fitbit Surge, no further instructions and information |
| Yeh 2016 Taiwan [ ] | NHL | RCT | 108 (54/54) (44.1) | Mean 59.8 (23–90) | Major medical disease, as uncontrolled arrhythmia, hypertension, unstable angina, severe respiratory disease, acute infection, multiple myeloma, bone metastasis, psychiatric disorders. Medical contraindications for exercise, e.g., orthopaedic problems and neurologic or musculoskeletal disturbances, or already practicing qigong or other exercise training programs | During chemotherapy | , home-based: T: Chan-Chuang qigong exercise, guidance booklet and weekly phone call I: NR L: 20–60 min, 2–3x/day (max. 5 times). D: 3 weeks | Less | T: UC |
| Outcomes | SMD (95% CI) | Participants Completed Outcome Measures, n Studies, (n) | Quality of Evidence GRADE | Comments |
|---|---|---|---|---|
| Physical function * 12MWT; 2MSC; 2MWT; 6MWT; Accelerometer; KPS; SWT; TUG | 0.29 (0.12–0.45) | 1219 (25) | ⨁◯◯◯ Very low | Downgraded, due to RoB (majority of trials), Inconsistency (moderate heterogeneity: 48.17%), and risk of Publication bias (Egger’s test p = 0.0516) |
| Aerobic capacity Aerobic Power Index; Modified Balke; Modified endurance test; Power Max, Timed Stair Climb; VO2 Max; VO2 Max Relative; VO2 Peak; VO2 Peak modified | 0.53 (0.27–0.79) | 853 (17) | ⨁⨁◯◯ Low | Downgraded, due to Inconsistency (substantial heterogeneity: 69.21%) and risk of Publication bias (Egger’s test p = 0.0443) |
| Muscle strength GRIP; Max test; Isometric Knee Extension test; STS | 0.47 (0.17–0.78) | 1091 (25) | ⨁⨁⨁◯ Moderate | Downgraded, due to Inconsistency (substantial/considerable heterogeneity: 82.59%) |
| Body composition BMI; BodPod; DEXA; SECA bioimpedance, Tanita Bioelectrical impedance | 0.20 (0.03–0.37) | 654 (12) | ⨁⨁⨁⨁ High | No change |
| Physical activity GLTEQ; IPAQ; PASE | 0.32 (−0.00–0.65) | 358 (5) | ⨁◯◯◯ Very low | Downgraded, due to RoB (majority of trials), Inconsistency (moderate heterogeneity: 56.97%), Imprecision (95% CI does not exclude 0), and risk of Publication bias (Egger’s test p = 0.0132) |
| QoL Global * CMSAS; EORTC QLQ-C30; FACT; FACT-An; FACT-BMT; FACT-Leu; GLQOL; POMS; PROMIS | 0.34 (0.04–0.64) | 1447 (29) | ⨁⨁◯◯ Low | Downgraded, due to RoB (majority of trials) and Inconsistency (substantial/considerable heterogeneity: 87.39%) |
| QoL Emotional CMSAS; EORTC QLQ-C30; FACT-General, FACT-Leu; Happiness Scale; NCCN Distress Thermometer; POMS; PROMIS; SF-12; SF-36 | 0.33 (0.05–0.60) | 1764 (28) | ⨁⨁◯◯ Low | Downgraded, due to Inconsistency (substantial/considerable heterogeneity: 86.93%) |
| QoL Functional EORTC QLQ-C30; FACT; FACT-An; FACT-BMT; FACT-Leu; FACT-TOI | 0.33 (0.09–0.57) | 455 (10) | ⨁⨁◯◯ Low | Downgraded, due to RoB (majority of trials), and Inconsistency (moderate heterogeneity: 37.54%) |
| QoL Physical CMSAS; EORTC QLQ-C30; FACT-An; FACT-BMT; FACT-Leu; FACT-TOI; PROMIS; SF-12; SF-36 | 0.32 (0.03–0.60) | 1731 (28) | ⨁⨁◯◯ Low | Downgraded, due to RoB (majority of trials) and Inconsistency (substantial/considerable heterogeneity: 87.72%) |
| Anxiety HADS; POMS; PROMIS; STAI | 0.21 (0.13–0.55) | 917 (17) | ⨁◯◯◯ Very low | Downgraded, due to RoB (majority of trials), Inconsistency (Substantial/considerable heterogeneity: 84.23%) and Imprecision (95% CI does not exclude 0) |
| Depression CES-D; HADS; POMS; PROMIS | 0.37 (0.09–0.64) | 919 (17) | ⨁◯◯◯ Very low | Downgraded, due to RoB (majority of trials), Inconsistency (substantial/considerable heterogeneity: 76.33%), and risk of Publication bias (Egger’s test p = 0.0184) |
| Fatigue BFI; EORTC QLQ-C30; FACT-An; FACIT-F; FACT-F; MFI; MPN-SAF; 11-point rating scale; POMS; PROMIS; SCFS | 0.44 (0.16–0.71) | 1860 (31) | ⨁⨁◯◯ Low | Downgraded, due to RoB (majority of trials) and Inconsistency (substantial/considerable heterogeneity: 87.89%) |
| Pain EORTC QLQ-C30; PROMIS; SF-36 | 0.43 (0.13–0.73) | 811 (14) | ⨁⨁◯◯ Low | Downgraded, due to RoB (majority of trials) and Inconsistency (substantial/considerable heterogeneity: 77.82%) |
| Recruitment IG and CG | Retention IG and CG | Participation | Adverse Events | |||
|---|---|---|---|---|---|---|
| IG | IG | |||||
| Author Year/Country | Sample Size Estimated, n | Eligibility Assessed, n | Included, n | Completed Post-Test, n | Adherence to Exercise (%) | AE Type, n |
| Accogli [ ] 2022, Italy | 40 | 193 | 46 | 42 | 90 | No AE |
| Alibhai [ ] 2014, Canada | 40 | 232 | 38 | 36 | 28 | NR |
| Alibhai [ ] 2015, Canada | 72 | 264 | 81 | 70 | 54 | AE: 4 grade II musculoskeletal events |
| Baumann [ ] 2010, Germany | 60 | NR | 64 | 49 | NR | NR |
| Baumann [ ] 2011, Germany | 45 | NR | 47 | 33 | NR | No AE |
| Bayram [ ] 2024, Turkey | 28 | 39 | 30 | 26 | 20 (IMT) | No AE |
| Bird [ ] 2010, UK | 132 | 158 | 58 | 46 | NR | No AE |
| Bryant [ ] 2018, USA | 30 | 82 | 18 | 17 | 80 | No AE |
| Chang [ ] 2008, Taiwan | NR | 28 | 24 | 22 | NR | No AE |
| Chen [ ] 2021, China | 30 | 46 | 30 | 29 | 98 | NR |
| Chow [ ] 2020, USA | 41 | 420 | 41 | 37 | 75 | NR |
| Chuang [ ] 2017, Taiwan | 100 | 105 | 100 | 96 | 96 | No AE |
| Cohen [ ] 2004, USA | 38 | NR | 39 | 30 | 32 | NR |
| Coleman [ ] 2003, USA | NR | NR | 24 | 13 | NR | No AE |
| Coleman [ ] 2012, USA | 200 | NR | 187 | 166 | NR | NR |
| Courneya [ ] 2009, Canada | 120 | 1306 | 122 | 117 | 92 | No SAE. AE: 3 back, hip, and knee pain |
| Defor [ ] 2007, USA | NR | 122 | 100 | 85 | 24 | NR |
| Eckert [ ] 2022, USA | NR | 326 | 72 | 43 | NR | No AE |
| Furzer [ ] 2016, Australia | NR | 89 | 44 | 37 | 91 | No SAE. AE: 2 minor exercise modifications due to pre-existing knee and back injuries |
| Gallardo-Rodriquez [ ] 2023, Mexico | 114 | 50 | 33 | 18 | NR | No (significant) AE |
| Hacker [ ] 2017, USA | NR | 118 | 67 | 67 | 83 | NR |
| Hacker [ ] 2022, USA | NR | 45 | 32 | 30 | NR | NR |
| Hathiramani [ ] 2020, UK | 46 | 62 | 46 | 38 | NR | No AE |
| Huberty [ ] 2019, USA | NR | 260 | 62 | 48 | 15 | No AE |
| Hung [ ] 2014, Australia | NR | 55 | 37 | 33 | NR | No AE |
| Jacobsen [ ] 2014, USA | 700 | NR | 711 | 560 | NR | No AE |
| Jarden [ ] 2009, Denmark | 40 | 82 | 42 | 34 | NR | No AE |
| Jarden [ ] 2016, Denmark Jarden [ ] 2021, Denmark | 70 | 170 | 70 | 62 | 71 | No SAE. AE: 8: sport-related (n = 5), cardioresp (n = 5), dizziness (n = 3), gastrointestinal (n = 3), pain/discomfort (n = 2) and bruising (n = 1) |
| Kim [ ] 2005, S. Korea | 42 | NR | 42 | 35 | NR | NR |
| Knols [ ] 2011, Switzerland | 128 | 310 | 131 | 114 | 85 | No AE |
| Kobayashi [ ] 2020, Japan | 32 | 33 | 33 | 22 | 67 | No AE |
| Koutoukidis [ ] 2020, UK | 140 | 313 | 131 | 99 | 75 | No AE |
| McCourt [ ] 2023, UK | NR | 123 | 50 | 33 | NR | No SAE. AE: 1 mild episode of dizziness |
| Mello [ ] 2003, Brazil | NR | 32 | 18 | 18 | NR | NR |
| Oechsle [ ] 2014, Germany | 48 | NR | 58 | 48 | NR | No AE |
| Pahl [ ] 2018, Germany | NR | 121 | 20 | 11 | 62 | No AE |
| Pahl [ ] 2020, Germany | NR | 112 | 71 | 44 | 59 | No SAE. AE: 2 sessions stopped prematurely due to knee pain and discomfort |
| Persoon [ ] 2017, The Netherlands | 120 | 469 | 109 | 97 | 86 | AE: 1 strained calf muscle |
| Potiaumpai [ ] 2021, USA | NR | 57 | 36 | 32 | 79 | NR |
| Safran [ ] 2022, Turkey | 32 | 77 | 43 | 31 | NR | No AE |
| Schumacher [ ] 2018, Germany | NR | 49 | 42 | 31 | NR | No AE |
| Shelton [ ] 2009, USA | 164 | 250 | 61 | 53 | 75 | NR |
| Streckmann [ ] 2014, Germany | 184 | 186 | 61 | 51 | 65 | No AE |
| Vallerand [ ] 2018, Canada | 50 | 407 | 51 | 51 | 93 | No AE |
| Waked [ ] 2019, Egypt | 54 | 60 | 54 | 50 | NR | NR |
| Wehrle [ ] 2019, Germany | 36 | 39 | 29 | 22 | 68 | No AE |
| Wiskemann [ ] 2011, Germany Wiskemann [ ] 2014, Germany | NR | 141 | 105 | 80 | 87 | NR |
| Wood [ ] 2020, USA | 60 | 113 | 34 | 16 | NR | NR |
| Yeh [ ] 2016, Taiwan | 64 | 118 | 108 | 102 | 100 | No AE |
| Total | NR (n = 16) | 7262 NR (n = 8) | 3552 | 2924 (82.3%) | Mean: 70% (15–100) NR (n = 21) | No AE (n = 26) AE (n = 7) SAE (n = 1) NR (n = 15) |
| Trial Identifier Design | Investigator Country | Title | Diagnosis | Sample Size, n | Age | Intervention Type and Duration | Treatment Trajectory | Primary Outcome | Study Status |
|---|---|---|---|---|---|---|---|---|---|
| NCT05642884 RCT | Smith Giri USA | Prehabilitation Feasibility Among Older Adults Undergoing Transplantation | MM | 30 | >60 years | Home-based prehabilitation multimodal exercise program delivered using a telehealth format 8 weeks | Before ASCT | Feasibility | Recruiting 2023-07-10 Estimated completion 2025-12-31 |
| NCT04898790 RCT | Thuy Koll USA | Improving Cognitive Function in Older Adults Undergoing Stem Cell Transplant (PROACTIVE) | Leukemia Lymphoma MM MDS MPN | 88 | >60 years | Partially supervised PA in the Community Health Activities Model Program for Seniors 12 weeks | Undergoing HSCT | Change in executive function and working memory | Recruiting 2021-11-18 Estimated completion 2025-04 |
| NCT04670029 RCT | Magali Bavaloine France | Impact of an APA Program on EFS in Patients with Diffuse Large-cell B Lymphoma Treated in 1st Line (PHARAOM) | Diffuse Large B Cell Lymphoma | 186 | >65 years | Partially supervised adapted physical activity with aerobic and anaerobic sessions on site and at home | During treatment | To detect an absolute difference of 15% in event-free survival between groups | Recruiting 2021-09-08 Estimated completion 2029-02 |
| NCT04057443 RCT | Maite Antonio Spain | Nutritional and Physical Exercise Intervention in Older Patients with Malignant Hemopathies | MDS LPS MM | 80 | >70 years | Nutritional support according to nutritional body composition parameters (Nutritional assessment and sarcopenia evaluation). Diet counselling, oral supplemented nutrition, enteral or parenteral nutrition. Exercise program with a mixed structure, designed individually with group sessions. 24 weeks, 3 days a week | During treatment | Adherence to oncological treatment from baseline to post treatment or 6 months. Difference between dose administered and prescribed. | Unknown status Start 2019-04-11 Estimated completion 2023-06-01 |
| The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
Share and Cite
Jarden, M.; Tscherning Lindholm, S.; Kaldan, G.; Grønset, C.; Faebo Larsen, R.; Larsen, A.T.S.; Schaufuss Engedal, M.; Kramer Mikkelsen, M.; Nielsen, D.; Vinther, A.; et al. Limited Evidence for the Benefits of Exercise in Older Adults with Hematological Malignancies: A Systematic Review and Meta-Analysis. Cancers 2024 , 16 , 2962. https://doi.org/10.3390/cancers16172962
Jarden M, Tscherning Lindholm S, Kaldan G, Grønset C, Faebo Larsen R, Larsen ATS, Schaufuss Engedal M, Kramer Mikkelsen M, Nielsen D, Vinther A, et al. Limited Evidence for the Benefits of Exercise in Older Adults with Hematological Malignancies: A Systematic Review and Meta-Analysis. Cancers . 2024; 16(17):2962. https://doi.org/10.3390/cancers16172962
Jarden, Mary, Sofie Tscherning Lindholm, Gudrun Kaldan, Charlotte Grønset, Rikke Faebo Larsen, Anders Thyge Steen Larsen, Mette Schaufuss Engedal, Marta Kramer Mikkelsen, Dorte Nielsen, Anders Vinther, and et al. 2024. "Limited Evidence for the Benefits of Exercise in Older Adults with Hematological Malignancies: A Systematic Review and Meta-Analysis" Cancers 16, no. 17: 2962. https://doi.org/10.3390/cancers16172962
Article Metrics
Article access statistics, supplementary material.
ZIP-Document (ZIP, 12748 KiB)
Further Information
Mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals

IMAGES
VIDEO
COMMENTS
This article is a practical guide to conducting data analysis in general literature reviews. The general literature review is a synthesis and analysis of published research on a relevant clinical issue, and is a common format for academic theses at the bachelor's and master's levels in nursing, physiotherapy, occupational therapy, public health and other related fields.
Reviews of the professional literature have consistently found that many applications of EFA are marked by an injudicious choice of methods and incomplete reports. ... Gaskin C. J., Happell B. (2014). On exploratory factor analysis: A review of recent evidence, an assessment of current practice, and recommendations for future use. International ...
Exploratory research can help you narrow down your topic and formulate a clear hypothesis and problem statement, as well as giving you the "lay of the land" on your topic. Data collection using exploratory research is often divided into primary and secondary research methods, with data analysis following the same model. Primary research
9.3. Types of Review Articles and Brief Illustrations. EHealth researchers have at their disposal a number of approaches and methods for making sense out of existing literature, all with the purpose of casting current research findings into historical contexts or explaining contradictions that might exist among a set of primary research studies conducted on a particular topic.
Exploratory factor analysis (EFA) is a powerful statistical technique that enables researchers to use their judgement and interpretation to identify a set of latent factors that meaningfully and parsimoniously represent a set of indicators (Goretzko et al., 2021, Hair et al., 2019, Howard, 2016, Watkins, 2018).The technique estimates the number of latent factors underlying the indicators as ...
Manual exploratory literature reviews should be a thing of the past, as technology and development of machine learning methods have matured. The learning curve for using machine learning methods is rapidly declining, enabling new possibilities for all researchers. A framework is presented on how to use topic modelling on a large collection of papers for an exploratory literature review and how ...
2.7 Extraction and analysis of data. Data were extracted in the process of scoping literature reviews, including information with regards to formulating the problem, establishing and validating the review procedure, searching the literature, screening for inclusion, evaluating quality, extracting data, analyzing and synthesizing data, and reporting the findings (Xiao & Watson, 2019).
Exploratory Factor Analysis. Exploratory Factor Analysis (EFA) is widely used in medical education research in the early phases of instrument development, specifically for measures of latent variables that cannot be assessed directly. ... Typically, in EFA, the researcher, through a review of the literature and engagement with content experts ...
Different solutions have been recommended in the extant literature to deal with this weakness, such as the use of mixed methods (e.g., Opoku et al., 2016), the support of the chosen methodology through a detailed research protocol (e.g., Yin, 2003), or the support of a study through a systematic literature review (e.g., Tranfield et al., 2003 ...
4. Choosing between factor analysis and principal components analysis4.1. Review of literature. Factor analysis and PCA are separate data extraction procedures, each with their own purpose and model (Schmitt, 2011, Thomson, 1939, Widaman, 2007).Some authors have argued that the purpose of factor analysis is to explain the correlations between items in terms of one or more latent factors ...
As mentioned previously, there are a number of existing guidelines for literature reviews. Depending on the methodology needed to achieve the purpose of the review, all types can be helpful and appropriate to reach a specific goal (for examples, please see Table 1).These approaches can be qualitative, quantitative, or have a mixed design depending on the phase of the review.
What is a literature review? Definition: A literature review is a systematic examination and synthesis of existing scholarly research on a specific topic or subject. Purpose: It serves to provide a comprehensive overview of the current state of knowledge within a particular field. Analysis: Involves critically evaluating and summarizing key findings, methodologies, and debates found in ...
1.3.1.2 Empirical. An empirical literature review collects, creates, arranges, and analyzes numeric data reflecting the frequency of themes, topics, authors and/or methods found in existing literature. Empirical literature reviews present their summaries in quantifiable terms using descriptive and inferential statistics.
Qualitative, narrative synthesis. Thematic analysis, may include conceptual models. Rapid review. Assessment of what is already known about a policy or practice issue, by using systematic review methods to search and critically appraise existing research. Completeness of searching determined by time constraints.
Abstract. As the name suggest a good literature review is always comprehensive and contextualized with respect to the research. It provides the reader or the target audience with a base of the theory base along with a survey of published works that pertain to the investigation of the researcher and further an analysis of that particular work.
Exploratory Search. Once you have an initial research question, you can develop and refine your research question and eligibility criteria through exploratory searching.Exploratory searching is also called preliminary, initial, and naive or novice searching.Regardless of what you call it, it is simply a series of searches conducted prior to starting the review with the goal of producing a well ...
A systematic literature review of exploratory factor analyses in management. September 2023. Journal of Business Research 164 (1):113969. 164 (1):113969. DOI: 10.1016/j.jbusres.2023.113969 ...
LITERATURE REVIEW . Exploratory data analysis (EDA) is an important first step in the data analysis process that involves exploring and . ... Exploratory data analysis (EDA) is a well-established ...
We also conducted an exploratory study of over 2700 AI-enabled healthcare startups worldwide to supplement our literature review. The SLR reveals several gaps within the research scope and ...
Later, we present a systematic literature review of 50 state-of-the-art visual data analytics tools and their utility in six distinct steps of the Exploratory Data Analysis (EDA) process. We also investigate the extent to which these modern visual EDA tools address scalability, interpretability, and analytical expertise challenges of analyzing ...
DOI: 10.1016/j.techsoc.2023.102321 Corpus ID: 259347766; Artificial intelligence innovation in healthcare: Literature review, exploratory analysis, and future research @article{Zahlan2023ArtificialII, title={Artificial intelligence innovation in healthcare: Literature review, exploratory analysis, and future research}, author={Ahmed Zahlan and Ravi Ranjan and David Hayes}, journal={Technology ...
An exploratory analysis of participants in whom normoglycaemia was achieved in the SURPASS 1-4 studies has recently been reported, ... Access is provided after a proposal has been approved by an independent review committee identified for this purpose and after receipt of a signed data-sharing agreement. Data and documents, including the ...
Design, Setting, and Participants This was an exploratory analysis of the Pediatric Adenotonsillectomy Trial for Snoring (PATS) randomized clinical trial of adenotonsillectomy vs watchful waiting for mild oSDB (snoring with obstructive apnea-hypopnea index of <3 events/hour) that took place at 7 pediatric tertiary care centers across the US and ...
Background and Objectives: We investigated the effects of using a BiZact™ device for tonsillectomy on operating time, intraoperative blood loss, postoperative bleeding rate, and pain through a meta-analysis of the relevant literature. Materials and Methods: We reviewed studies retrieved from the databases of PubMed, SCOPUS, Google Scholar, Embase, Web of Science, and Cochrane up to March ...
Current approaches to gas path analysis are extended by incorporating EO data. The analytical approach is presented in combination with a literature review. The literature review covers the following topics: flight trajectory modeling, EO/environmental condition data, as well as engine performance, condition, and deterioration modeling.
Analysis Source. IMPACT Initiatives; Posted 29 Aug 2024 ... launched an in-depth literature review at the beginning of 2024 to understand what the emerging innovations and best practices in the ...
The second step of the review is illustrated in Fig. 2, where we performed a systematic process following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [29] to select research articles for inclusion in this SLR.In the first stage of our investigation, we looked through the keywords listed in Table 2.The search was conducted with the selected keywords ...
Older patients receiving antineoplastic treatment face challenges such as frailty and reduced physical capacity and function. This systematic review and meta-analysis aimed to evaluate the effects of exercise interventions on physical function outcomes, health-related quality of life (QoL), and symptom burden in older patients above 65 years with hematological malignancies undergoing ...
Abstract. This paper presents an end-to-end analysis of Fintech-driven sandboxes, with a particular focus on Latin America. Contrary to the procedural approach characterizing sandbox research, our analysis adopted the managerial perspective, and resulted in a theoretical and applicable framework.
We review the application and reporting of exploratory factor analysis (EFA) in management. First, we integrate recommendations from relevant reviews and simulation studies to provide modern guidelines regarding EFA for psychometric investigation, and we highlight severe concerns associated with EFA for Harman's one-factor test. Second, we conduct a systematic literature review including ...