Fact sheets
- Facts in pictures
- Publications
- Questions and answers
- Tools and toolkits
- Endometriosis
- Excessive heat
- Mental disorders
- Polycystic ovary syndrome
- All countries
- Eastern Mediterranean
- South-East Asia
- Western Pacific
- Data by country
- Country presence
- Country strengthening
- Country cooperation strategies
- News releases
Feature stories
- Press conferences
- Commentaries
- Photo library
- Afghanistan
- Cholera
- Coronavirus disease (COVID-19)
- Greater Horn of Africa
- Israel and occupied Palestinian territory
- Disease Outbreak News
- Situation reports
- Weekly Epidemiological Record
- Surveillance
- Health emergency appeal
- International Health Regulations
- Independent Oversight and Advisory Committee
- Classifications
- Data collections
- Global Health Observatory
- Global Health Estimates
- Mortality Database
- Sustainable Development Goals
- Health Inequality Monitor
- Global Progress
- World Health Statistics
- Partnerships
- Committees and advisory groups
- Collaborating centres
- Technical teams
- Organizational structure
- Initiatives
- General Programme of Work
- WHO Academy
- Investment in WHO
- WHO Foundation
- External audit
- Financial statements
- Internal audit and investigations
- Programme Budget
- Results reports
- Governing bodies
- World Health Assembly
- Executive Board
- Member States Portal
- Fact sheets /

Hypertension
- An estimated 1.28 billion adults aged 30–79 years worldwide have hypertension, most (two-thirds) living in low- and middle-income countries
- An estimated 46% of adults with hypertension are unaware that they have the condition.
- Less than half of adults (42%) with hypertension are diagnosed and treated.
- Approximately 1 in 5 adults (21%) with hypertension have it under control.
- Hypertension is a major cause of premature death worldwide.
- One of the global targets for noncommunicable diseases is to reduce the prevalence of hypertension by 33% between 2010 and 2030.
Hypertension (high blood pressure) is when the pressure in your blood vessels is too high (140/90 mmHg or higher). It is common but can be serious if not treated.
People with high blood pressure may not feel symptoms. The only way to know is to get your blood pressure checked.
Things that increase the risk of having high blood pressure include:
- older age
- being overweight or obese
- not being physically active
- high-salt diet
- drinking too much alcohol
Lifestyle changes like eating a healthier diet, quitting tobacco and being more active can help lower blood pressure. Some people may still need to take medicines.
Blood pressure is written as two numbers. The first (systolic) number represents the pressure in blood vessels when the heart contracts or beats. The second (diastolic) number represents the pressure in the vessels when the heart rests between beats. Hypertension is diagnosed if, when it is measured on two different days, the systolic blood pressure readings on both days is ≥140 mmHg and/or the diastolic blood pressure readings on both days is ≥90 mmHg.
Risk factors
Modifiable risk factors include unhealthy diets (excessive salt consumption, a diet high in saturated fat and trans fats, low intake of fruits and vegetables), physical inactivity, consumption of tobacco and alcohol, and being overweight or obese. In addition, there are environmental risk factors for hypertension and associated diseases, where air pollution is the most significant. Non-modifiable risk factors include a family history of hypertension, age over 65 years and co-existing diseases such as diabetes or kidney disease.
Most people with hypertension don’t feel any symptoms. Very high blood pressures can cause headaches, blurred vision, chest pain and other symptoms.
Checking your blood pressure is the best way to know if you have high blood pressure. If hypertension isn’t treated, it can cause other health conditions like kidney disease, heart disease and stroke.
People with very high blood pressure (usually 180/120 or higher) can experience symptoms including:
- severe headaches
- difficulty breathing
- blurred vision or other vision changes
- buzzing in the ears
- abnormal heart rhythm
If you are experiencing any of these symptoms and a high blood pressure, seek care immediately.
The only way to detect hypertension is to have a health professional measure blood pressure. Having blood pressure measured is quick and painless. Although individuals can measure their own blood pressure using automated devices, an evaluation by a health professional is important for assessment of risk and associated conditions.
Lifestyle changes can help lower high blood pressure. These include:
- eating a healthy, low-salt diet
- losing weight
- being physically active
- quitting tobacco.
If you have high blood pressure, your doctor may recommend one or more medicines. Your recommended blood pressure goal may depend on what other health conditions you have.
Blood pressure goal is less than 130/80 if you have:
- cardiovascular disease (heart disease or stroke)
- diabetes (high blood sugar)
- chronic kidney disease
- high risk for cardiovascular disease.
For most people, the goal is to have a blood pressure less than 140/90.
There are several common blood pressure medicines:
- ACE inhibitors including enalapril and lisinopril relax blood vessels and prevent kidney damage.
- Angiotensin-2 receptor blockers (ARBs) including losartan and telmisartan relax blood vessels and prevent kidney damage.
- Calcium channel blockers including amlodipine and felodipine relax blood vessels.
- Diuretics including hydrochlorothiazide and chlorthalidone eliminate extra water from the body, lowering blood pressure.
Lifestyle changes can help lower high blood pressure and can help anyone with hypertension. Many who make these changes will still need to take medicine.
These lifestyle changes can help prevent and lower high blood pressure.
- Eat more vegetables and fruits.
- Get at least 150 minutes per week of moderate-intensity aerobic activity or 75 minutes per week of vigorous aerobic activity.
- Do strength building exercises 2 or more days each week.
- Lose weight if you’re overweight or obese.
- Take medicines as prescribed by your health care professional.
- Keep appointments with your health care professional.
Don’t:
- eat too much salty food (try to stay under 2 grams per day)
- eat foods high in saturated or trans fats
- smoke or use tobacco
- drink too much alcohol (1 drink daily max for women, 2 for men)
- miss or share medication.
Reducing hypertension prevents heart attack, stroke and kidney damage, as well as other health problems.
Reduce the risks of hypertension by:
- reducing and managing stress
- regularly checking blood pressure
- treating high blood pressure
- managing other medical conditions
- reducing exposure to polluted air.
Complications of uncontrolled hypertension
Among other complications, hypertension can cause serious damage to the heart. Excessive pressure can harden arteries, decreasing the flow of blood and oxygen to the heart. This elevated pressure and reduced blood flow can cause:
- chest pain, also called angina;
- heart attack, which occurs when the blood supply to the heart is blocked and heart muscle cells die from lack of oxygen. The longer the blood flow is blocked, the greater the damage to the heart;
- heart failure, which occurs when the heart cannot pump enough blood and oxygen to other vital body organs; and
- irregular heart beat which can lead to a sudden death.
Hypertension can also burst or block arteries that supply blood and oxygen to the brain, causing a stroke.
In addition, hypertension can cause kidney damage, leading to kidney failure.
Hypertension in low- and middle-income countries
The prevalence of hypertension varies across regions and country income groups. The WHO African Region has the highest prevalence of hypertension (27%) while the WHO Region of the Americas has the lowest prevalence of hypertension (18%).
The number of adults with hypertension increased from 594 million in 1975 to 1.13 billion in 2015, with the increase seen largely in low- and middle-income countries. This increase is due mainly to a rise in hypertension risk factors in those populations.
WHO response
The World Health Organization (WHO) supports countries to reduce hypertension as a public health problem.
In 2021, WHO released a new guideline for on the pharmacological treatment of hypertension in adults. The publication provides evidence-based recommendations for the initiation of treatment of hypertension, and recommended intervals for follow-up. The document also includes target blood pressure to be achieved for control, and information on who, in the health-care system, can initiate treatment.
To support governments in strengthening the prevention and control of cardiovascular disease, WHO and the United States Centers for Disease Control and Prevention (U.S. CDC) launched the Global Hearts Initiative in September 2016, which includes the HEARTS technical package. The six modules of the HEARTS technical package (Healthy-lifestyle counselling, Evidence-based treatment protocols, Access to essential medicines and technology, Risk-based management, Team-based care, and Systems for monitoring) provide a strategic approach to improve cardiovascular health in countries across the world.
In September 2017, WHO began a partnership with Resolve to Save Lives, an initiative of Vital Strategies, to support national governments to implement the Global Hearts Initiative. Other partners contributing to the Global Hearts Initiative are the CDC Foundation, the Global Health Advocacy Incubator, the Johns Hopkins Bloomberg School of Public Health, the Pan American Health Organization (PAHO) and the U.S. CDC. Since implementation of the programme in 2017 in 31 countries low- and middle-income countries, 7.5 million people have been put on protocol-based hypertension treatment through person-centred models of care. These programmes demonstrate the feasibility and effectiveness of standardized hypertension control programmes.
- More on hypertension
High blood pressure (hypertension)
On this page, alternative medicine, coping and support, preparing for your appointment.

- Hypertension FAQs
Hi. I'm Dr. Leslie Thomas, a nephrologist at Mayo Clinic. And I'm here to answer some of the important questions you might have about hypertension.
What is the best way to measure my blood pressure at home?
Measuring your blood pressure at home is a straightforward process. Many people have a slightly higher blood pressure in one arm versus the other. So it's important to measure the blood pressures in the arm with the higher readings. It's best to avoid caffeine, exercise and, if you smoke, smoking for at least 30 minutes. To prepare for the measurement, you should be relaxed with your feet on the floor and legs uncrossed, and your back supported for at least five minutes. Your arms should be supported on a flat surface. After resting for five minutes, at least two readings are taken one minute apart in the morning prior to medications and in the evening before the evening meal. Your blood pressure monitor should be checked for proper calibration every year.
What could be causing my blood pressure to be quite erratic?
This pattern of abrupt changes in blood pressure from normal to quite high is sometimes referred to as labile blood pressure. For those who develop labile blood pressure, heart problems, hormonal problems, neurological problems, or even psychological conditions might be present. Finding and treating the underlying cause of labile blood pressure can significantly improve the condition.
Should I restrict salt to reduce my blood pressure?
It's important to note that some people with high blood pressure already consume a diet significantly restricted in sodium. And those people further restriction of dietary sodium would not necessarily be helpful or even recommended. In many people, dietary sodium intake is though relatively high. Therefore, an effective target to consider for those people is less than 1500 milligrams per day. Many though, will benefit from a target of less than a 1000 milligrams per day. Following dietary sodium restriction, it may take some time, even weeks, for the blood pressure to improve and stabilize at a lower range. So it is critically important to both be consistent with decreased sodium intake and patient when assessing for improvement.
How can I lower my blood pressure without medication?
This is a very common question. A lot of people want to avoid medication if they can, when trying to reduce their blood pressure. A few ways have been shown scientifically to reduce blood pressure. The first, and perhaps most important, is to stay physically active. Losing weight also can be important in a lot of different people. Limiting alcohol, reducing sodium intake, and increasing dietary potassium intake can all help.
What is the best medication to take for hypertension?
There's not one best medication for the treatment of hypertension for everyone. Because an individual's historical and present medical conditions must be considered. Additionally, every person has a unique physiology. Assessing how certain physiological forces may be present to contribute to the hypertension in an individual allows for a rational approach to medication choice. Antihypertensive medications are grouped by class. Each class of medication differs from the other classes by the way it lowers blood pressure. For instance, diuretics, no matter the type, act to reduce the body's total content of salt and water. This leads to reduction in plasma volume within the blood vessels and consequently a lower blood pressure. Calcium channel blockers reduce the relative constriction of blood vessels. This reduced vasoconstriction also promotes a lower blood pressure. Other classes of antihypertensive medication act in their own ways. Considering your health conditions, physiology, and how each medication works, your doctor can advise the safest and most effective medication for you.
Are certain blood pressure medications harmful to my kidneys?
Following the correction of blood pressure or the institution of certain blood pressure medications, it's pretty common to see changes in the markers for kidney function on blood tests. However, small changes in these markers, which reflects small changes in kidney filtration performance shouldn't necessarily be interpreted as absolute evidence of kidney harm. Your doctor can interpret changes in laboratory tests following any change in medication.
How can I be the best partner to my medical team?
Keep an open dialogue with your medical team about your goals and personal preferences. Communication, trust and collaboration are key to long-term success managing your blood pressure. Never hesitate to ask your medical team any questions or concerns you have. Being informed makes all the difference. Thanks for your time and we wish you well.
To diagnose high blood pressure, your health care provider examines you and asks questions about your medical history and any symptoms. Your provider listens to your heart using a device called a stethoscope.
Your blood pressure is checked using a cuff, usually placed around your arm. It's important that the cuff fits. If it's too big or too small, blood pressure readings can vary. The cuff is inflated using a small hand pump or a machine.

Blood pressure measurement
A blood pressure reading measures the pressure in the arteries when the heart beats (top number, called systolic pressure) and between heartbeats (bottom number, called diastolic pressure). To measure blood pressure, an inflatable cuff is usually placed around the arm. A machine or small hand pump is used to inflate the cuff. In this image, a machine records the blood pressure reading. This is called an automated blood pressure measurement.
The first time your blood pressure is checked, it should be measured in both arms to see if there's a difference. After that, the arm with the higher reading should be used.
Blood pressure is measured in millimeters of mercury (mm Hg). A blood pressure reading has two numbers.
- Top number, called systolic pressure. The first, or upper, number measures the pressure in the arteries when the heart beats.
- Bottom number, called diastolic pressure. The second, or lower, number measures the pressure in the arteries between heartbeats.
High blood pressure (hypertension) is diagnosed if the blood pressure reading is equal to or greater than 130/80 millimeters of mercury (mm Hg). A diagnosis of high blood pressure is usually based on the average of two or more readings taken on separate occasions.
Blood pressure is grouped according to how high it is. This is called staging. Staging helps guide treatment.
- Stage 1 hypertension. The top number is between 130 and 139 mm Hg or the bottom number is between 80 and 89 mm Hg .
- Stage 2 hypertension. The top number is 140 mm Hg or higher or the bottom number is 90 mm Hg or higher.
Sometimes the bottom blood pressure reading is normal (less than 80 mm Hg ) but the top number is high. This is called isolated systolic hypertension. It's a common type of high blood pressure in people older than 65.
If you are diagnosed with high blood pressure, your provider may recommend tests to check for a cause.
- Ambulatory monitoring. A longer blood pressure monitoring test may be done to check blood pressure at regular times over six or 24 hours. This is called ambulatory blood pressure monitoring. However, the devices used for the test aren't available in all medical centers. Check with your insurer to see if ambulatory blood pressure monitoring is a covered service.
- Lab tests. Blood and urine tests are done to check for conditions that can cause or worsen high blood pressure. For example, tests are done to check your cholesterol and blood sugar levels. You may also have lab tests to check your kidney, liver and thyroid function.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the heart's electrical activity. It can tell how fast or how slow the heart is beating. During an electrocardiogram (ECG), sensors called electrodes are attached to the chest and sometimes to the arms or legs. Wires connect the sensors to a machine, which prints or displays results.
- Echocardiogram. This noninvasive exam uses sound waves to create detailed images of the beating heart. It shows how blood moves through the heart and heart valves.
Taking your blood pressure at home
Your health care provider may ask you to regularly check your blood pressure at home. Home monitoring is a good way to keep track of your blood pressure. It helps your care providers know if your medicine is working or if your condition is getting worse.
Home blood pressure monitors are available at local stores and pharmacies.
For the most reliable blood pressure measurement, the American Heart Association recommends using a monitor with a cuff that goes around your upper arm, when available.
Devices that measure your blood pressure at your wrist or finger aren't recommended by the American Heart Association because they can provide less reliable results.
More Information
- Blood pressure chart
- Blood pressure test
Changing your lifestyle can help control and manage high blood pressure. Your health care provider may recommend that you make lifestyle changes including:
- Eating a heart-healthy diet with less salt
- Getting regular physical activity
- Maintaining a healthy weight or losing weight
- Limiting alcohol
- Not smoking
- Getting 7 to 9 hours of sleep daily
Sometimes lifestyle changes aren't enough to treat high blood pressure. If they don't help, your provider may recommend medicine to lower your blood pressure.
Medications
The type of medicine used to treat hypertension depends on your overall health and how high your blood pressure is. Two or more blood pressure drugs often work better than one. It can take some time to find the medicine or combination of medicines that works best for you.
When taking blood pressure medicine, it's important to know your goal blood pressure level. You should aim for a blood pressure treatment goal of less than 130/80 mm Hg if:
- You're a healthy adult age 65 or older
- You're a healthy adult younger than age 65 with a 10% or higher risk of developing cardiovascular disease in the next 10 years
- You have chronic kidney disease, diabetes or coronary artery disease
The ideal blood pressure goal can vary with age and health conditions, particularly if you're older than age 65.
Medicines used to treat high blood pressure include:
Water pills (diuretics). These drugs help remove sodium and water from the body. They are often the first medicines used to treat high blood pressure.
There are different classes of diuretics, including thiazide, loop and potassium sparing. Which one your provider recommends depends on your blood pressure measurements and other health conditions, such as kidney disease or heart failure. Diuretics commonly used to treat blood pressure include chlorthalidone, hydrochlorothiazide (Microzide) and others.
A common side effect of diuretics is increased urination. Urinating a lot can reduce potassium levels. A good balance of potassium is necessary to help the heart beat correctly. If you have low potassium (hypokalemia), your provider may recommend a potassium-sparing diuretic that contains triamterene.
- Angiotensin-converting enzyme (ACE) inhibitors. These drugs help relax blood vessels. They block the formation of a natural chemical that narrows blood vessels. Examples include lisinopril (Prinivil, Zestril), benazepril (Lotensin), captopril and others.
- Angiotensin II receptor blockers (ARBs). These drugs also relax blood vessels. They block the action, not the formation, of a natural chemical that narrows blood vessels. angiotensin II receptor blockers (ARBs) include candesartan (Atacand), losartan (Cozaar) and others.
Calcium channel blockers. These drugs help relax the muscles of the blood vessels. Some slow your heart rate. They include amlodipine (Norvasc), diltiazem (Cardizem, Tiazac, others) and others. Calcium channel blockers may work better for older people and Black people than do angiotensin-converting enzyme (ACE) inhibitors alone.
Don't eat or drink grapefruit products when taking calcium channel blockers. Grapefruit increases blood levels of certain calcium channel blockers, which can be dangerous. Talk to your provider or pharmacist if you're concerned about interactions.
Other medicines sometimes used to treat high blood pressure
If you're having trouble reaching your blood pressure goal with combinations of the above medicines, your provider may prescribe:
- Alpha blockers. These medicines reduce nerve signals to blood vessels. They help lower the effects of natural chemicals that narrow blood vessels. Alpha blockers include doxazosin (Cardura), prazosin (Minipress) and others.
- Alpha-beta blockers. Alpha-beta blockers block nerve signals to blood vessels and slow the heartbeat. They reduce the amount of blood that must be pumped through the vessels. Alpha-beta blockers include carvedilol (Coreg) and labetalol (Trandate).
Beta blockers. These medicines reduce the workload on the heart and widen the blood vessels. This helps the heart beat slower and with less force. Beta blockers include atenolol (Tenormin), metoprolol (Lopressor, Toprol-XL, Kapspargo sprinkle) and others.
Beta blockers aren't usually recommended as the only medicine prescribed. They may work best when combined with other blood pressure drugs.
- Aldosterone antagonists. These drugs may be used to treat resistant hypertension. They block the effect of a natural chemical that can lead to salt and fluid buildup in the body. Examples are spironolactone (Aldactone) and eplerenone (Inspra).
Renin inhibitors. Aliskiren (Tekturna) slows the production of renin, an enzyme produced by the kidneys that starts a chain of chemical steps that increases blood pressure.
Due to a risk of serious complications, including stroke, you shouldn't take aliskiren with ACE inhibitors or ARBs .
- Vasodilators. These medicines stop the muscles in the artery walls from tightening. This prevents the arteries from narrowing. Examples include hydralazine and minoxidil.
- Central-acting agents. These medicines prevent the brain from telling the nervous system to increase the heart rate and narrow the blood vessels. Examples include clonidine (Catapres, Kapvay), guanfacine (Intuniv) and methyldopa.
Always take blood pressure medicines as prescribed. Never skip a dose or abruptly stop taking blood pressure medicines. Suddenly stopping certain ones, such as beta blockers, can cause a sharp increase in blood pressure called rebound hypertension.
If you skip doses because of cost, side effects or forgetfulness, talk to your care provider about solutions. Don't change your treatment without your provider's guidance.
Treating resistant hypertension
You may have resistant hypertension if:
- You take at least three different blood pressure drugs, including a diuretic. But your blood pressure remains stubbornly high.
- You're taking four different medicines to control high blood pressure. Your care provider should check for a possible second cause of the high blood pressure.
Having resistant hypertension doesn't mean your blood pressure will never get lower. If you and your provider can determine the cause, a more effective treatment plan can be created.
Treating resistant hypertension may involve many steps, including:
- Changing blood pressure medicines to find the best combination and dosage.
- Reviewing all your medicines, including those bought without a prescription.
- Checking blood pressure at home to see if medical appointments cause high blood pressure. This is called white coat hypertension.
- Eating healthy, managing weight and making other recommended lifestyle changes.
High blood pressure during pregnancy
If you have high blood pressure and are pregnant, discuss with your care providers how to control blood pressure during your pregnancy.
Potential future treatments
Researchers have been studying the use of heat to destroy specific nerves in the kidney that may play a role in resistant hypertension. The method is called renal denervation. Early studies showed some benefit. But more-robust studies found that it doesn't significantly lower blood pressure in people with resistant hypertension. More research is underway to determine what role, if any, this therapy may have in treating hypertension.
- Alpha blockers
- Angiotensin II receptor blockers
- Angiotensin-converting enzyme (ACE) inhibitors
- Beta blockers
- Calcium channel blockers
- Central-acting agents
- Choosing blood pressure medicines
- Vasodilators
- Beta blockers: Do they cause weight gain?
- Beta blockers: How do they affect exercise?
- Blood pressure medications: Can they raise my triglycerides?
- Calcium supplements: Do they interfere with blood pressure drugs?
- Diuretics: A cause of low potassium?
From Mayo Clinic to your inbox
Clinical trials.
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
A commitment to a healthy lifestyle can help prevent and manage high blood pressure. Try these heart-healthy strategies:
- Eat healthy foods. Eat a healthy diet. Try the Dietary Approaches to Stop Hypertension (DASH) diet. Choose fruits, vegetables, whole grains, poultry, fish and low-fat dairy foods. Get plenty of potassium from natural sources, which can help lower blood pressure. Eat less saturated fat and trans fat.
- Use less salt. Processed meats, canned foods, commercial soups, frozen dinners and certain breads can be hidden sources of salt. Check food labels for the sodium content. Limit foods and beverages that are high in sodium. A sodium intake of 1,500 mg a day or less is considered ideal for most adults. But ask your provider what's best for you.
- Limit alcohol. Even if you're healthy, alcohol can raise your blood pressure. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women, and up to two drinks a day for men. One drink equals 12 ounces of beer, 5 ounces of wine or 1.5 ounces of 80-proof liquor.
- Don't smoke. Tobacco injures blood vessel walls and speeds up the process of hardening of the arteries. If you smoke, ask your care provider for strategies to help you quit.
- Maintain a healthy weight. If you're overweight or have obesity, losing weight can help control blood pressure and lower the risk of complications. Ask your health care provider what weight is best for you. In general, blood pressure drops by about 1 mm Hg with every 2.2 pounds (1 kilogram) of weight lost. In people with high blood pressure, the drop in blood pressure may be even more significant per kilogram of weight lost.
Get more exercise. Regular exercise keeps the body healthy. It can lower blood pressure, ease stress, manage weight and reduce the risk of chronic health conditions. Aim to get at least 150 minutes a week of moderate aerobic activity or 75 minutes a week of vigorous aerobic activity, or a combination of the two.
If you have high blood pressure, consistent moderate- to high-intensity workouts can lower your top blood pressure reading by about 11 mm Hg and the bottom number by about 5 mm Hg .
- Practice good sleep habits. Poor sleep may increase the risk of heart disease and other chronic conditions. Adults should aim to get 7 to 9 hours of sleep daily. Kids often need more. Go to bed and wake at the same time every day, including on weekends. If you have trouble sleeping, talk to your provider about strategies that might help.
- Manage stress. Find ways to help reduce emotional stress. Getting more exercise, practicing mindfulness and connecting with others in support groups are some ways to reduce stress.
- Try slow, deep breathing. Practice taking deep, slow breaths to help relax. Some research shows that slow, paced breathing (5 to 7 deep breaths per minute) combined with mindfulness techniques can reduce blood pressure. There are devices available to promote slow, deep breathing. According to the American Heart Association, device-guided breathing may be a reasonable nondrug option for lowering blood pressure. It may be a good option if you have anxiety with high blood pressure or can't tolerate standard treatments.
- High blood pressure and exercise
- Medication-free hypertension control
- Stress and high blood pressure
- Blood pressure medication: Still necessary if I lose weight?
- Can whole-grain foods lower blood pressure?
- High blood pressure and cold remedies: Which are safe?
- Resperate: Can it help reduce blood pressure?
- How to measure blood pressure using a manual monitor
- How to measure blood pressure using an automatic monitor
- Picnic Problems: High Sodium
- What is blood pressure?
Diet and exercise are the best ways to lower blood pressure. But some supplements are promoted as heart healthy. These supplements include:
- Fiber, such as blond psyllium and wheat bran
- Minerals, such as magnesium, calcium and potassium
- Supplements or products that increase nitric oxide or widen blood vessels — called vasodilators — such as cocoa, coenzyme Q10, L-arginine and garlic
- Omega-3 fatty acids, found in fatty fish, high-dose fish oil supplements and flaxseed
Researchers are also studying whether vitamin D can reduce blood pressure, but evidence is conflicting. More research is needed.
Talk to your care provider before adding any supplements to your blood pressure treatment. Some can interact with medicines, causing harmful side effects that could be life-threatening.
Deep breathing or mindfulness are alternative medicine techniques that can help you relax. These practices may temporarily reduce blood pressure.
- L-arginine: Does it lower blood pressure?
High blood pressure isn't something that you can treat and then ignore. It's a condition that requires regular health checkups. Some things you can do to help manage the condition are:
- Take medicines as directed. If side effects or costs pose problems, ask your provider about other options. Don't stop taking your medicines without first talking to a care provider.
- Schedule regular health checkups. It takes a team effort to treat high blood pressure successfully. Work with your provider to bring your blood pressure to a safe level and keep it there. Know your goal blood pressure level.
- Choose healthy habits. Eat healthy foods, lose excess weight and get regular physical activity. Limit alcohol. If you smoke, quit.
- Manage stress. Say no to extra tasks, release negative thoughts, and remain patient and optimistic.
- Ask for help. Sticking to lifestyle changes can be difficult, especially if you don't see or feel any symptoms of high blood pressure. It may help to ask your friends and family to help you meet your goals.
- Join a support group. You may find that talking about any concerns with others in similar situations can help.
If you think you may have high blood pressure, make an appointment with your health care provider for a blood pressure test. You might want to wear a short-sleeved shirt to your appointment so it's easier to place the blood pressure cuff around your arm.
No special preparations are necessary for a blood pressure test. To get an accurate reading, avoid caffeine, exercise and tobacco for at least 30 minutes before the test.
Because some medicines can raise blood pressure, bring a list of all medicines, vitamins and other supplements you take and their doses to your medical appointment. Don't stop taking any medicines without your provider's advice.
Appointments can be brief. Because there's often a lot to discuss, it's a good idea to be prepared for your appointment. Here's some information to help you get ready.

What you can do
- Write down any symptoms that you're having. High blood pressure rarely has symptoms, but it's a risk factor for heart disease. Let your care provider know if you have symptoms such as chest pains or shortness of breath. Doing so can help your provider decide how aggressively to treat your high blood pressure.
- Write down important medical information, including a family history of high blood pressure, high cholesterol, heart disease, stroke, kidney disease or diabetes, and any major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements that you're taking. Include dosages.
- Take a family member or friend along, if possible. Sometimes it can be difficult to remember all the information provided to you during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Be prepared to discuss your diet and exercise habits. If you don't already follow a diet or exercise routine, be ready to talk to your care provider about any challenges you might face in getting started.
- Write down questions to ask your provider.
Preparing a list of questions can help you and your provider make the most of your time together. List your questions from most important to least important in case time runs out. For high blood pressure, some basic questions to ask your provider include:
- What kinds of tests will I need?
- What is my blood pressure goal?
- Do I need any medicines?
- Is there a generic alternative to the medicine you're prescribing for me?
- What foods should I eat or avoid?
- What's an appropriate level of physical activity?
- How often do I need to schedule appointments to check my blood pressure?
- Should I monitor my blood pressure at home?
- I have other health conditions. How can I best manage them together?
- Are there brochures or other printed material that I can have? What websites do you recommend?
Don't hesitate to ask any other questions that you might have.
What to expect from your doctor
Your health care provider is likely to ask you questions. Being ready to answer them may reserve time to go over any points you want to spend more time on. Your provider may ask:
- Do you have a family history of high cholesterol, high blood pressure or heart disease?
- What are your diet and exercise habits like?
- Do you drink alcohol? How many drinks do you have in a week?
- Do you smoke?
- When did you last have your blood pressure checked? What was the result?
What you can do in the meantime
It's never too early to make healthy lifestyle changes, such as quitting smoking, eating healthy foods and getting more exercise. These are the main ways to protect yourself against high blood pressure and its complications, including heart attack and stroke.
Feb 29, 2024
- High blood pressure. National Heart, Lung, and Blood Institute. https://www.nhlbi.nih.gov/health/high-blood-pressure. Accessed July 18, 2022.
- Flynn JT, et al. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics. 2017; doi:10.1542/peds.2017-1904.
- Physical Activity Guidelines for Americans. 2nd ed. U.S. Department of Health and Human Services. https://health.gov/our-work/physical-activity/current-guidelines. Accessed June 15, 2022.
- Hypertension in adults: Screening. U.S. Preventive Services Task Force. https://uspreventiveservicestaskforce.org/uspstf/recommendation/hypertension-in-adults-screening. Accessed July 18, 2022.
- Thomas G, et al. Blood pressure measurement in the diagnosis and treatment of hypertension in adults. https://www.uptodate.com/contents/search. Accessed July 18, 2022.
- Muntner P, et al. Measurement of blood pressure in humans: A scientific statement from the American Heart Association. Hypertension. 2019; doi:10.1161/HYP.0000000000000087.
- Basile J, et al. Overview of hypertension in adults. https://www.uptodate.com/contents/search. Accessed July 22, 2022.
- Know your risk factors for high blood pressure. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/why-high-blood-pressure-is-a-silent-killer/know-your-risk-factors-for-high-blood-pressure. Accessed July 18, 2022.
- Rethinking drinking. Alcohol and your health. National Institute on Alcohol Abuse and Alcoholism. https://www.rethinkingdrinking.niaaa.nih.gov/Default.aspx. Accessed July 18, 2022.
- Libby P, et al., eds. Systemic hypertension: Mechanisms, diagnosis, and treatment. In: Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Elsevier; 2022. https://www.clinicalkey.com. Accessed July 18, 2022.
- AskMayoExpert. Hypertension (adult). Mayo Clinic; 2021.
- About metabolic syndrome. American Heart Association. https://www.heart.org/en/health-topics/metabolic-syndrome/about-metabolic-syndrome. Accessed July 18, 2022.
- Understanding blood pressure readings. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings. Accessed July 18, 2022.
- Whelton PK, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018; doi:10.1161/HYP.0000000000000065.
- Monitoring your blood pressure at home. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings/monitoring-your-blood-pressure-at-home. Accessed July 18, 2022.
- Mann JF. Choice of drug therapy in primary (essential) hypertension. https://www.uptodate.com/contents/search. Accessed July 18, 2022.
- Agasthi P, et al. Renal denervation for resistant hypertension in the contemporary era: A systematic review and meta-analysis. Scientific Reports. 2019; doi:10.1038/s41598-019-42695-9.
- Chernova I, et al. Resistant hypertension updated guidelines. Current Cardiology Reports. 2019; doi:10.1007/s11886-019-1209-6.
- Forman JP, et al. Diet in the treatment and prevention of hypertension. https://www.uptodate.com/contents/search. Accessed July 18, 2022.
- Goldman L, et al., eds. Cognitive impairment and dementia. In: Goldman-Cecil Medicine. 26th ed. Elsevier; 2020. https://www.clinicalkey.com. Accessed July 18, 2022.
- Managing stress to control high blood pressure. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/changes-you-can-make-to-manage-high-blood-pressure/managing-stress-to-control-high-blood-pressure. Accessed July 18, 2022.
- Brenner J, et al. Mindfulness with paced breathing reduces blood pressure. Medical Hypothesis. 2020; doi:10.1016/j.mehy.2020.109780.
- Grundy SM, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the management of blood cholesterol: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019; doi:10.1161/CIR.0000000000000625.
- Monitoring your blood pressure at home. American Heart Association. https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings/monitoring-your-blood-pressure-at-home. Accessed July 22, 2022.
- Natural medicines in the clinical management of hypertension. Natural Medicines. https://naturalmedicines.therapeuticresearch.com. Accessed Dec. 20, 2020.
- Saper RB, et al. Overview of herbal medicine and dietary supplements. https://www.uptodate.com/contents/search. Accessed July 18, 2022.
- Lopez-Jimenez F (expert opinion). Mayo Clinic. Aug. 19, 2022.
- 2020-2025 Dietary Guidelines for Americans. U.S. Department of Health and Human Services and U.S. Department of Agriculture. https://www.dietaryguidelines.gov. Accessed July 18, 2022.
- Börjesson M, et al. Physical activity and exercise lower blood pressure in individuals with hypertension: Narrative review of 27 RCTs. British Journal of Sports Medicine. 2016; doi:10.1136/bjsports-2015-095786.
- Lloyd-Jones DM, et al. Life's essential 8: Updating and enhancing the American Heart Association's construct of cardiovascular health: A presidential advisory from the American Heart Association. Circulation. 2022; doi:10.1161/CIR.0000000000001078.
- American Heart Association adds sleep to cardiovascular health checklist. American Heart Association. https://newsroom.heart.org/news/american-heart-association-adds-sleep-to-cardiovascular-health-checklist. Accessed July 15, 2022.
- Symptoms & causes
- Doctors & departments
- Diseases & Conditions
- High blood pressure (hypertension) diagnosis & treatment
News from Mayo Clinic

- Alcohol: Does it affect blood pressure?
- Anxiety: A cause of high blood pressure?
- Blood pressure cuff: Does size matter?
- Blood pressure readings: Why higher at home?
- Blood pressure: Can it be higher in one arm?
- Blood pressure: Does it have a daily pattern?
- Blood pressure: Is it affected by cold weather?
- Caffeine and hypertension
- Can having vitamin D deficiency cause high blood pressure?
- Free blood pressure machines: Are they accurate?
- High blood pressure and sex
- High blood pressure dangers
- Home blood pressure monitoring
- Hypertensive crisis: What are the symptoms?
- Isolated systolic hypertension: A health concern?
- Medications and supplements that can raise your blood pressure
- Menopause and high blood pressure: What's the connection?
- Pulse pressure: An indicator of heart health?
- Sleep deprivation: A cause of high blood pressure?
- What is hypertension? A Mayo Clinic expert explains.
- White coat hypertension
- Wrist blood pressure monitors: Are they accurate?
Associated Procedures
Products & services.
- A Book: Mayo Clinic on High Blood Pressure
- Blood Pressure Monitors at Mayo Clinic Store
- The Mayo Clinic Diet Online
CON-XXXXXXXX
5X Challenge
Thanks to generous benefactors, your gift today can have 5X the impact to advance AI innovation at Mayo Clinic.

- Hypertension
- Author: Mackenzie Samson, MD; Chief Editor: Eric H Yang, MD more...
- Sections Hypertension
- Practice Essentials
- Pathophysiology
- Epidemiology
- Patient Education
- Physical Examination
- Hypertension and Cerebrovascular Disease
- Hypertensive Emergencies
- Hypertensive Heart Disease
- Hypertension in Pediatric Patients
- Hypertension in Pregnancy
- Primary Aldosteronism
- Approach Considerations
- Baseline Laboratory Evaluation
- Radiologic Studies
- Nonpharmacologic Therapy
- Pharmacologic Therapy
- Management of Diabetes and Hypertension
- Management of Hypertensive Emergencies
- Management of Hypertension in Pregnancy
- Management of Hypertension in Pediatric Patients
- Management of Hypertension in the Elderly
- Management of Hypertension in Black Patients
- Management of Ocular Hypertension
- Management of Renovascular Hypertension
- Management of Resistant Hypertension
- Management of Pseudohypertension
- Management of Pheochromocytoma
- Management of Primary Hyperaldosteronism
- Interventions for Improving Blood Pressure Control
- Medication Summary
- Diuretics, Thiazide
- Diuretic, Potassium-Sparing
- Diuretics, Loop
- Beta-Blockers, Beta-1 Selective
- Beta-Blockers, Alpha Activity
- Beta-Blockers, Intrinsic Sympathomimetic
- Vasodilators
- Calcium Channel Blockers
- Aldosterone Antagonists, Selective
- Alpha2-agonists, Central-acting
- Renin Inhibitors/Combos
- Alpha-Blockers, Antihypertensives
- Antihypertensives, Other
- Antihypertensive Combinations
- Endothelin Antagonists
- Questions & Answers
- Media Gallery
High blood pressure (BP), or hypertension, is defined by two levels by the 2017 American College of Cardiology/American Heart Association (ACC/AHA) guidelines [ 1 , 2 ] : (1) elevated BP, with a systolic pressure (SBP) between 120 and 129 mm Hg and diastolic pressure (DBP) less than 80 mm Hg, and (2) stage 1 hypertension, with an SBP of 130 to 139 mm Hg or a DBP of 80 to 89 mm Hg.
Hypertension is the most common primary diagnosis in the United States. [ 3 ] It affects approximately 86 million adults (≥20 years) in the United States [ 4 ] and is a major risk factor for stroke, myocardial infarction, vascular disease, and chronic kidney disease.
Signs and symptoms of hypertension
The 2017 ACC/AHA guidelines provide the following definitions and classifications of elevated BP and stages of hypertension [ 1 , 2 ] :
Elevated BP with a systolic pressure between 120 and 129 mm Hg and diastolic pressure less than 80 mm Hg
Stage 1 hypertension, with a systolic pressure of 130 to 139 mm Hg or a diastolic pressure of 80 to 89 mm Hg
- Stage 2 hypertension, with a systolic pressure of 140 mm Hg or greater or a diastolic pressure of 90 mm Hg or greater
Of note, the International Society of Hypertension (ISH) and the European Society of Cardiology (ESC) have a higher BP threshold, defining hypertension as an SBP of 140 mm Hg or greater and/or a DBP of 90 mm Hg or above. [ 5 , 6 ]
Hypertension may be primary, which may develop as a result of a variety of environmental or genetic causes, or it may be secondary to renal, vascular, and endocrine causes. Primary or essential hypertension accounts for 90-95% of adult cases, and secondary hypertension accounts for 2-10% of adult cases.
See Presentation for more detail.
Diagnosis of hypertension
The evaluation of hypertension involves accurately measuring the patient’s BP, performing a focused medical history and physical examination, and obtaining results of routine laboratory studies. [ 7 , 8 ] A 12-lead electrocardiogram should also be obtained. These steps can help determine the following [ 7 , 8 , 9 ] :
Presence of end-organ disease
Possible causes of hypertension
Cardiovascular risk factors
Baseline values for judging biochemical effects of therapy
Other studies may be obtained on the basis of clinical findings or in individuals with suspected secondary hypertension and/or evidence of target-organ disease, such as complete blood cell (CBC) count, basic metabolic panel; chest radiograph, transthoracic echocardiogram; and urine microalbumin. [ 7 ]
See Workup for more detail.
Management of hypertension
Many guidelines exist for the management of hypertension. Most groups, including the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood (JNC), the American Diabetes Associate (ADA), and the ACC/AHA recommend lifestyle modification as the first step in managing hypertension.
Lifestyle modifications
JNC 7 recommendations to lower BP and decrease cardiovascular disease risk include the following, with greater results achieved when two or more lifestyle modifications are combined [ 7 ] :
Weight loss (range of approximate SBP reduction, 5-20 mm Hg per 10 kg)
Limit alcohol intake to no more than 1 oz (30 mL) of ethanol per day for men or 0.5 oz (15 mL) of ethanol per day for women and people of lighter weight (range of approximate SBP reduction, 2-4 mm Hg)
Reduce sodium intake to no more than 100 mmol/day (2.4 g sodium or 6 g sodium chloride; range of approximate SBP reduction, 2-8 mm Hg) [ 10 ]
Maintain adequate intake of dietary potassium (approximately 90 mmol/day)
Maintain adequate intake of dietary calcium and magnesium for general health
Stop smoking and reduce intake of dietary saturated fat and cholesterol for overall cardiovascular health
Engage in aerobic exercise at least 30 minutes daily for most days (range of approximate SBP reduction, 4-9 mm Hg)
The ACC/AHA recommends a diet that is low in sodium, is high in potassium, and promotes the consumption of fruits, vegetables, and low-fat dairy products for reducing BP and lowering the risk of cardiovascular events. Other recommendations include increasing physical activity (30 minutes or more of moderate intensity activity on a daily basis) and losing weight (persons with overweight and obesity). [ 1 ]
The 2018 ESC and the European Society of Hypertension (ESH) guidelines recommend a low-sodium diet (limited to 2 g per day) as well as reducing body-mass index (BMI) to 20-25 kg/m 2 and waist circumference (to < 94 cm in men and < 80 cm in women). [ 11 ] The 2023 ESH guidelines for managing arterial hypertension indicates a linear reduction in BP with sodium intake limited to as low as 800 mg/day; when dietary sodium intake fell from about 3.6 g/day to around 2.7 g/day, there was an associated 18-26% fall in cardiovascular disease. [ 6 ]
Pharmacologic therapy
If lifestyle modifications are insufficient to achieve the goal BP, there are several drug options for treating and managing hypertension. Thiazide diuretics, an angiotensin-converting enzyme inhibitor (ACEI)/angiotensin receptor blocker (ARB), or calcium channel blocker (CCB) are the preferred first-line agents. [ 1 ] Often, patients require several antihypertensive agents to achieve adequate BP control.
Compelling indications for specific agents include comorbidities such as heart failure, ischemic heart disease, chronic kidney disease, and diabetes. Drug intolerability or contraindications may also be factors. [ 7 ]
The following are drug class recommendations for compelling indications based on various clinical trials [ 7 ] :
Heart failure: Diuretic, beta-blocker, ACE inhibitor/ARB/ARNI, aldosterone antagonist
Following myocardial infarction: Beta-blocker, ACE inhibitor
Diabetes: ACE inhibitor/ARB
Chronic kidney disease: ACE inhibitor/ARB
Although the 2017 ACC/AHA guidelines favor CCBs or thiazide diuretics in the absence of other indications as first-line medications in Black hypertensive populations, [ 1 ] reports in relatively recent years have raised questions on the benefits of race or ethnicity-based medication prescribing. [ 12 , 13 , 14 , 15 , 16 , 17 , 18 , 19 , 20 ]
See Treatment and Medication for more details.
Hypertension is the most common primary diagnosis in the United States, [ 3 ] and it is one of the most common worldwide diseases afflicting humans. It is a major risk factor for stroke, myocardial infarction, vascular disease, and chronic kidney disease. Despite extensive research over the past several decades, the etiology of most cases of adult hypertension is still unknown, and control of blood pressure (BP) is suboptimal in the general population. Due to the associated morbidity and mortality and cost to society, preventing and treating hypertension is an important public health challenge. Fortunately, relatively recent advances and trials in hypertension research are leading to an increased understanding of the pathophysiology of hypertension and the promise for novel pharmacologic and interventional treatments for this widespread disease.
According to the American Heart Association (AHA), approximately 86 million adults (34%) in the United States are affected by hypertension, which is defined as a systolic BP (SBP) of 130 mm Hg or more or a diastolic BP (DBP) of 80 mm Hg or more, taking antihypertensive medication, or having been told by clinicians on at least two occasions as having hypertension. [ 1 ] Substantial efforts have been made to enhance awareness and treatment of hypertension. However, a National Health Examination Survey (NHANES) spanning 2011-2014 revealed that 34% of US adults aged 20 years and older are hypertensive and NHANES 2013-2014 data showed that 15.9% of these hypertensive adults are unaware they are hypertensive; these data have increased from NHANES 2005-2006 data that showed 29% of US adults aged 18 years and older were hypertensive and that 7% of these hypertensive adults had never been told that they had hypertension. [ 4 ]
Of those with elevated BP, 78% were aware they were hypertensive, 68% were being treated with antihypertensive agents, and only 64% of treated individuals had controlled hypertension. [ 4 ] In addition, previous data from NHANES estimated that 52.6% (NHANES 2009-2010) to 55.8% (NHANES 1999-2000) of adults aged 20 years and older have elevated BP or stage 1 hypertension, defined as an untreated SBP of 120-139 mm Hg or untreated DBP of 80-89 mm Hg. [ 4 ] (See Epidemiology .)
Hypertension is the most important modifiable risk factor for coronary heart disease (the leading cause of death in North America), stroke (the third leading cause), congestive heart failure, end-stage renal disease, and peripheral vascular disease. Therefore, healthcare professionals must not only identify and treat patients with hypertension but also promote a healthy lifestyle and preventive strategies to decrease the prevalence of hypertension in the general population. (See Treatment .)
Definition and classification
The definition of abnormally high blood pressure (BP) has varied among guidelines. Nevertheless, the relationship between systemic arterial pressure and morbidity appears to be quantitative rather than qualitative. A level for high BP must be agreed upon in clinical practice for screening patients with hypertension and for instituting diagnostic evaluation and initiating therapy. Because the risk to an individual patient may correlate with the severity of hypertension, a classification system is essential for making decisions about aggressiveness of treatment or therapeutic interventions. (See Presentation .)
Based on recommendations of the 2017 ACC/AHA guidelines, the classification of BP (expressed in mm Hg) for adults aged 18 years or older is as follows [ 1 , 2 ] :
Normal: Systolic lower than 120 mm Hg and diastolic lower than 80 mm Hg
Elevated: Systolic 120-129 mm Hg and diastolic lower than 80 mm Hg
Stage 1: Systolic 130-139 mm Hg or diastolic 80-89 mm Hg
Stage 2: Systolic 140 mm Hg or greater or diastolic 90 mm Hg or greater
The classification above is based on the average of two or more readings taken at each of two or more visits after the initial screening. [ 1 ] Normal BP with respect to cardiovascular risk is less than 120/80 mm Hg. However, unusually low readings should be evaluated for clinical significance.
From another perspective, hypertension may be categorized as either primary or secondary. Primary (essential) hypertension is diagnosed in the absence of an identifiable secondary cause. Approximately 90-95% of adults with hypertension have primary hypertension, whereas secondary hypertension accounts for about 5-10% of the cases. [ 21 ] However, secondary forms of hypertension, such as primary hyperaldosteronism, account for as much as 30% of resistant hypertension (hypertension in which BP is >140/90 mm Hg despite the use of medications from three or more drug classes, one of which is a thiazide diuretic).
Especially severe cases of hypertension, or hypertensive crises, are defined as a BP of more than 180/120 mm Hg and may be further categorized as hypertensive emergencies or urgencies. Hypertensive emergencies are characterized by evidence of impending or progressive target organ dysfunction, whereas hypertensive urgencies are those situations without target organ dysfunction. [ 7 ]
Acute end-organ damage in the setting of a hypertensive emergency may include the following [ 22 ] :
Neurologic: hypertensive encephalopathy, cerebral vascular accident/cerebral infarction, subarachnoid hemorrhage, intracranial hemorrhage
Cardiovascular: myocardial ischemia/infarction, acute left ventricular dysfunction, acute pulmonary edema, aortic dissection, unstable angina pectoris
Other: acute renal failure/insufficiency, retinopathy, eclampsia, microangiopathic hemolytic anemia
With the advent of antihypertensives, the incidence of hypertensive emergencies has declined from 7% to approximately 1%. [ 23 ] In addition, the 1-year survival rate associated with this condition has increased from only 20% (prior to 1950) to more than 90% with appropriate medical treatment. [ 24 ] (See Medication .)
The pathogenesis of primary hypertension is multifactorial and complex. [ 25 ] Multiple factors modulate the blood pressure (BP) including humoral mediators, vascular reactivity, circulating blood volume, vascular caliber, blood viscosity, cardiac output, blood vessel elasticity, and neural stimulation. The pathogenesis of primary hypertension involves multiple factors, including genetic predisposition, excess dietary salt intake, adrenergic tone, and renal sodium and water handling that interact to produce BP elevations. Although genetics contribute, with rare exceptions this condition is polygenic. Emerging evidence suggests a role for immune cell activation and the microbiome in the pathogenesis of hypertension. [ 26 ]
The natural history of primary hypertension evolves from occasional to established hypertension. After a long asymptomatic period, persistent hypertension develops into complicated hypertension, in which end-organ damage to the aorta and small arteries, heart, kidneys, retina, and central nervous system is evident.
A general progression of primary hypertension is as follows:
Prehypertension in persons aged 10-30 years (by increased cardiac output)
Early hypertension in persons aged 20-40 years (in which increased peripheral resistance is prominent)
Established hypertension in persons aged 30-50 years
Complicated hypertension in persons aged 40-60 years
As evident from the above, younger individuals may present with hypertension associated with an elevated cardiac output (high-output hypertension). High-output hypertension results from volume and sodium retention by the kidney, leading to increased stroke volume and, often, with cardiac stimulation by adrenergic hyperactivity. Systemic vascular resistance is generally not increased at such earlier stages of hypertension. As hypertension is sustained, however, vascular adaptations including remodeling, vasoconstriction, and vascular rarefaction occur, leading to increased systemic vascular resistance. In this situation, cardiac output is generally normal or slightly reduced, and circulating blood volume is normal.
Cortisol reactivity, an index of hypothalamic-pituitary-adrenal function, may be another mechanism by which psychosocial stress is associated with future hypertension. [ 27 ] In a prospective sub-study of the Whitehall II cohort, with 3 years follow-up of an occupational cohort in previously healthy patients, investigators reported 15.9% of the patient group developed hypertension in response to laboratory-induced mental stressors, and there was an association between cortisol stress reactivity and incident hypertension. [ 27 ]
Investigations into the pathophysiology of hypertension, both in animals and humans, have revealed that hypertension may have an immunologic basis. Studies have revealed that hypertension is associated with renal infiltration of immune cells and that pharmacologic immunosuppression (such as with the drug mycophenolate mofetil) or pathologic immunosuppression (such as occurs with human immunovirus [HIV] deficiency) results in reduced BP in animals and humans. Evidence suggests that T lymphocytes and T-cell derived cytokines (eg, interleukin 17, tumor necrosis factor alpha) play an important role in hypertension. [ 28 , 29 ]
One hypothesis is that prehypertension results in oxidation of lipids such as arachidonic acid that leads to the formation of isoketals or isolevuglandins, which function as neoantigens, which are then presented to T cells, leading to T-cell activation and infiltration of critical organs (eg, kidney, vasculature). [ 30 ] This results in persistent or severe hypertension and end-organ damage. Sympathetic nervous system activation and noradrenergic stimuli have also been shown to promote T-lymphocyte activation and infiltration, and contribute to the pathophysiology of hypertension. [ 31 , 32 , 33 ]
Hypertension can be primary, which may develop as a result of environmental or genetic causes, or secondary, which has multiple etiologies, including renal, vascular, and endocrine causes. Primary or essential hypertension accounts for 90-95% of adult cases, and a small percentage of patients (2-10%) have a secondary cause. Hypertensive emergencies are most often precipitated by inadequate medication or poor adherence.
Environmental and genetic/epigenetic causes
Hypertension develops secondary to environmental factors, as well as multiple genes, whose inheritance appears to be complex. [ 24 , 34 ] Furthermore, obesity, diabetes, and heart disease also have genetic components and contribute to hypertension. Epidemiologic studies using twin data and data from Framingham Heart Study families reveal that blood pressure (BP) has a substantial heritable component, ranging from 33% to 57%. [ 35 , 36 , 37 ]
In an attempt to elucidate the genetic components of hypertension, multiple genome wide association studies (GWAS) have been conducted, revealing multiple gene loci in known pathways of hypertension as well as some novel genes with no known link to hypertension as of yet. [ 38 ] Further research into these novel genes, some of which are immune-related, will likely increase the understanding of the pathophysiology of hypertension, allowing for increased risk stratification and individualized treatment.
Epigenetic phenomena, such as DNA methylation and histone modification, have also been implicated in the pathogenesis of hypertension. For example, a high-salt diet appears to unmask nephron development caused by methylation. Maternal water deprivation and protein restriction during pregnancy increase renin-angiotensin expression in the fetus. Mental stress induces a DNA methylase, which enhances autonomic responsiveness. The pattern of serine protease inhibitor gene methylation predicts preeclampsia in pregnant women. [ 39 ]
Despite these genetic findings, targeted genetic therapy seems to have little impact on hypertension. In the general population, not only does it appear that individual and joint genetic mutations have very small effects on BP levels, but it has not been shown that any of these genetic abnormalities are responsible for any applicable percentage of cases of hypertension in the general population. [ 40 ]
Secondary causes of hypertension related to single genes are very rare. They include Liddle syndrome, glucocorticoid-remediable hyperaldosteronism, 11 beta-hydroxylase and 17 alpha-hydroxylase deficiencies, syndrome of apparent mineralocorticoid excess, and pseudohypoaldosteronism type II. [ 7 ]
Causes of secondary hypertension
Renal causes (2.5-6%) of hypertension include the renal parenchymal diseases and renal vascular diseases, as follows:
Polycystic kidney disease
Chronic kidney disease
Urinary tract obstruction
Renin-producing tumor
Liddle syndrome
- Nephritic syndrome/glomerulonephritis
Renovascular hypertension (RVHT) causes 0.2-4% of cases of hypertension. Since the 1934 seminal experiment by Goldblatt et al, [ 41 ] RVHT has become increasingly recognized as an important cause of clinically atypical hypertension and chronic kidney disease—the latter by virtue of renal ischemia. The coexistence of renal arterial vascular (ie, renovascular) disease and hypertension roughly defines this type of secondary hypertension. More specific diagnoses are made retrospectively when hypertension is improved after intravascular intervention.
Vascular causes include the following:
Coarctation of the aorta
Collagen vascular disease
Endocrine causes may account for the largest proportion of secondary hypertension (10-20%) and include exogenous or endogenous hormonal imbalances. Exogenous causes include administration of steroids. Primary hyperaldosteronism is the most common endogenous hormone abnormality causing hypertension. Approximately 20% of cases of confirmed resistant hypertension are due to primary hyperaldosteronism. Pheochromocytomas and paragangliomas are rare, chromaffin cell tumors, that produce catecholamines. The prevalence of these tumors is 0.01-0.2% in the hypertensive population, but up to 4% in the resistant hypertension population. Cushing syndrome is caused by excess glucocorticoids and can present in a variety of ways, including weight gain, menstrual irregularities, mood disorders, muscle weakness, abdominal striae, and enlargement of the pad fat on the dorsal neck. Small cohort studies suggest a high prevalence of hypertension in patients with Cushing syndrome; further studies are needed for accurate correlation. [ 42 ]
Another common endocrine cause of hypertension is oral contraceptive use, likely due to activation of the renin-angiotensin-aldosterone system (RAAS). This is caused by increased hepatic synthesis of angiotensinogen in response to the estrogen component of oral contraceptives. Approximately 5% of women taking oral contraceptives may develop hypertension, which abates within 6 months after discontinuation. The risk factors for oral contraceptive–associated hypertension include coexistent renal disease, familial history of primary hypertension, age older than 35 years, and obesity.
Exogenous administration of steroids used for therapeutic purposes also increases BP, especially in susceptible individuals, mainly by volume expansion. Nonsteroidal anti-inflammatory drugs (NSAIDs) may also have adverse effects on BP. NSAIDs block both cyclooxygenase-1 (COX-1) and COX-2 enzymes. The inhibition of COX-2 can inhibit its natriuretic effect, which, in turn, increases sodium retention. NSAIDs also inhibit the vasodilating effects of prostaglandins and the production of vasoconstricting factors—namely, endothelin-1. These effects can contribute to the induction of hypertension in a normotensive or controlled hypertensive patient.
Endogenous hormonal causes include the following:
Primary hyperaldosteronism
Cushing syndrome
Pheochromocytoma
Congenital adrenal hyperplasia
Neurogenic causes include the following:
Brain tumor
Autonomic dysfunction
Sleep apnea
Intracranial hypertension
Drugs and toxins that cause hypertension include the following:
Cyclosporine, tacrolimus
Erythropoietin
Adrenergic medications
Decongestants containing ephedrine
Herbal remedies and candy that contain licorice (including licorice root) or ephedrine (and ephedra)
Other causes include the following:
Hyperthyroidism and hypothyroidism
Hypercalcemia
Hyperparathyroidism
Obstructive sleep apnea
Obstructive sleep apnea (OSA) is a common but frequently undiagnosed sleep-related breathing disorder defined as an average of at least five apneic and hypopneic episodes per sleep hour, with associated symptoms, including excessive daytime sleepiness. [ 43 ] Multiple studies have shown OSA to be an independent risk factor for the development of primary hypertension, even after adjusting for age, sex, and degree of obesity.
Approximately half of individuals with hypertension have OSA, and approximately half with OSA have hypertension. Ambulatory BP monitoring normally reveals a "dip" in BP of at least 10% during sleep. However, if a patient is a "nondipper," the chances that the patient has OSA is increased. Nondipping is thought to be caused by frequent apneic/hypopneic episodes that end with arousals associated with marked spikes in BP that last for several seconds. Apneic episodes are associated with striking increases in sympathetic nerve activity and enormous elevations of BP. Individuals with sleep apnea have increased cardiovascular mortality, in part likely related to the high incidence of hypertension.
Although treatment of sleep apnea with continuous airway positive pressure (CPAP) would logically seem to improve cardiovascular outcomes and hypertension, studies evaluating this mode of therapy have been disappointing. A 2016 review of several studies indicated that CPAP either had no effect or a modest BP-lowering effect. [ 44 ] Findings from the SAVE (Sleep Apnea Cardiovascular Endpoints) study showed no effect of CPAP therapy on BP above usual care. [ 45 ] It is likely that patients with sleep apnea have other etiologies of hypertension, including obesity, hyperaldosteronism, increased sympathetic drive, and activation of the renin/angiotensin system that contribute to their hypertension. Although CPAP remains an effective therapy for other aspects of sleep apnea, it should not be expected to normalize BP in the majority of patients.
Causes of hypertensive emergencies
The most common hypertensive emergency is a rapid unexplained rise in BP in patients with chronic essential hypertension. Most patients who develop hypertensive emergencies have a history of inadequate hypertensive treatment or an abrupt discontinuation of their medications. [ 46 , 47 ]
Other causes of hypertensive emergencies include the use of recreational drugs, abrupt clonidine withdrawal, post pheochromocytoma removal, and systemic sclerosis, as well as the following:
Renal parenchymal disease: chronic pyelonephritis, primary glomerulonephritis, tubulointerstitial nephritis (accounts for 80% of all secondary causes)
Systemic disorders with renal involvement: systemic lupus erythematosus, systemic sclerosis, vasculitis
Renovascular disease: atherosclerotic disease, fibromuscular dysplasia, polyarteritis nodosa
Endocrine disease: pheochromocytoma, Cushing syndrome, primary hyperaldosteronism
Drugs: cocaine, [ 48 ] amphetamines, cyclosporine, clonidine (withdrawal), phencyclidine, diet pills, oral contraceptive pills
Drug interactions: monoamine oxidase inhibitors with tricyclic antidepressants, antihistamines, or tyramine-containing food
Central nervous system (CNS) factors: CNS trauma or spinal cord disorders, such as Guillain-Barré syndrome
Preeclampsia/eclampsia
Postoperative hypertension
Hypertension is a worldwide epidemic; accordingly, its epidemiology has been well studied. Data from the US National Health and Nutrition Examination Survey (NHANES) spanning 2011-2014 found that of those in the population aged 20 years or older, an estimated 86 million adults had hypertension, with a prevalence of 34%. [ 4 ]
More recently, 2020 data from the Centers for Disease Control and Prevention's (CDC) National Center for Health Statistics (NCHS) spanning 2017-2018 show a 45.4% prevalence of hypertension among those aged 18 and older (see the following image; prevalence by sex and age). [ 49 ] Of the US adult population diagnosed with hypertension, a higher prevalence exists in males (51%) relative to females (39.7%).
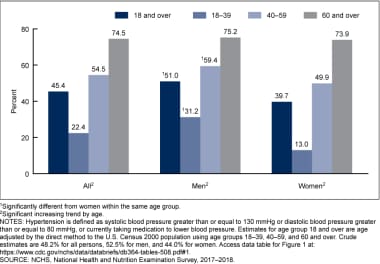
There has been an interesting trend in the prevalence of hypertension, which fell in the early 2000s but began trending upward in 2014 (see the image below, which shows the prevalence of hypertension by year and sex). [ 49 ] The prevalence of hypertension declined during the first decade of this century, but it has since increased, particularly in men.
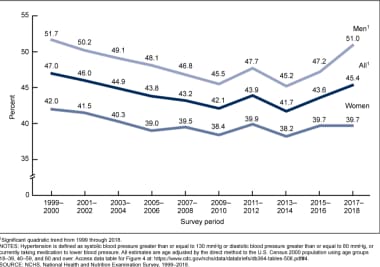
Globally, an estimated 26% of the world’s population (972 million people) has hypertension, and the prevalence is expected to increase to 29% by 2025, driven largely by increases in economically developing nations. [ 50 ] The high prevalence of hypertension exacts a tremendous public health burden. For example, as a primary contributor to heart disease and stroke, the first and third leading causes of death worldwide, respectively, high BP was the top modifiable risk factor for disability adjusted life-years lost worldwide in 2013. [ 51 , 52 ]
Hypertension and sex- and age-related statistics
Females have a lower prevalence of hypertension until the fifth decade of life. Afterward, the prevalence of hypertension is increased in females compared to males. [ 1 ]
Hypertension and race and ethnicity
Black adults have among the highest rates of hypertension, with an increasing prevalence, in the United States and globally. [ 17 , 18 , 19 , 53 ] Although White adults also have an increasing incidence of high BP, they develop this condition later in life than Black adults and have much lower average BPs. In fact, compared to hypertensive White persons, hypertensive Black individuals have a 1.3-fold higher rate of nonfatal stroke, a 1.8-fold higher rate of fatal stroke, a 1.5-fold higher mortality rate due to heart disease, and a 4.2-fold higher rate of end-stage renal disease (ESRD). [ 54 ]
Table 2, below, summarizes age-adjusted prevalence estimates from the National Health Interview Survey (NHIS) and the NCHS according to racial/ethnic groups and diagnosed conditions in individuals aged 18 years and older.
Table 2. NHIS/NCHS Age-Adjusted Prevalence Estimates in Individuals Aged 18 Years and Older in 2015. (Open Table in a new window)
Race/Ethnic Group | Have Hypertension, % | Have Heart Disease, % | Have Coronary Heart Disease, % | Have Had a Stroke, % |
White only | 23.8 | 11.3 | 5.6 | 2.4 |
Black/African American | 34.4 | 9.5 | 5.4 | 3.7 |
Hispanic/Latino | 23.0 | 8.2 | 5.1 | 2.4 |
Asian | 20.6 | 7.1 | 3.7 | 1.4 |
American Indian/Alaska Native | 28.4 | 13.7 | 9.3 | 2.2 (this number is considered unreliable) |
Source: Summary health statistics: National Health Interview Survey, 2015. Available at: . Accessed: November 14, 2016. NCHS = National Center for Health Statistics; NHIS = National Health Interview Survey. | ||||
Most individuals diagnosed with hypertension will have increasing blood pressure (BP) as they age. Untreated hypertension is notorious for raising the mortality risk and is often described as a silent killer. Mild to moderate hypertension, if left untreated, may be associated with a risk of atherosclerotic disease in 30% of people and of organ damage in 50% of persons within 8-10 years after onset. Patients with resistant hypertension are also at higher risk for poor outcomes, particularly those with certain comorbidities (eg, chronic kidney disease, ischemic heart disease). [ 55 ] Patients with resistant hypertension who have lower BP appear to have a reduced risk for some cardiovascular events (eg, incident stroke, coronary heart disease, or heart failure). [ 55 ]
Death from ischemic heart disease or stroke increases progressively as BP increases. For every 20 mm Hg systolic or 10 mm Hg diastolic increase in BP above 115/75 mm Hg, mortality doubles for both ischemic heart disease and stroke. [ 7 ]
Hypertensive retinopathy was associated with an increased long-term risk of stroke, even in patients with well-controlled BP, in a report of 2907 adults with hypertension participating in the Atherosclerosis Risk in Communities (ARIC) study. [ 56 , 57 ] Increasing severity of hypertensive retinopathy was associated with an increased risk of stroke; the stroke risk was 1.35 in the mild retinopathy group and 2.37 in the moderate/severe group.
In a meta-analysis of pooled data from 19 prospective cohort studies involving 762,393 patients, Huang et al reported that, after adjustment for multiple cardiovascular risk factors, prehypertension was associated with a 66% increased risk for stroke, compared with an optimal BP (< 120/80 mm Hg). [ 58 , 59 ] Patients in the high range of prehypertension (130-139/85-89 mm Hg) had a 95% increased risk of stroke, compared to a 44% increased risk for those in the low range of prehypertension (120-129/80-84 mm Hg). [ 58 , 59 ]
The morbidity and mortality of hypertensive emergencies depend on the extent of end-organ dysfunction on presentation and the degree to which BP is controlled subsequently. With BP control and medication adherence, the 10-year survival of patients with hypertensive crises approaches 70%. [ 60 ]
In the Framingham Heart Study, the age-adjusted risk of congestive heart failure was 2.3 times higher in men and 3 times higher in women when the highest BP was compared to the lowest BP. [ 61 ] Multiple Risk Factor Intervention Trial (MRFIT) data showed that the relative mortality risk for coronary artery disease was 2.3 to 6.9 times higher for persons with mild to severe hypertension than it was for persons with normal BP. [ 62 ] The relative risk for stroke ranged from 3.6 to 19.2. The population-attributable risk percentage for coronary artery disease varied from 2.3 to 25.6%, whereas the population-attributable risk for stroke ranged from 6.8% to 40%. [ 62 ]
The Framingham Heart Study also found a 72% increase in the risk of all-cause death and a 57% increase in the risk of any cardiovascular event in patients with hypertension who were also diagnosed with diabetes mellitus. [ 63 ]
Nephrosclerosis is one of the possible complications of long-standing hypertension. The risk of hypertension-induced end-stage renal disease is higher in Black patients, even when BP is under good control. Furthermore, patients with diabetic nephropathy who are hypertensive are also at high risk for developing end-stage renal disease.
Comparative data from the National Health Examination Survey (NHANES) I and III showed a decrease in mortality over time in hypertensive adults, but the mortality gap between hypertensive and normotensive adults remained high. [ 64 ]
Clinical trials have demonstrated the following benefits with antihypertensive therapy [ 7 ] :
Average 35-40% reduction in stroke incidence
Average 20-25% reduction in myocardial infarction
Average greater than 50% reduction in heart failure
Moreover, it is estimated that 1 death is prevented per 11 patients treated for stage 1 hypertension and other cardiovascular risk factors when a sustained reduction of 12 mm Hg in systolic BP over 10 years is achieved. [ 7 ] However, for the same lowering in systolic BP reduction, it is estimated that 1 death is prevented per 9 patients treated when cardiovascular disease or end-organ damage is present. [ 7 ]
Hypertension is a lifelong disorder. For optimal control, a long-term commitment to lifestyle modifications and pharmacologic therapy is required. Therefore, repeated in-depth patient education and counseling not only improves compliance with medical therapy but also reduces cardiovascular risk factors.
Various strategies to decrease cardiovascular disease risk include the following:
Prevention and treatment of obesity: An increase in body mass index (BMI) and waist circumference is associated with an increased risk of developing conditions with high cardiovascular risk, such as hypertension, diabetes mellitus, impaired fasting glucose, and left ventricular hypertrophy [ 65 ]
Appropriate amounts of aerobic physical activity
Diets low in salt, total fat, and cholesterol
Adequate dietary intake of potassium, calcium, and magnesium
Limited alcohol consumption
Avoidance of cigarette smoking
Avoidance of the use of illicit drugs, such as cocaine
[Guideline] Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension . 2018 Jun. 71(6):e13-e115. [QxMD MEDLINE Link] . [Full Text] .
Jeffrey S. New ACC/AHA hypertension guidelines make 130 the new 140. Medscape Medical News. November 13, 2017. Available at https://www.medscape.com/viewarticle/888560 . Accessed: November 18, 2017.
Rivera SL, Martin J, Landry J. Acute and chronic hypertension: what clinicians need to know for diagnosis and management. Crit Care Nurs Clin North Am . 2019 Mar. 31(1):97-108. [QxMD MEDLINE Link] .
Benjamin EJ, Blaha MJ, Chiuve SE, et al, for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2017 update: a report from the American Heart Association. Circulation . 2017 Mar 7. 135(10):e146-e603. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Unger T, Borghi C, Charchar F, et al. 2020 International Society of Hypertension global hypertension practice guidelines. Hypertension . 2020 Jun. 75(6):1334-57. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Mancia G, Kreutz R, Brunström M, et al, for The Task Force for the management of arterial hypertension of the European Society of Hypertension: Endorsed by the International Society of Hypertension (ISH) and the European Renal Association (ERA). 2023 ESH Guidelines for the management of arterial hypertension. J Hypertens . 2023 Dec 1. 41 (12):1874-2071. [QxMD MEDLINE Link] . [Full Text] .
Chobanian AV, Bakris GL, Black HR, et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension . 2003 Dec. 42(6):1206-52. [QxMD MEDLINE Link] .
Katakam R, Brukamp K, Townsend RR. What is the proper workup of a patient with hypertension?. Cleve Clin J Med . 2008 Sep. 75(9):663-72. [QxMD MEDLINE Link] .
Institute for Clinical Systems Improvement (ICSI). Hypertension diagnosis and treatment . Bloomington, Minn: Institute for Clinical Systems Improvement (ICSI); 2010.
Whelton PK, Appel LJ, Sacco RL, et al. Sodium, blood pressure, and cardiovascular disease: further evidence supporting the American Heart Association sodium reduction recommendations. Circulation . 2012 Dec 11. 126(24):2880-9. [QxMD MEDLINE Link] .
[Guideline] Williams B, Mancia G, Spiering W, et al, for the ESC Scientific Document Group. 2018 ESC/ESH guidelines for the management of arterial hypertension. Eur Heart J . 2018 Sep 1. 39 (33):3021-104. [QxMD MEDLINE Link] . [Full Text] .
Gopal DP, Okoli GN, Rao M. Re-thinking the inclusion of race in British hypertension guidance. J Hum Hypertens . 2022 Mar. 36(3):333-5. [QxMD MEDLINE Link] . [Full Text] .
Gopal DP, Francis R. Does race belong in the hypertension guidelines?. J Hum Hypertens . 2021 Oct. 35(10):940-1. [QxMD MEDLINE Link] .
Holt HK, Gildengorin G, Karliner L, Fontil V, Pramanik R, Potter MB. Differences in hypertension medication prescribing for Black Americans and their association with hypertension outcomes. J Am Board Fam Med . 2022 Jan-Feb. 35(1):26-34. [QxMD MEDLINE Link] . [Full Text] .
Apeles L. Race-based prescribing for Black people with high blood pressure shows no benefit. University of California San Francisco. Available at https://www.ucsf.edu/news/2022/01/422151/race-based-prescribing-black-people-high-blood-pressure-shows-no-benefit . January 18, 2022; Accessed: February 27, 2024.
Abrahamowicz AA, Ebinger J, Whelton SP, Commodore-Mensah Y, Yang E. Racial and ethnic disparities in hypertension: barriers and opportunities to Improve Blood Pressure Control. Curr Cardiol Rep . 2023 Jan. 25 (1):17-27. [QxMD MEDLINE Link] . [Full Text] .
Hedgepeth C III. Discrimination, high blood pressure, and health disparities in African Americans. Harvard Health Blog. Available at https://www.health.harvard.edu/blog/discrimination-high-blood-pressure-and-health-disparities-in-african-americans-2020092120943 . September 21, 2020; Accessed: February 27, 2023.
Ogunniyi MO, Commodore-Mensah Y, Ferdinand KC. Race, ethnicity, hypertension, and heart disease: JACC focus seminar 1/9. J Am Coll Cardiol . 2021 Dec 14. 78 (24):2460-70. [QxMD MEDLINE Link] . [Full Text] .
Williamson L. The link between structural racism, high blood pressure and Black people's health. Heart.org. Available at https://www.heart.org/en/news/2021/04/15/the-link-between-structural-racism-high-blood-pressure-and-black-peoples-health . April 15, 2021; Accessed: February 27, 2024.
Flack JM, Buhnerkempe MG. Race and antihypertensive drug therapy: edging closer to a new paradigm. Hypertension . 2022 Feb. 79 (2):349-51. [QxMD MEDLINE Link] . [Full Text] .
Hajjar I, Kotchen TA. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988-2000. JAMA . 2003 Jul 9. 290(2):199-206. [QxMD MEDLINE Link] .
Bianchi S, Bigazzi R, Campese VM. Microalbuminuria in essential hypertension: significance, pathophysiology, and therapeutic implications. Am J Kidney Dis . 1999 Dec. 34(6):973-95. [QxMD MEDLINE Link] .
Shayne PH, Pitts SR. Severely increased blood pressure in the emergency department. Ann Emerg Med . 2003 Apr. 41(4):513-29. [QxMD MEDLINE Link] .
Rhoades R, Planzer R. Human Physiology . 3rd ed. Fort Worth, TX: Saunders College Publishing; 1996.
Gandhi SK, Powers JC, Nomeir AM, et al. The pathogenesis of acute pulmonary edema associated with hypertension. N Engl J Med . 2001 Jan 4. 344(1):17-22. [QxMD MEDLINE Link] . [Full Text] .
Harrison DG, Coffman TM, Wilcox CS. Pathophysiology of hypertension: the Mosaic Theory and beyond. Circ Res . 2021 Apr 2. 128(7):847-63. [QxMD MEDLINE Link] . [Full Text] .
Hamer M, Steptoe A. Cortisol responses to mental stress and incident hypertension in healthy men and women. J Clin Endocrinol Metab . 2012 Jan. 97(1):E29-34. [QxMD MEDLINE Link] .
Madhur MS, Lob HE, McCann LA, et al. Interleukin 17 promotes angiotensin II-induced hypertension and vascular dysfunction. Hypertension . 2010 Feb. 55(2):500-7. [QxMD MEDLINE Link] . [Full Text] .
Venegas-Pont M, Manigrasso MB, Grifoni SC, et al. Tumor necrosis factor-alpha antagonist etanercept decreases blood pressure and protects the kidney in a mouse model of systemic lupus erythematosus. Hypertension . 2010 Oct. 56(4):643-9. [QxMD MEDLINE Link] . [Full Text] .
Kirabo A, Fontana V, de Faria AP, et al. DC isoketal-modified proteins activate T cells and promote hypertension. J Clin Invest . 2014 Oct. 124(10):4642-56. [QxMD MEDLINE Link] . [Full Text] .
Harrison DG, Guzik TJ, Lob HE, et al. Inflammation, immunity, and hypertension. Hypertension . 2011 Feb. 57(2):132-40. [QxMD MEDLINE Link] . [Full Text] .
Guzik TJ, Hoch NE, Brown KA, et al. Role of the T cell in the genesis of angiotensin II induced hypertension and vascular dysfunction. J Exp Med . 2007 Oct 1. 204(10):2449-60. [QxMD MEDLINE Link] .
Madhur MS, Lob HE, McCann LA, et al. Interleukin 17 promotes angiotensin II-induced hypertension and vascular dysfunction. Hypertension . 2010 Feb. 55(2):500-7. [QxMD MEDLINE Link] .
Rule AD, Fridley BL, Hunt SC, et al. Genome-wide linkage analysis for uric acid in families enriched for hypertension. Nephrol Dial Transplant . 2009 Aug. 24(8):2414-20. [QxMD MEDLINE Link] . [Full Text] .
Jermendy G, Horvath T, Littvay L, et al. Effect of genetic and environmental influences on cardiometabolic risk factors: a twin study. Cardiovasc Diabetol . 2011 Nov 3. 10:96. [QxMD MEDLINE Link] . [Full Text] .
Mitchell GF, DeStefano AL, Larson MG, et al. Heritability and a genome-wide linkage scan for arterial stiffness, wave reflection, and mean arterial pressure: the Framingham Heart Study. Circulation . 2005 Jul 12. 112(2):194-9. [QxMD MEDLINE Link] .
Levy D, DeStefano AL, Larson MG, et al. Evidence for a gene influencing blood pressure on chromosome 17. Genome scan linkage results for longitudinal blood pressure phenotypes in subjects from the framingham heart study. Hypertension . 2000 Oct. 36(4):477-83. [QxMD MEDLINE Link] .
Coffman TM. Under pressure: the search for the essential mechanisms of hypertension. Nat Med . 2011 Nov 7. 17(11):1402-9. [QxMD MEDLINE Link] .
Millis RM. Epigenetics and hypertension. Curr Hypertens Rep . 2011 Feb. 13(1):21-8. [QxMD MEDLINE Link] .
Brown MJ. Hypertension and ethnic group. BMJ . 2006 Apr 8. 332(7545):833-6. [QxMD MEDLINE Link] . [Full Text] .
Goldblatt H, Lynch J, Hanzal RF, Summerville WW. Studies on experimental hypertension: I. The production of persistent elevation of systolic blood pressure by means of renal ischemia. J Exp Med . 1934 Feb 28. 59(3):347-79. [QxMD MEDLINE Link] . [Full Text] .
Carey RM, Calhoun DA, Bakris GL, et al, for the American Heart Association Professional/Public Education and Publications Committee of the Council on Hypertension; Council on Cardiovascular and Stroke Nursing; Council on Clinical Cardiology; et al. Resistant Hypertension: Detection, Evaluation, and Management: A Scientific Statement From the American Heart Association. Hypertension . 2018 Nov. 72(5):e53-e90. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Kapur VK, Auckley DH, Chowdhuri S, et al. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med . 2017 Mar 15. 13(3):479-504. [QxMD MEDLINE Link] . [Full Text] .
Feldstein CA. Blood pressure effects of CPAP in nonresistant and resistant hypertension associated with OSA: A systematic review of randomized clinical trials. Clin Exp Hypertens . 2016. 38(4):337-46. [QxMD MEDLINE Link] .
McEvoy RD, Antic NA, Heeley E, et al, for the SAVE Investigators and Coordinators. CPAP for prevention of cardiovascular events in obstructive sleep apnea. N Engl J Med . 2016 Sep 8. 375(10):919-31. [QxMD MEDLINE Link] . [Full Text] .
Marik PE, Varon J. Hypertensive crises: challenges and management. Chest . 2007 Jun. 131(6):1949-62. [QxMD MEDLINE Link] .
Rodriguez MA, Kumar SK, De Caro M. Hypertensive crisis. Cardiol Rev . 2010 Mar-Apr. 18(2):102-7. [QxMD MEDLINE Link] .
Hollander JE. Cocaine intoxication and hypertension. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S18-20. [QxMD MEDLINE Link] .
Ostchega Y, Fryar CD, Nwankwo T, Nguyen DT. Hypertension prevalence among adults aged 18 and over: United States, 2017-2018. NCHS Data Brief . 2020 Apr. no 364:1-8. [QxMD MEDLINE Link] . [Full Text] .
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J. Global burden of hypertension: analysis of worldwide data. Lancet . 2005 Jan 15-21. 365(9455):217-23. [QxMD MEDLINE Link] .
Forouzanfar MH, Alexander L, Anderson HR, et al, for the GBD 2013 Risk Factors Collaborators. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet . 2015 Dec 5. 386(10010):2287-323. [QxMD MEDLINE Link] . [Full Text] .
GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet . 2015 Jan 10. 385(9963):117-71. [QxMD MEDLINE Link] . [Full Text] .
Saeed A, Dixon DL, Yang E. Racial disparities in hypertension prevalence and management: a crisis control?. American College of Cardiology. Available at https://www.acc.org/Latest-in-Cardiology/Articles/2020/04/06/08/53/Racial-Disparities-in-Hypertension-Prevalence-and-Management . April 6, 2020; Accessed: February 27, 2024.
Mozaffarian D, Benjamin EJ, Go AS, et al, for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics--2015 update: a report from the American Heart Association. Circulation . 2015 Jan 27. 131(4):e29-322. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Carey RM, Calhoun DA, Bakris GL, et al, for the American Heart Association Professional/Public Education and Publications Committee of the Council on Hypertension; Council on Cardiovascular and Stroke Nursing; Council on Clinical Cardiology; et al. Resistant hypertension: detection, evaluation, and management: a scientific statement from the American Heart Association. Hypertension . 2018 Nov. 72(5):e53-e90. [QxMD MEDLINE Link] . [Full Text] .
Ong YT, Wong TY, Klein R, et al. Hypertensive retinopathy and risk of stroke. Hypertension . 2013 Oct. 62(4):706-11. [QxMD MEDLINE Link] . [Full Text] .
Brooks M. Hypertensive retinopathy linked to increased stroke risk. Medscape Medical News. August 16, 2013. Available at https://www.medscape.com/viewarticle/809541 . Accessed: August 20, 2013.
Huang Y, Cai X, Li Y, et al. Prehypertension and the risk of stroke: a meta-analysis. Neurology . 2014 Apr 1. 82(13):1153-61. [QxMD MEDLINE Link] .
Hughes S. Even prehypertension increases stroke risk: meta-analysis. Medscape Medical News. March 14, 2014. Available at https://www.medscape.com/viewarticle/821977 . Accessed: March 20, 2014.
Webster J, Petrie JC, Jeffers TA, Lovell HG. Accelerated hypertension--patterns of mortality and clinical factors affecting outcome in treated patients. Q J Med . 1993 Aug. 86(8):485-93. [QxMD MEDLINE Link] .
Culleton BF, Larson MG, Kannel WB, Levy D. Serum uric acid and risk for cardiovascular disease and death: the Framingham Heart Study. Ann Intern Med . 1999 Jul 6. 131(1):7-13. [QxMD MEDLINE Link] .
Mortality after 10 1/2 years for hypertensive participants in the Multiple Risk Factor Intervention Trial. Circulation . 1990 Nov. 82(5):1616-28. [QxMD MEDLINE Link] .
Chen G, McAlister FA, Walker RL, Hemmelgarn BR, Campbell NR. Cardiovascular outcomes in Framingham participants with diabetes: the importance of blood pressure. Hypertension . 2011 May. 57(5):891-7. [QxMD MEDLINE Link] . [Full Text] .
Ford ES. Trends in mortality from all causes and cardiovascular disease among hypertensive and nonhypertensive adults in the United States. Circulation . 2011 Apr 26. 123(16):1737-44. [QxMD MEDLINE Link] .
Bombelli M, Facchetti R, Sega R, et al. Impact of body mass index and waist circumference on the long-term risk of diabetes mellitus, hypertension, and cardiac organ damage. Hypertension . 2011 Dec. 58(6):1029-35. [QxMD MEDLINE Link] . [Full Text] .
Redon J, Campos C, Narciso ML, Rodicio JL, Pascual JM, Ruilope LM. Prognostic value of ambulatory blood pressure monitoring in refractory hypertension: a prospective study. Hypertension . 1998 Feb. 31(2):712-8. [QxMD MEDLINE Link] . [Full Text] .
Wong TY, Mitchell P. Hypertensive retinopathy. N Engl J Med . 2004 Nov 25. 351(22):2310-7. [QxMD MEDLINE Link] .
Zampaglione B, Pascale C, Marchisio M, Cavallo-Perin P. Hypertensive urgencies and emergencies. Prevalence and clinical presentation. Hypertension . 1996 Jan. 27(1):144-7. [QxMD MEDLINE Link] .
Staykov D, Schwab S. Posterior reversible encephalopathy syndrome. J Intensive Care Med . 2012 Feb. 27(1):11-24. [QxMD MEDLINE Link] .
McCord J, Mundy BJ, Hudson MP, et al, for the Breathing Not Properly Multinational Study Investigators. Relationship between obesity and B-type natriuretic peptide levels. Arch Intern Med . 2004 Nov 8. 164(20):2247-52. [QxMD MEDLINE Link] . [Full Text] .
Mammaro A, Carrara S, Cavaliere A, et al. Hypertensive disorders of pregnancy. J Prenat Med . 2009 Jan. 3(1):1-5. [QxMD MEDLINE Link] . [Full Text] .
Wang IK, Muo CH, Chang YC, et al. Association between hypertensive disorders during pregnancy and end-stage renal disease: a population-based study. CMAJ . 2013 Feb 19. 185(3):207-13. [QxMD MEDLINE Link] . [Full Text] .
American College of Obstetricians and Gynecologists, Task Force on Hypertension in Pregnancy. Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet Gynecol . 2013 Nov. 122(5):1122-31. [QxMD MEDLINE Link] . [Full Text] .
Pickering TG, James GD, Boddie C, Harshfield GA, Blank S, Laragh JH. How common is white coat hypertension?. JAMA . 1988 Jan 8. 259(2):225-8. [QxMD MEDLINE Link] .
Stiles S. Framingham criteria predict new hypertension better than prehypertension in young adults. Medscape Medical News. September 20, 2013. Available at https://www.medscape.com/viewarticle/811416 . Accessed: September 30, 2013.
Carson AP, Lewis CE, Jacobs DR Jr, et al. Evaluating the Framingham hypertension risk prediction model in young adults: the Coronary Artery Risk Development in Young Adults (CARDIA) study. Hypertension . 2013 Dec. 62(6):1015-20. [QxMD MEDLINE Link] . [Full Text] .
Koivistoinen T, Lyytikainen LP, Aatola H, et al. Pulse wave velocity predicts the progression of blood pressure and development of hypertension in young adults. Hypertension . 2018 Mar. 71(3):451-6. [QxMD MEDLINE Link] . [Full Text] .
Olin JW, Piedmonte MR, Young JR, DeAnna S, Grubb M, Childs MB. The utility of duplex ultrasound scanning of the renal arteries for diagnosing significant renal artery stenosis. Ann Intern Med . 1995 Jun 1. 122(11):833-8. [QxMD MEDLINE Link] .
US Food and Drug Administration. Information on gadolinium-based contrast agents. Available at https://www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationforPatientsandProviders/ucm142882.htm . Accessed: February 22, 2012.
American College of Radiology. ACR manual on contrast media, 2023. Available at https://www.acr.org/-/media/ACR/Files/Clinical-Resources/Contrast_Media.pdf . Accessed: March 4, 2024.
Cortigiani L, Bigi R, Landi P, Bovenzi F, Picano E, Sicari R. Prognostic implication of stress echocardiography in 6214 hypertensive and 5328 normotensive patients. Eur Heart J . 2011 Jun. 32(12):1509-18. [QxMD MEDLINE Link] .
[Guideline] Qaseem A, Wilt TJ, Rich R, et al, for the Clinical Guidelines Committee of the American College of Physicians and the Commission on Health of the Public and Science of the American Academy of Family Physicians. Pharmacologic treatment of hypertension in adults aged 60 years or older to higher versus lower blood pressure targets: A clinical practice guideline from the American College of Physicians and the American Academy of Family Physicians. Ann Intern Med . 2017 Mar 21. 166(6):430-7. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] ElSayed NA, Aleppo G, Aroda VR, et al, for the American Diabetes Association. Addendum. 3. Prevention or delay of type 2 diabetes and associated comorbidities: standards of care in diabetes-2023. Diabetes Care . 2023 Sep 1. 46 (9):1716-17. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] ElSayed NA, Aleppo G, Aroda VR, et al, for the American Diabetes Association. Addendum. 2. Classification and diagnosis of diabetes: standards of care in diabetes-2023. Diabetes Care . 2023 Sep 1. 46 (9):1715. [QxMD MEDLINE Link] . [Full Text] .
Redon J, Cifkova R, Laurent S, et al. Mechanisms of hypertension in the cardiometabolic syndrome. J Hypertens . 2009 Mar. 27(3):441-51. [QxMD MEDLINE Link] .
[Guideline] American Diabetes Association. Standards of medical care in diabetes-2016 abridged for primary care providers. Clin Diabetes . 2016 Jan. 34(1):3-21. [QxMD MEDLINE Link] . [Full Text] .
Tseng CD, Yen AM, Chiu SY, Chen LS, Chen HH, Chang SH. A predictive model for risk of prehypertension and hypertension and expected benefit after population-based life-style modification (KCIS No. 24). Am J Hypertens . 2012 Feb. 25(2):171-9. [QxMD MEDLINE Link] .
Stiles S. New AHA/ACC cholesterol treatment guideline expands role of LDL targets. Medscape Medical News. November 10, 2018. Available at https://www.medscape.com/viewarticle/904736 . Accessed: December 1, 2018.
[Guideline] Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol . 2019 Jun 25. 73(24):e285-e350. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation . 2019 Sep 10. 140(11):e596-e646. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Jellinger PS, Handelsman Y, Rosenblit PD, et al. American Association of Clinical Endocrinologists and American College of Endocrinology guidelines for management of dyslipidemia and prevention of cardiovascular disease. Endocr Pract . 2017 Apr. 23(suppl 2):1-87. [QxMD MEDLINE Link] . [Full Text] .
Barbato E, Azizi M, Schmieder RE, et al. Renal denervation in the management of hypertension in adults. A clinical consensus statement of the ESC Council on Hypertension and the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur Heart J . 2023 Apr 17. 44(15):1313-30. [QxMD MEDLINE Link] . [Full Text] .
Forman JP, Scheven L, de Jong PE, Bakker SJ, Curhan GC, Gansevoort RT. Association between sodium intake and change in uric acid, urine albumin excretion, and the risk of developing hypertension. Circulation . 2012 Jun 26. 125(25):3108-16. [QxMD MEDLINE Link] . [Full Text] .
Slagman MC, Waanders F, Hemmelder MH, et al. Moderate dietary sodium restriction added to angiotensin converting enzyme inhibition compared with dual blockade in lowering proteinuria and blood pressure: randomised controlled trial. BMJ . 2011 Jul 26. 343:d4366. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] American Diabetes Association. Standards of medical care in diabetes--2011. Diabetes Care . 2011 Jan. 34 Suppl 1:S11-61. [QxMD MEDLINE Link] . [Full Text] .
Aburto NJ, Hanson S, Gutierrez H, Hooper L, Elliott P, Cappuccio FP. Effect of increased potassium intake on cardiovascular risk factors and disease: systematic review and meta-analyses. BMJ . 2013 Apr 3. 346:f1378. [QxMD MEDLINE Link] . [Full Text] .
Ried K, Sullivan T, Fakler P, Frank OR, Stocks NP. Does chocolate reduce blood pressure? A meta-analysis. BMC Med . 2010 Jun 28. 8:39. [QxMD MEDLINE Link] . [Full Text] .
Salaish Kumar S, Mhd Jalil AM, Hussin N, Mat Daud Z', Ismail A. Effects of flavanols and procyanidins-rich cocoa consumption on metabolic syndrome: an update review (2013 to 2023). Biosci Biotechnol Biochem . 2024 Jan 29. [QxMD MEDLINE Link] . [Full Text] .
Amoah I, Lim JJ, Osei EO, et al. Effect of cocoa beverage and dark chocolate consumption on blood Pressure in Those with Normal and elevated blood pressure: a systematic review and meta-analysis. Foods . 2022 Jul 1. 11 (13):1962. [QxMD MEDLINE Link] . [Full Text] .
Ha V, Sievenpiper JL, de Souza RJ, et al. Effect of fructose on blood pressure: a systematic review and meta-analysis of controlled feeding trials. Hypertension . 2012 Apr. 59(4):787-95. [QxMD MEDLINE Link] . [Full Text] .
Blumenthal JA, Babyak MA, Hinderliter A, et al. Effects of the DASH diet alone and in combination with exercise and weight loss on blood pressure and cardiovascular biomarkers in men and women with high blood pressure: the ENCORE study. Arch Intern Med . 2010 Jan 25. 170(2):126-35. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] de Boer IH, Bangalore S, Benetos A, et al. Diabetes and hypertension: a position statement by the American Diabetes Association. Diabetes Care . 2017 Sep. 40(9):1273-84. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Piercy KL, Troiano RP, Ballard RM, et al. The physical activity guidelines for Americans. JAMA . 2018 Nov 20. 320(19):2020-8. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] 2018 Physical Activity Guidelines Advisory Committee. 2018 Physical Activity Guidelines Advisory Committee Scientific Report . Washington, DC: US Department of Health and Human Services; November 2018. [Full Text] .
Daien V, Duny Y, Ribstein J, et al. Treatment of hypertension with renin-angiotensin system inhibitors and renal dysfunction: a systematic review and meta-analysis. Am J Hypertens . 2012 Jan. 25(1):126-32. [QxMD MEDLINE Link] .
Boggs W. Benazepril plus amlodipine effective for high-risk, stage 2 hypertension. Medscape Medical News. May 3, 2013. Available at https://www.medscape.com/viewarticle/803579 . Accessed: May 8, 2013.
Bakris G, Briasoulis A, Dahlof B, et al, for the ACCOMPLISH Investigators. Comparison of benazepril plus amlodipine or hydrochlorothiazide in high-risk patients with hypertension and coronary artery disease. Am J Cardiol . 2013 Jul 15. 112(2):255-9. [QxMD MEDLINE Link] .
Cushman WC, Evans GW, Byington RP, Goff DC Jr, Grimm RH Jr. Effects of intensive blood-pressure control in type 2 diabetes mellitus. N Engl J Med . 2010 Apr 29. 362(17):1575-85. [QxMD MEDLINE Link] . [Full Text] .
Jamerson K, Weber MA, Bakris GL, et al, for the ACCOMPLISH Trial Investigators. Benazepril plus amlodipine or hydrochlorothiazide for hypertension in high-risk patients. N Engl J Med . 2008 Dec 4. 359(23):2417-28. [QxMD MEDLINE Link] . [Full Text] .
Chrysant SG, Izzo JL Jr, Kereiakes DJ, et al. Efficacy and safety of triple-combination therapy with olmesartan, amlodipine, and hydrochlorothiazide in study participants with hypertension and diabetes: a subpopulation analysis of the TRINITY study. J Am Soc Hypertens . 2012 Mar-Apr. 6(2):132-41. [QxMD MEDLINE Link] .
Ruggenenti P, Lauria G, Iliev IP, et al, for the DEMAND Study Investigators. Effects of manidipine and delapril in hypertensive patients with type 2 diabetes mellitus: the delapril and manidipine for nephroprotection in diabetes (DEMAND) randomized clinical trial. Hypertension . 2011 Nov. 58(5):776-83. [QxMD MEDLINE Link] . [Full Text] .
O'Riordan M. Spironolactone provides benefit in resistant hypertension, small study shows. Medscape Medical News. June 17, 2013. Available at https://www.medscape.com/viewarticle/806388 . Accessed: July 29, 2013.
Tsimihodimos V, Gonzalez-Villalpando C, Meigs JB, Ferrannini E. Hypertension and diabetes mellitus: coprediction and time trajectories. Hypertension . 2018 Mar. 71(3):422-8. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] ElSayed NA, Aleppo G, Aroda VR, et al, on behalf of the American Diabetes Association. 10. Cardiovascular disease and risk management: standards of care in diabetes-2023. Diabetes Care . 2023 Jan 1. 46(Suppl 1):S158-S190. [QxMD MEDLINE Link] . [Full Text] .
Pancioli AM. Hypertension management in neurologic emergencies. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S24-7. [QxMD MEDLINE Link] .
Slovis CM, Reddi AS. Increased blood pressure without evidence of acute end organ damage. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S7-9. [QxMD MEDLINE Link] .
[Guideline] Flynn JT, Kaelber DC, Baker-Smith CM, et al, for the Subcommittee on Screening and Management of High Blood Pressure in Children and Adolescents. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics . 2017 Sep. 140(3): [QxMD MEDLINE Link] . [Full Text] .
Blowey DL, Duda PJ, Stokes P, Hall M. Incidence and treatment of hypertension in the neonatal intensive care unit. J Am Soc Hypertens . 2011 Nov-Dec. 5(6):478-83. [QxMD MEDLINE Link] .
[Guideline] James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA . 2014 Feb 5. 311(5):507-20. [QxMD MEDLINE Link] . [Full Text] .
Wood S. JNC 8 at last! Guidelines ease up on BP thresholds, drug choices. Heartwire from Medscape. December 18, 2013. Available at https://www.medscape.com/viewarticle/817991 . Accessed: December 21, 2013.
Goto Y, Ishii M, Saruta T, et al, for the JATOS Study Group. Principal results of the Japanese trial to assess optimal systolic blood pressure in elderly hypertensive patients (JATOS). Hypertens Res . 2008 Dec. 31(12):2115-27. [QxMD MEDLINE Link] .
Ogihara T, Saruta T, Rakugi H, et al, for the Valsartan in Elderly Isolated Systolic Hypertension Study Group. Target blood pressure for treatment of isolated systolic hypertension in the elderly: valsartan in elderly isolated systolic hypertension study. Hypertension . 2010 Aug. 56(2):196-202. [QxMD MEDLINE Link] . [Full Text] .
Williamson JD, Supiano MA, Applegate WB, et al, for the SPRINT Research Group. Intensive vs standard blood pressure control and cardiovascular disease outcomes in adults aged ≥75 years: a randomized clinical trial. JAMA . 2016 Jun 28. 315(24):2673-82. [QxMD MEDLINE Link] . [Full Text] .
Kostis JB, Cabrera J, Cheng JQ, et al. Association between chlorthalidone treatment of systolic hypertension and long-term survival. JAMA . 2011 Dec 21. 306(23):2588-93. [QxMD MEDLINE Link] . [Full Text] .
Staessen JA, Fagard R, Thijs L, et al. Randomised double-blind comparison of placebo and active treatment for older patients with isolated systolic hypertension. The Systolic Hypertension in Europe (Syst-Eur) Trial Investigators. Lancet . 1997 Sep 13. 350(9080):757-64. [QxMD MEDLINE Link] .
Cooper CJ, Murphy TP, Cutlip DE, et al, for the CORAL Investigators. Stenting and medical therapy for atherosclerotic renal-artery stenosis. N Engl J Med . 2014 Jan 2. 370(1):13-22. [QxMD MEDLINE Link] . [Full Text] .
Calhoun DA. Advances in resistant hypertension. Ann Transl Med . 2018 Aug. 6(15):294. [QxMD MEDLINE Link] . [Full Text] .
Nishizaka MK, Zaman MA, Calhoun DA. Efficacy of low-dose spironolactone in subjects with resistant hypertension. Am J Hypertens . 2003 Nov. 16(11 Pt 1):925-30. [QxMD MEDLINE Link] .
de la Sierra A, Segura J, Banegas JR, et al. Clinical features of 8295 patients with resistant hypertension classified on the basis of ambulatory blood pressure monitoring. Hypertension . 2011 May. 57(5):898-902. [QxMD MEDLINE Link] . [Full Text] .
Townsend RR, Epstein M. Resistant hypertension: insights on evaluation and management in the post-SPRINT (Systolic Blood Pressure Intervention Trial) era. Hypertension . 2016 Nov. 68(5):1073-80. [QxMD MEDLINE Link] . [Full Text] .
Idorsia Pharmaceuticals. US FDA approves Idorsia’s once-daily TRYVIO (aprocitentan) – the first and only endothelin receptor antagonist for the treatment of high blood pressure not adequately controlled in combination with other antihypertensives [news release]. Available at https://www.idorsia.com/media/news/news-archive/media-release-details?id=3195250 . March 20, 2024; Accessed: March 20, 2024.
Brooks M. FDA okays new drug for resistant hypertension. Medscape Medical News. Available at https://www.medscape.com/viewarticle/fda-okays-new-drug-resistant-hypertension-2024a100058b . March 20, 2024; Accessed: March 20, 2024.
Schlaich MP, Bellet M, Weber MA, et al, for the PRECISION investigators. Dual endothelin antagonist aprocitentan for resistant hypertension (PRECISION): a multicentre, blinded, randomised, parallel-group, phase 3 trial. Lancet . 2022 Dec 3. 400 (10367):1927-37. [QxMD MEDLINE Link] .
Orciari Herman A, Sadoughi S. Heart group updates guidelines on resistant hypertension. NEJM Journal Watch. September 13, 2018. Available at https://www.jwatch.org/fw114569/2018/09/13/heart-group-updates-guidelines-resistant-hypertension . Accessed: October 2, 2018.
Krum H, Schlaich M, Whitbourn R, et al. Catheter-based renal sympathetic denervation for resistant hypertension: a multicentre safety and proof-of-principle cohort study. Lancet . 2009 Apr 11. 373(9671):1275-81. [QxMD MEDLINE Link] .
Catheter-based renal sympathetic denervation for resistant hypertension: durability of blood pressure reduction out to 24 months. Hypertension . 2011 May. 57(5):911-7. [QxMD MEDLINE Link] .
Esler MD, Krum H, Sobotka PA, et al. Renal sympathetic denervation in patients with treatment-resistant hypertension (The Symplicity HTN-2 Trial): a randomised controlled trial. Lancet . 2010 Dec 4. 376(9756):1903-9. [QxMD MEDLINE Link] .
Bhatt DL, Kandzari DE, O'Neill WW, et al, for the SYMPLICITY HTN-3 Investigators. A controlled trial of renal denervation for resistant hypertension. N Engl J Med . 2014 Apr 10. 370(15):1393-401. [QxMD MEDLINE Link] . [Full Text] .
Azizi M, Sanghvi K, Saxena M, et al, for the RADIANCE-HTN investigators. Ultrasound renal denervation for hypertension resistant to a triple medication pill (RADIANCE-HTN TRIO): a randomised, multicentre, single-blind, sham-controlled trial. Lancet . 2021 Jun 26. 397(10293):2476-86. [QxMD MEDLINE Link] .
Azizi M, Saxena M, Wang Y, et al, for the RADIANCE II Investigators and Collaborators. Endovascular ultrasound renal denervation to treat hypertension: the RADIANCE II randomized clinical trial. JAMA . 2023 Feb 28. 329(8):651-61. [QxMD MEDLINE Link] . [Full Text] .
Bohm M, Kario K, Kandzari DE, et al, for the SPYRAL HTN-OFF MED Pivotal Investigators. Efficacy of catheter-based renal denervation in the absence of antihypertensive medications (SPYRAL HTN-OFF MED Pivotal): a multicentre, randomised, sham-controlled trial. Lancet . 2020 May 2. 395(10234):1444-51. [QxMD MEDLINE Link] .
Mahfoud F, Kandzari DE, Kario K, et al. Long-term efficacy and safety of renal denervation in the presence of antihypertensive drugs (SPYRAL HTN-ON MED): a randomised, sham-controlled trial. Lancet . 2022 Apr 9. 399(10333):1401-10. [QxMD MEDLINE Link] .
Bisognano JD, Bakris G, Nadim MK, et al. Baroreflex activation therapy lowers blood pressure in patients with resistant hypertension: results from the double-blind, randomized, placebo-controlled rheos pivotal trial. J Am Coll Cardiol . 2011 Aug 9. 58(7):765-73. [QxMD MEDLINE Link] . [Full Text] .
de La Sierra A, Larrousse M, Oliveras A, et al. Abnormalities of vascular function in resistant hypertension. Blood Press . 2012 Apr. 21(2):104-9. [QxMD MEDLINE Link] . [Full Text] .
Mariampillai JE, Eskas PA, Heimark S, et al. Apparent treatment-resistant hypertension - patient-physician relationship and ethical issues. Blood Press . 2017 Jun. 26(3):133-8. [QxMD MEDLINE Link] .
Kronish IM, Woodward M, Sergie Z, Ogedegbe G, Falzon L, Mann DM. Meta-analysis: impact of drug class on adherence to antihypertensives. Circulation . 2011 Apr 19. 123(15):1611-21. [QxMD MEDLINE Link] . [Full Text] .
Fagugli RM, Taglioni C. Changes in the perceived epidemiology of primary hyperaldosteronism. Int J Hypertens . 2011. 2011:162804. [QxMD MEDLINE Link] . [Full Text] .
Pedrosa RP, Drager LF, Gonzaga CC, et al. Obstructive sleep apnea: the most common secondary cause of hypertension associated with resistant hypertension. Hypertension . 2011 Nov. 58(5):811-7. [QxMD MEDLINE Link] . [Full Text] .
Martinez-Garcia MA, Capote F, Campos-Rodriguez F, et al, for the Spanish Sleep Network. Effect of CPAP on blood pressure in patients with obstructive sleep apnea and resistant hypertension: the HIPARCO randomized clinical trial. JAMA . 2013 Dec 11. 310(22):2407-15. [QxMD MEDLINE Link] . [Full Text] .
O'Riordan M. CPAP reduces blood pressure in resistant hypertension. Heartwire from Medscape. December 10, 2013. Available at https://www.medscape.com/viewarticle/817569 . Accessed: December 16, 2013.
Fahey T, Schroeder K, Ebrahim S. Interventions used to improve control of blood pressure in patients with hypertension. Cochrane Database Syst Rev . 2006 Apr 19. CD005182. [QxMD MEDLINE Link] . [Full Text] .
Pezzin LE, Feldman PH, Mongoven JM, McDonald MV, Gerber LM, Peng TR. Improving blood pressure control: results of home-based post-acute care interventions. J Gen Intern Med . 2011 Mar. 26(3):280-6. [QxMD MEDLINE Link] . [Full Text] .
Glynn LG, Murphy AW, Smith SM, Schroeder K, Fahey T. Interventions used to improve control of blood pressure in patients with hypertension. Cochrane Database Syst Rev . 2010 Mar 17. CD005182. [QxMD MEDLINE Link] . [Full Text] .
Bosworth HB, Powers BJ, Olsen MK, et al. Home blood pressure management and improved blood pressure control: results from a randomized controlled trial. Arch Intern Med . 2011 Jul 11. 171(13):1173-80. [QxMD MEDLINE Link] . [Full Text] .
O'Riordan M. New European hypertension guidelines released: goal is less than 140 mm Hg for all. Heartwire from Medscape. June 15, 2013. Available at https://www.medscape.com/viewarticle/806367 . Accessed: June 24, 2013.
[Guideline] Mancia G, Fagard R, Narkiewicz K, et al, for the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension and the European Society of Cardiology. 2013 ESH/ESC practice guidelines for the management of arterial hypertension. Blood Press . 2014 Feb. 23(1):3-16. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Krist AH, Davidson KW, Mangione CM, et al, for the US Preventive Services Task Force. Screening for hypertension in adults: US Preventive Services Task Force reaffirmation recommendation statement. JAMA . 2021 Apr 27. 325(16):1650-6. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] American Congress of Obstetricians and Gynecologists (ACOG). Well-woman care: assessments & recommendations. Washington, DC: American Congress of Obstetricians and Gynecologists. Available at https://www.acog.org/About-ACOG/ACOG-Departments/Annual-Womens-Health-Care/Well-Woman-Recommendations . 2013; Accessed: May 15, 2016.
[Guideline] Department of Veterans Affairs and Department of Defense (VA/DoD). Clinical practice guideline for the diagnosis and management of hypertension in the primary care setting. Version 3.0. Available at https://www.healthquality.va.gov/guidelines/CD/htn/VADoDCPGfortheManagementofHTN.pdf . 2014; Accessed: May 15, 2016.
[Guideline] Rosendorff C, Lackland DT, Allison M, Aronow WS, et al, for the American Heart Association, et al. Treatment of hypertension in patients with coronary artery disease: a scientific statement from the American Heart Association, American College of Cardiology, and American Society of Hypertension. Circulation . 2015 May 12. 131(19):e435-70. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Go AS, Bauman MA, Coleman King SM, et al, for the American Heart Association, American College of Cardiology, et al. An effective approach to high blood pressure control: a science advisory from the American Heart Association, the American College of Cardiology, and the Centers for Disease Control and Prevention. Hypertension . 2014 Apr. 63(4):878-85. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Weber MA, Schiffrin EL, White WB, et al. Clinical practice guidelines for the management of hypertension in the community a statement by the American Society of Hypertension and the International Society of Hypertension. J Hypertens . 2014 Jan. 32(1):3-15. [QxMD MEDLINE Link] . [Full Text] .
Wright JT Jr, Williamson JD, Whelton PK, et al, for the SPRINT Research Group. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med . 2015 Nov 26. 373(22):2103-16. [QxMD MEDLINE Link] . [Full Text] .
Benavente OR, Coffey CS, Conwit R, et al, for the SPS3 Study Group. Blood-pressure targets in patients with recent lacunar stroke: the SPS3 randomised trial. Lancet . 2013 Aug 10. 382(9891):507-15. [QxMD MEDLINE Link] . [Full Text] .
Oparil S, Lewis CE. Should patients with cardiovascular risk factors receive intensive treatment of hypertension to Circulation</i>. 2016 Nov 1. 134(18):1308-1310. [QxMD MEDLINE Link] . [Full Text] .
Thomopoulos C, Parati G, Zanchetti A. Effects of blood pressure lowering on outcome incidence in hypertension: 7. Effects of more vs. less intensive blood pressure lowering and different achieved blood pressure levels - updated overview and meta-analyses of randomized trials. J Hypertens . 2016 Apr. 34(4):613-22. [QxMD MEDLINE Link] .
O'Riordan M. AHA/ACC/CDC issue 'science advisory' on treating BP. Medscape Medical News. November 15, 2013. Available at https://www.medscape.com/viewarticle/814442 . Accessed: November 16, 2013.
[Guideline] Magee LA, Pels A, Helewa M, Rey E, von Dadelszen P, Canadian Hypertensive Disorders of Pregnancy Working Group. Diagnosis, evaluation, and management of the hypertensive disorders of pregnancy: executive summary. J Obstet Gynaecol Can . 2014 May. 36(5):416-41. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Goldstein LB, Bushnell CD, Adams RJ, et al, for the American Heart Association Stroke Council, Council on Cardiovascular Nursing, et al. Guidelines for the primary prevention of stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke . 2011 Feb. 42(2):517-84. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Wolf SJ, Lo B, Shih RD, Smith MD, Fesmire FM; American College of Emergency Physicians Clinical Policies Committee. Clinical policy: critical issues in the evaluation and management of adult patients in the emergency department with asymptomatic elevated blood pressure. Ann Emerg Med . 2013 Jul. 62(1):59-68. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] National High Blood Pressure Education Program Working Group. Report of the National High Blood Pressure Education Program Working Group on high blood pressure in pregnancy. Am J Obstet Gynecol . 2000 Jul. 183(1):S1-S22. [QxMD MEDLINE Link] .
[Guideline] American College of Obstetricians and Gynecologists, Task Force on Hypertension in Pregnancy. Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet Gynecol . 2013 Nov. 122(5):1122-31. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Committee on Obstetric Practice. Committee opinion no. 623: emergent therapy for acute-onset, severe hypertension during pregnancy and the postpartum period. Obstet Gynecol . 2015 Feb. 125(2):521-5. [QxMD MEDLINE Link] . [Full Text] .
Leung AA, Wright A, Pazo V, Karson A, Bates DW. Risk of thiazide-induced hyponatremia in patients with hypertension. Am J Med . 2011 Nov. 124(11):1064-72. [QxMD MEDLINE Link] .
Harel Z, Gilbert C, Wald R, et al. The effect of combination treatment with aliskiren and blockers of the renin-angiotensin system on hyperkalaemia and acute kidney injury: systematic review and meta-analysis. BMJ . 2012 Jan 9. 344:e42. [QxMD MEDLINE Link] . [Full Text] .
Cummings DM, Amadio P Jr, Nelson L, Fitzgerald JM. The role of calcium channel blockers in the treatment of essential hypertension. Arch Intern Med . 1991 Feb. 151(2):250-9. [QxMD MEDLINE Link] .
Fryar CD, Ostchega Y, Hales CM, Zhang G, Kruszon-Moran D. Hypertension prevalence and control among adults: United States, 2015-2016. NCHS Data Brief . 2017 Oct. 1-8. [QxMD MEDLINE Link] . [Full Text] .
Stowasser M, Gordon RD. Primary aldosteronism: changing definitions and new concepts of physiology and pathophysiology both inside and outside the kidney. Physiol Rev . 2016 Oct. 96(4):1327-84. [QxMD MEDLINE Link] . [Full Text] .
Briasoulis A, Bakris GL. Current status of renal denervation in hypertension. Curr Cardiol Rep . 2016 Nov. 18(11):107. [QxMD MEDLINE Link] .
Frellick M. Updated hypertension guidelines released by ACP, AAFP. Medscape Medical News. January 17, 2017. Available at https://www.medscape.com/viewarticle/874494 . Accessed: November 18, 2017.
Weinberger MH, Izzo JL Jr, Purkayastha D, Weitzman R, Black HR. Comparative efficacy and safety of combination aliskiren/amlodipine and amlodipine monotherapy in African Americans with stage 2 hypertension and obesity or metabolic syndrome. J Am Soc Hypertens . 2011 Nov-Dec. 5(6):489-97. [QxMD MEDLINE Link] .
Denker MG, Cohen DL, Townsend RR. Catheter-based renal artery denervation for resistant hypertension: promise unfulfilled or unsettled?. Curr Atheroscler Rep . 2015 Oct. 17(10):535. [QxMD MEDLINE Link] .
Qureshi AI, Suri MF, Kirmani JF, Divani AA. Prevalence and trends of prehypertension and hypertension in United States: National Health and Nutrition Examination Surveys 1976 to 2000. Med Sci Monit . 2005 Sep. 11(9):CR403-9. [QxMD MEDLINE Link] .
Cornoni-Huntley J, LaCroix AZ, Havlik RJ. Race and sex differentials in the impact of hypertension in the United States. The National Health and Nutrition Examination Survey I Epidemiologic Follow-up Study. Arch Intern Med . 1989 Apr. 149(4):780-8. [QxMD MEDLINE Link] .
Strong Heart Study Data Book: A Report to American Indian Communities . Bethesda, MD: National Heart, Lung, and Blood Institute, NIH; 2001.
Grundy SM, Cleeman JI, Daniels SR, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation . 2005 Oct 25. 112(17):2735-52. [QxMD MEDLINE Link] .
Aronow WS, Fleg JL, Pepine CJ, et al. ACCF/AHA 2011 expert consensus document on hypertension in the elderly: a report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus documents developed in collaboration with the American Academy of Neurology, American Geriatrics Society, American Society for Preventive Cardiology, American Society of Hypertension, American Society of Nephrology, Association of Black Cardiologists, and European Society of Hypertension. J Am Coll Cardiol . 2011 May 17. 57(20):2037-114. [QxMD MEDLINE Link] . [Full Text] .
[Guideline] Guidelines Subcommittee. 1999 World Health Organization-International Society of Hypertension guidelines for the management of hypertension. J Hypertens . 1999 Feb. 17(2):151-83. [QxMD MEDLINE Link] .
Abalos E, Duley L, Steyn DW, Henderson-Smart DJ. Antihypertensive drug therapy for mild to moderate hypertension during pregnancy. Cochrane Database Syst Rev . 2007 Jan 24. CD002252. [QxMD MEDLINE Link] .
Abergel E, Chatellier G, Battaglia C, Menard J. Can echocardiography identify mildly hypertensive patients at high risk, left untreated based on current guidelines?. J Hypertens . 1999 Jun. 17(6):817-24. [QxMD MEDLINE Link] .
Matchar DB, McCrory DC, Orlando LA, et al. Systematic review: comparative effectiveness of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers for treating essential hypertension. Ann Intern Med . 2008 Jan 1. 148(1):16-29. [QxMD MEDLINE Link] . [Full Text] .
ACR Committee on Drugs and Contrast Media. ACR Manual on Contrast Media. Vers. 7. American College of Radiology. 2023. Available at https://www.acr.org/-/media/ACR/Files/Clinical-Resources/Contrast_Media.pdf .
Anderson CS, Huang Y, Arima H, et al, for the INTERACT Investigators. Effects of early intensive blood pressure-lowering treatment on the growth of hematoma and perihematomal edema in acute intracerebral hemorrhage: the Intensive Blood Pressure Reduction in Acute Cerebral Haemorrhage Trial (INTERACT). Stroke . 2010 Feb. 41(2):307-12. [QxMD MEDLINE Link] . [Full Text] .
Anderson CS, Huang Y, Wang JG, et al, for the INTERACT Investigators. Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomised pilot trial. Lancet Neurol . 2008 May. 7(5):391-9. [QxMD MEDLINE Link] .
Ault MJ, Ellrodt AG. Pathophysiological events leading to the end-organ effects of acute hypertension. Am J Emerg Med . 1985 Dec. 3(6 Suppl):10-5. [QxMD MEDLINE Link] .
Barton JR. Hypertension in pregnancy. Ann Emerg Med . 2008 Mar. 51 (3 suppl):S16-7. [QxMD MEDLINE Link] .
Brown MJ, McInnes GT, Papst CC, Zhang J, MacDonald TM. Aliskiren and the calcium channel blocker amlodipine combination as an initial treatment strategy for hypertension control (ACCELERATE): a randomised, parallel-group trial. Lancet . 2011 Jan 22. 377(9762):312-20. [QxMD MEDLINE Link] .
Chapman N, Huxley R, Anderson C, et al, for the Writing Committee for the PROGRESS Collaborative Group. Effects of a perindopril-based blood pressure-lowering regimen on the risk of recurrent stroke according to stroke subtype and medical history: the PROGRESS Trial. Stroke . 2004 Jan. 35(1):116-21. [QxMD MEDLINE Link] . [Full Text] .
Cheung AT, Hobson RW 2nd. Hypertension in vascular surgery: aortic dissection and carotid revascularization. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S28-33. [QxMD MEDLINE Link] .
Chrysant SG, Fagan T, Glazer R, Kriegman A. Effects of benazepril and hydrochlorothiazide, given alone and in low- and high-dose combinations, on blood pressure in patients with hypertension. Arch Fam Med . 1996 Jan. 5(1):17-24; discussion 25. [QxMD MEDLINE Link] .
Cushman WC, Bakris GL, White WB, et al. Azilsartan medoxomil plus chlorthalidone reduces blood pressure more effectively than olmesartan plus hydrochlorothiazide in stage 2 systolic hypertension. Hypertension . 2012 Aug. 60(2):310-8. [QxMD MEDLINE Link] . [Full Text] .
Diercks DB, Ohman EM. Hypertension with acute coronary syndrome and heart failure. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S34-6. [QxMD MEDLINE Link] .
Dungan JR, Conley YP, Langaee TY, et al. Altered beta-2 adrenergic receptor gene expression in human clinical hypertension. Biol Res Nurs . 2009 Jul. 11(1):17-26. [QxMD MEDLINE Link] . [Full Text] .
Epstein M. Calcium antagonists and renal disease. Kidney Int . 1998 Nov. 54(5):1771-84. [QxMD MEDLINE Link] .
Faselis C, Doumas M, Kokkinos JP, et al. Exercise capacity and progression from prehypertension to hypertension. Hypertension . 2012 Aug. 60(2):333-8. [QxMD MEDLINE Link] . [Full Text] .
Hansson L, Hedner T, Lund-Johansen P, et al. Randomised trial of effects of calcium antagonists compared with diuretics and beta-blockers on cardiovascular morbidity and mortality in hypertension: the Nordic Diltiazem (NORDIL) study. Lancet . 2000 Jul 29. 356(9227):359-65. [QxMD MEDLINE Link] . [Full Text] .
Heilpern K. Pathophysiology of hypertension. Ann Emerg Med . 2008 Mar. 51(3 Suppl):S5-6. [QxMD MEDLINE Link] .
Hermida RC, Ayala DE, Mojon A, Fernandez JR. Decreasing sleep-time blood pressure determined by ambulatory monitoring reduces cardiovascular risk. J Am Coll Cardiol . 2011 Sep 6. 58(11):1165-73. [QxMD MEDLINE Link] . [Full Text] .
Izzo JL Jr, Weintraub HS, Duprez DA, et al. Treating systolic hypertension in the very elderly with valsartan-hydrochlorothiazide vs. either monotherapy: ValVET primary results. J Clin Hypertens (Greenwich) . 2011 Oct. 13(10):722-30. [QxMD MEDLINE Link] . [Full Text] .
Kandzari DE, Bhatt DL, Sobotka PA, et al. Catheter-based renal denervation for resistant hypertension: rationale and design of the SYMPLICITY HTN-3 Trial. Clin Cardiol . 2012 Sep. 35(9):528-35. [QxMD MEDLINE Link] . [Full Text] .
Kaplan NM. Calcium entry blockers in the treatment of hypertension. Current status and future prospects. JAMA . 1989 Aug 11. 262(6):817-23. [QxMD MEDLINE Link] .
[Guideline] Khan NA, McAlister FA, Lewanczuk RZ, et al, for the Canadian Hypertension Education Program. The 2005 Canadian Hypertension Education Program recommendations for the management of hypertension: part II - therapy. Can J Cardiol . 2005 Jun. 21(8):657-72. [QxMD MEDLINE Link] .
Kitiyakara C, Guzman NJ. Malignant hypertension and hypertensive emergencies. J Am Soc Nephrol . 1998 Jan. 9(1):133-42. [QxMD MEDLINE Link] .
Lao D, Parasher PS, Cho KC, Yeghiazarians Y. Atherosclerotic renal artery stenosis--diagnosis and treatment. Mayo Clin Proc . 2011 Jul. 86(7):649-57. [QxMD MEDLINE Link] . [Full Text] .
Lloyd-Jones D, Adams RJ, Brown TM, et al, for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics--2010 update: a report from the American Heart Association. Circulation . 2010 Feb 23. 121(7):e46-e215. [QxMD MEDLINE Link] . [Full Text] .
Magee LA, Helewa M, Rey E, Hypertension Guidelines Committee, Strategic Training Initiative in Research in the Reproductive Health Sciences (STIRRHS) Scholars. Diagnosis, evaluation, and management of the hypertensive disorders of pregnancy. J Obstet Gynaecol Can . 2008 Mar. 30(3 Suppl):S1-S2. [QxMD MEDLINE Link] .
Furberg CD, Wright JT, Davis BR, et al, for the The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major cardiovascular events in hypertensive patients randomized to doxazosin vs chlorthalidone: the antihypertensive and lipid-lowering treatment to prevent heart attack trial (ALLHAT). ALLHAT Collaborative Research Group. JAMA . 2000 Apr 19. 283(15):1967-75. [QxMD MEDLINE Link] . [Full Text] .
Narkiewicz K. Diagnosis and management of hypertension in obesity. Obes Rev . 2006 May. 7(2):155-62. [QxMD MEDLINE Link] .
National Institutes of Health. Your guide to lowering your blood pressure with DASH. National Heart, Lung, and Blood Institute. April 2006. Available at https://www.nhlbi.nih.gov/health/public/heart/hbp/dash/new_dash.pdf .
Novartis announces termination of ALTITUDE study with Rasilez/Tekturna in high-risk patients with diabetes and renal impairment [press release]. FiercePharma. December 20, 2011. Available at https://www.fiercepharma.com/pharma/novartis-announces-termination-of-altitude-study-rasilez%C2%AE-tekturna%C2%AE-high-risk-patients . Accessed: February 22, 2012.
O'Connor PJ, Vazquez-Benitez G, Schmittdiel JA, et al. Benefits of early hypertension control on cardiovascular outcomes in patients with diabetes. Diabetes Care . 2013 Feb. 36(2):322-7. [QxMD MEDLINE Link] . [Full Text] .
O'Riordan M. Olmesartan label to include intestinal problems, FDA says. Medscape Medical News. July 3, 2013. Available at https://www.medscape.com/viewarticle/807289 . Accessed: July 8, 2013.
Pimenta E, Calhoun DA, Oparil S. Sleep apnea, aldosterone, and resistant hypertension. Prog Cardiovasc Dis . 2009 Mar-Apr. 51(5):371-80. [QxMD MEDLINE Link] .
Pleis JR, Lucas JW, Ward BW. Summary health statistics for U.S. adults: National Health Interview Survey, 2008. Vital Health Stat 10 . 2009 Dec. No. 242:1-157. [QxMD MEDLINE Link] . [Full Text] .
Podymow T, August P. Antihypertensive drugs in pregnancy. Semin Nephrol . 2011 Jan. 31(1):70-85. [QxMD MEDLINE Link] .
Pollare T, Lithell H, Berne C. A comparison of the effects of hydrochlorothiazide and captopril on glucose and lipid metabolism in patients with hypertension. N Engl J Med . 1989 Sep 28. 321(13):868-73. [QxMD MEDLINE Link] .
Rastan A, Krankenberg H, Muller-Hulsbeck S, et al. Improved renal function and blood pressure control following renal artery angioplasty: the renal artery angioplasty in patients with renal insufficiency and hypertension using a dedicated renal stent device study (PRECISION). EuroIntervention . 2008 Aug. 4(2):208-13. [QxMD MEDLINE Link] .
Roberts CL, Ford JB, Algert CS, et al. Population-based trends in pregnancy hypertension and pre-eclampsia: an international comparative study. BMJ Open . 2011 May 24. 1(1):e000101. [QxMD MEDLINE Link] . [Full Text] .
Shook RP, Lee DC, Sui X, et al. Cardiorespiratory fitness reduces the risk of incident hypertension associated with a parental history of hypertension. Hypertension . 2012 Jun. 59(6):1220-4. [QxMD MEDLINE Link] . [Full Text] .
Svetkey LP, Moore TJ, Simons-Morton DG, et al, for the DASH collaborative research group. Angiotensinogen genotype and blood pressure response in the Dietary Approaches to Stop Hypertension (DASH) study. J Hypertens . 2001 Nov. 19(11):1949-56. [QxMD MEDLINE Link] .
Taubert D, Roesen R, Lehmann C, Jung N, Schomig E. Effects of low habitual cocoa intake on blood pressure and bioactive nitric oxide: a randomized controlled trial. JAMA . 2007 Jul 4. 298(1):49-60. [QxMD MEDLINE Link] .
World Health Organization. The World Health Report 2002 - reducing risks, promoting healthy life. Geneva, Switzerland: WHO; 2002. Available at https://www.who.int/whr/2002/en/ . Accessed: February 20, 2012.
Tymchak W, Armstrong PW, Westerhout CM, et al. Mode of hospital presentation in patients with non-ST-elevation myocardial infarction: implications for strategic management. Am Heart J . 2011 Sep. 162(3):436-43. [QxMD MEDLINE Link] .
Wallach R, Karp RB, Reves JG, Oparil S, Smith LR, James TN. Pathogenesis of paroxysmal hypertension developing during and after coronary bypass surgery: a study of hemodynamic and humoral factors. Am J Cardiol . 1980 Oct. 46(4):559-65. [QxMD MEDLINE Link] .
White WB, Weber MA, Sica D, et al. Effects of the angiotensin receptor blocker azilsartan medoxomil versus olmesartan and valsartan on ambulatory and clinic blood pressure in patients with stages 1 and 2 hypertension. Hypertension . 2011 Mar. 57(3):413-20. [QxMD MEDLINE Link] . [Full Text] .
Wolz M, Cutler J, Roccella EJ, Rohde F, Thom T, Burt V. Statement from the National High Blood Pressure Education Program: prevalence of hypertension. Am J Hypertens . 2000 Jan. 13(1 Pt 1):103-4. [QxMD MEDLINE Link] .
Yakovlevitch M, Black HR. Resistant hypertension in a tertiary care clinic. Arch Intern Med . 1991 Sep. 151(9):1786-92. [QxMD MEDLINE Link] .
Dolan E, O'Brien E. Is it daily, monthly, or yearly blood pressure variability that enhances cardiovascular risk?. Curr Cardiol Rep . 2015 Nov. 17(11):93. [QxMD MEDLINE Link] .
Cau SB, Guimaraes DA, Rizzi E, Ceron CS, Gerlach RF, Tanus-Santos JE. The nuclear factor kappaB inhibitor pyrrolidine dithiocarbamate prevents cardiac remodelling and matrix metalloproteinase-2 up-regulation in renovascular hypertension. Basic Clin Pharmacol Toxicol . 2015 Oct. 117(4):234-41. [QxMD MEDLINE Link] . [Full Text] .
Rosner B, Cook NR, Daniels S, Falkner B. Childhood blood pressure trends and risk factors for high blood pressure: the NHANES experience 1988-2008. Hypertension . 2013 Aug. 62(2):247-54. [QxMD MEDLINE Link] . [Full Text] .
Alam T, Khan S, Gaba B, Haider MF, Baboota S, Ali J. Nanocarriers as treatment modalities for hypertension. Drug Deliv . 2017 Nov. 24(1):358-69. [QxMD MEDLINE Link] . [Full Text] .
Marcuccilli M, Kendrick J, Chonchol M. Sodium and fluid management in the conservative management of chronic kidney disease. Panminerva Med . 2017 Jun. 59(2):116-23. [QxMD MEDLINE Link] .
Clinical implications: hypertension. Hypertension . 2018 Mar 1. 71(3):367. [Full Text] .
Osborn JW, Banek CT. Catheter-based renal nerve ablation as a novel hypertension therapy: lost, and then found, in translation. Hypertension . 2018 Mar. 71(3):383-88. [QxMD MEDLINE Link] . [Full Text] .
Itoh H, Hayashi K, Miyashita K. Pre-emptive medicine for hypertension and its prospects. Hypertens Res . 2019 Mar. 42(3):301-5. [QxMD MEDLINE Link] .
Vemu PL, Yang E, Ebinger J. 2023 ESH hypertension guideline update: bringing us closer together across the pond. American College of Cardiology. Available at https://www.acc.org/Latest-in-Cardiology/Articles/2024/02/05/11/43/2023-ESH-Hypertension-Guideline-Update . February 5, 2024; Accessed: February 27, 2024.
Whelton PK, Carey RM, Mancia G, Kreutz R, Bundy JD, Williams B. Harmonization of the American College of Cardiology/American Heart Association and European Society of Cardiology/European Society of Hypertension blood pressure/hypertension guidelines: comparisons, reflections, and recommendations. Circulation . 2022 Sep 13. 146 (11):868-77. [QxMD MEDLINE Link] . [Full Text] .
- Hypertension. Anteroposterior x-ray from a 28-year old woman who presented with congestive heart failure secondary to her chronic hypertension, or high blood pressure. The enlarged cardiac silhouette on this image is due to congestive heart failure due to the effects of chronic high blood pressure on the left ventricle. The heart then becomes enlarged, and fluid accumulates in the lungs, known as pulmonary congestion.
- Hypertension. Electrocardiogram (ECG) from a 47-year-old man with a long-standing history of uncontrolled hypertension. This image shows left atrial enlargement and left ventricular hypertrophy.
- Hypertension. Electrocardiogram (ECG) from a 46-year-old man with long-standing hypertension. This ECG shows left atrial abnormality and left ventricular hypertrophy with strain.
- Hypertension. Hypertrophied cardiac myocytes with enlarged "box car" nuclei.
- Hypertension. Prevalence of hypertension among adults aged 18 and older, by sex and age: United States, 2017-2018. Courtesy of the Centers for Disease Control and Prevention (CDC), National Center for Health Statistics (NCHS).
- Hypertension. Age-adjusted trends in hypertension among adults aged 18 and older: United States, 1999–2018. Courtesy of the Centers for Disease Control and Prevention (CDC), National Center for Health Statistics (NCHS).
- Table 2. NHIS/NCHS Age-Adjusted Prevalence Estimates in Individuals Aged 18 Years and Older in 2015.
- Table 2. Identifiable Hypertension and Screening Tests
- Table 3. Hypertensive Disorders in Pregnancy
- Table 4. Guidelines for Blood Pressure Screening in Adults
- Table 5. Target Blood Pressure Recommendations
- Table 6. American Society of Hypertension/International Society of Hypertension Treatment Recommendations
- Table 7. JNC 7 Classification of Hypertensive Disorders in Pregnancy
Race/Ethnic Group | Have Hypertension, % | Have Heart Disease, % | Have Coronary Heart Disease, % | Have Had a Stroke, % |
White only | 23.8 | 11.3 | 5.6 | 2.4 |
Black/African American | 34.4 | 9.5 | 5.4 | 3.7 |
Hispanic/Latino | 23.0 | 8.2 | 5.1 | 2.4 |
Asian | 20.6 | 7.1 | 3.7 | 1.4 |
American Indian/Alaska Native | 28.4 | 13.7 | 9.3 | 2.2 (this number is considered unreliable) |
Source: Summary health statistics: National Health Interview Survey, 2015. Available at: . Accessed: November 14, 2016. NCHS = National Center for Health Statistics; NHIS = National Health Interview Survey. | ||||
|
|
|
Renal parenchymal disease | Labs/renal ultrasonography | Further workup of etiology of renal disease |
Coarctation of the aorta | Echocardiography | Thoracic and abdominal computed tomography (CT) angiography (CTA) or magnetic resonance (MR) angiography (MRA) |
Cushing syndrome; other states of glucocorticoid excess (eg, chronic steroid therapy | Overnight 1 mg dexamethasone suppression test | 24-hour urinary free cortisol excretion; midnight salivary cortisol |
Drug-induced/drug-related hypertension* | Drug screening | Response to removal of offending agent |
Pheochromocytoma | 24-hour urinary fractionated metanephrines or plasma metanephrines | CT or MR imaging (MRI) of abdomen/pelvis |
Primary aldosteronism, other states of mineralocorticoid excess | Plasma aldosterone to renin ratio (ARR) | Oral sodium loading challenge or intravenous saline infusion test, adrenal CT scan, adrenal vein sampling |
Renovascular disease | Doppler flow ultrasonography, magnetic resonance angiography, computed tomography angiography | Bilateral renal angiography |
Sleep apnea | Berlin Questionnaire, Epworth Sleepiness Score, overnight oximetry | Polysomnography |
Thyroid/parathyroid disease | Thyroid-stimulating hormone level, serum calcium and parathyroid hormone levels | If hyperthyroid, consider radioactive iodine uptake scan |
Congenital adrenal hyperplasia | Hypertension, hypokalemia, low/normal levels of renin and aldosterone | 11-beta-OH, elevated 11-deoxycortisol and androgens 17-alpha-OH, elevated deoxycorticosterone and corticosterone |
Acromegaly | Serum growth hormone during oral glucose load | Elevated insulin-like growth factor-1 (IGF-1) level for age and sex, MRI pituitary |
Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. 2018 Jun. 71(6):e13-e115. Some examples of agents that induce hypertension include nonsteroidal anti-inflammatory drugs (NSAIDs) and cyclooxygenase-2 (COX-2) inhibitors; illicit drugs; sympathomimetic agents; oral contraceptive or adrenal steroid hormones; cyclosporine and tacrolimus; licorice; erythropoietin; and certain over-the-counter dietary supplements and medicines, such as ephedra, ma huang, and bitter orange. Drug-related causes of hypertension include nonadherence, inadequate doses, and inappropriate combinations. | ||
|
|
Chronic hypertension | Prepregnancy or before 20 weeks’ gestation; SBP = 140 mm Hg or DBP = 90 mm Hg that persists >12 weeks postpartum |
Preeclampsia | After 20 weeks’ gestation; SBP =140 mm Hg or DBP = 90 mm Hg with proteinuria (>300 mg/24 h) Can progress to eclampsia More common in nulliparous women, multiple gestation, history of preeclampsia, previous hypertension in pregnancy, and renal disease |
Chronic hypertension with superimposed preeclampsia | New-onset proteinuria after 20 weeks in a woman with hypertension before 20 weeks’ gestation Sudden 2- to 3-fold increase in proteinuria Sudden increase in BP Thrombocytopenia Elevated AST or ALT levels |
Gestational hypertension | Temporary diagnosis Hypertension without proteinuria after 20 weeks’ gestation May be a preproteinuric phase of preeclampsia or a recurrence of chronic hypertension that abated in mid-pregnancy May lead to preeclampsia Severe cases may cause higher rates of premature delivery and growth retardation relative to mild preeclampsia |
Transient hypertension | Diagnosis made retrospectively BP returns to normal by 12 weeks postpartum May recur in subsequent pregnancies Predictive of future primary hypertension |
Chobanian AV, Bakris GL, Black HR, et al, and the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National Heart, Lung, and Blood Institute; National High Blood Pressure Education Program Coordinating Committee. Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. . Dec 2003;42(6):1206-52. ] ALT = alanine aminotransferase; AST = aspartate aminotransferase; BP = blood pressure; DBP = diastolic BP; SBP = systolic BP. | |
|
|
|
|
|
European Society of Cardiology/ European Society of Hypertension (ESC/ESH) ] | 2018 | All adults | Office measurement | At regular intervals on the basis of the blood pressure level: |
American College of Cardiology/American Heart Association (ACC/AHA) ] | 2017 | All adults | Office measurements, requiring at least two measurements at two separate visits. Out-of-office measurements are recommended to confirm the diagnosis of hypertension. | At time of routine preventative care or health assessment |
US Preventive Services Task Force (USPSTF) ] | 2015; 2021 | Adults ≥18 years without known hypertension | Measurements outside of the clinical setting should be obtained for diagnostic confirmation before starting treatment. No evidence was found for a single gold standard protocol for HBPM or ABPM. However, both may be used in conjunction with proper office measurement to make a diagnosis and guide management and treatment options. | Annually for adults age ≥40 and those at increased risk for high blood pressure including those who have high-normal blood pressure (130–139/85–89 mm Hg), are overweight or obese, or are Black. Adults ages ≥18 to < 40 years with normal blood pressure (≤130/85 mm Hg) with no known risk factors should be screened every 3-5 years |
Seventh Report of the Prevention, Detection, Evaluation, and Treatment of the Joint National Committee on High Blood Pressure (JNC 7) ] | 2003 | Adults ages ≥18 years | Diagnosis based on average of 2 or more seated blood pressure readings on each of two or more office visits | At least once every 2 years in adults with blood pressure less than 120/80 mm Hg and every year in those with levels of 120–139/80–89 mm Hg. |
American College of Obstetricians and Gynecologists (ACOG) ] | 2013 | All females ages ≥13 years | Office measurement | Annually as part of routine well-woman care |
Department of Veterans Affairs/Department of Defense (VA/DoD) ] | 2014 | All adults | Office measurement; Diagnosis based on 2 readings at 2 separate visits; For patients where diagnosis remains uncertain, home blood pressure monitoring (2-3 times a day for 7 days) or 24 hour ambulatory monitoring to confirm diagnosis | Periodic, preferably annually, at time of routine preventative care or health assessment; |
European Society of Hypertension /European Society of Cardiology (ESH/ESC) ] | 2013 | All adults | Office measurement; Diagnosis based on at least 2 readings at 2 separate visits; Consider home blood pressure monitoring or 24 hour ambulatory monitoring to confirm diagnosis | At time of routine preventative care or health assessment |
|
|
|
|
Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7) ] | 2003 | All adults except those with diabetes or chronic kidney disease Adults with diabetes or chronic kidney disease | < 140/90 mm Hg < 130/80 mm Hg |
Eighth Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 8) ] | 2014 | Adults age < 60 years and those >18 with diabetes or chronic kidney disease Adults age ≥60 years | < 140/90 mm Hg < 150/90 mm Hg |
European Society of Hypertension/European Society of Cardiology (ESH/ECS) ] | 2013 | All adults except those with diabetes Adults with diabetes | 140-150 mm Hg systolic; consider < 140 mm Hg if the patient is fit and healthy; for ages ≥80 years, the patient's mental capacity and physical heath should also be considered if targeting to < 140 mm Hg < 85 mm Hg diastolic BP |
American Heart Association/American College of Cardiology/American Society of Hypertension (AHA/ACC/ASH) ] | 2015 | Adults ages >80 years Adults with CAD, except as noted below Adults with MI, stroke, TIA, carotid artery disease, peripheral artery disease or abdominal aortic aneurysm | < 150/90 mm Hg < 140/90 mm Hg < 130/80 mm Hg |
American Heart Association/American College of Cardiology (ACC)/Centers for Disease Control and Prevention (AHA/ACC/CDC) ] | 2014 | All adults | < 140/90 mm Hg |
American College of Cardiology/American Heart Association (ACC/AHA) ] | 2017 | All adults | < 130/80 mm Hg |
American Society of Hypertension/International Society of Hypertension (ASH/ISH) ] | 2014 | Adults ages 18-79 years Adults ages ≥80 years | < 140/90 mm Hg; < 130/80 mm Hg BP target may be considered in younger adults < 150/90 mm Hg |
Department of Veterans Affairs/Department of Defense (VA/DoD) ] | 2014 | All adults Adults with diabetes | < 150/90 mm Hg < 150/85 mm Hg |
American Diabetes Association (ADA) ] | 2016 | Adults with diabetes | < 140/90 mm Hg; < 130/80 mm Hg target may be appropriate in younger adults |
American Diabetes Association (ADA) ] | 2017 | Adults with diabetes | < 140/90 mm Hg; < 130/80 mm Hg target may be appropriate for those at high risk of cardiovascular disease (if achievable without undue treatment burden) |
American College of Physicians (ACP) ] | 2017 | Adults ≥ 60 years old | Systolic BP (SBP) < 150 mm Hg; history of cerebrovascular accident or high cardiovascular risk SBP < 140 mm Hg |
CAD = coronary artery disease; MI = myocardial infarction; TIA = transient ischemic attack. | |||
|
| Drug (if needed to reach BP target) | Drug (if needed to reach BP target) |
African ancestry | CCB or thiazide diuretic | ARB or ACEI | Combination of CCB plus ACEI or ARB plus thiazide diuretic |
White and other non-African ancestry ages < 60 years | ARB or ACEI | CCB or thiazide diuretic | Combination of CCB plus ACEI or ARB plus thiazide diuretic |
White and other non-African ancestry ages ≥60 years | CCB or thiazide diuretic; ARB or ACEI also effective | ARB or ACEI; CCB or thiazide diuretic if ARB or ACEI used first | Combination of CCB plus ACEI or ARB plus thiazide diuretic |
| |||
Diabetes (white and other non-African ancestry) | ARB or ACEI | CCB or thiazide diuretic | Alternative 2 drug (CCB or thiazide diuretic) |
Diabetes (African ancestry) | CCB or thiazide diuretic | ARB or ACEI | Alternative 1 drug (CCB or thiazide diuretic) |
Chronic kidney disease | ARB or ACEI | CCB or thiazide diuretic | Alternative 2 drug (CCB or thiazide diuretic) |
Coronary artery disease | Beta-blocker plus ARB or ACEI | CCB or thiazide diuretic | Alternative 2 drug (CCB or thiazide diuretic) |
Stroke | ACEI or ARB | CCB or thiazide diuretic | Alternative 2 drug (CCB or thiazide diuretic) |
Symptomatic heart failure | Beta-blocker plus ARB or ACEI plus diuretic plus spironolactone regardless of BP; CCB can be added if needed for BP control | ||
ACEI = angiotensin-converting enzyme inhibitor; ARB = angiotensin receptor blocker; BP = blood pressure; CCB = calcium channel blocker. | |||
|
|
Chronic hypertension | SBP ≥140 mm Hg or DBP ≥90 mm Hg, present pre-pregnancy or before 20 weeks’ gestation and persisting >12 weeks postpartum |
Preeclampsia | SBP ≥140 mm Hg or DBP ≥90 mm Hg with proteinuria (>300 mg/24 h) that develops >20 weeks’ gestation; Can progress to eclampsia More common in nulliparous women, multiple gestation, women with hypertension ≥4 years, family history of preeclampsia, previous hypertension in pregnancy, and renal disease |
Chronic hypertension with superimposed preeclampsia | New-onset proteinuria after 20 weeks’ gestation in a hypertensive woman In a woman with hypertension and proteinuria before 20 weeks’ gestation: • Sudden 2- to 3-fold increase in proteinuria • Sudden increase in BP • Thrombocytopenia • Elevated AST or ALT levels |
Gestational hypertension | Temporary diagnosis Hypertension without proteinuria after 20 weeks’ gestation May be a preproteinuric phase of preeclampsia or a recurrence of chronic hypertension that abated in mid-pregnancy May lead to preeclampsia Severe cases may cause higher rates of premature delivery and growth retardation relative to mild preeclampsia |
Transient hypertension | Diagnosis made retrospectively BP returns to normal by 12 weeks postpartum May recur in subsequent pregnancies Predictive of future primary hypertension |
ALT = alanine aminotransferase; AST = aspartate aminotransferase; BP = blood pressure; DBP = diastolic BP; SBP = systolic BP | |

Contributor Information and Disclosures
Mackenzie Samson, MD Resident Physician, Department of Internal Medicine, Vanderbilt University Medical Center Disclosure: Nothing to disclose.
Matthew R Alexander, MD, PhD Assistant Professor of Medicine, Department of Medicine, Division of Clinical Pharmacology, Division of Cardiovascular Medicine, Vanderbilt University School of Medicine; Assistant Professor of Molecular Physiology and Biophysics, Vanderbilt University Matthew R Alexander, MD, PhD is a member of the following medical societies: American Association of Immunologists , American Heart Association , American Physiological Society , Federation of Clinical Immunology Societies , Vanderbilt Institute for Infection, Immunology, and Inflammation Disclosure: Nothing to disclose.
Meena S Madhur, MD, PhD, FACC, FAHA Associate Professor with Tenure, Division Chief of Clinical Pharmacology, Department of Medicine, Division of Clinical Pharmacology and Division of Cardiology, Adjunct Associate Professor of Anatomy, Cell Biology, and Physiology, Indiana University School of Medicine; Adjunct Associate Professor of Medicine, Vanderbilt University School of Medicine Meena S Madhur, MD, PhD, FACC, FAHA is a member of the following medical societies: American College of Cardiology , American Heart Association , American Physiological Society , American Society for Clinical Investigation Disclosure: Nothing to disclose.
David G Harrison, MD Betty and Jack Bailey Professor of Medicine and Pharmacology, Director of Clinical Pharmacology, Vanderbilt University School of Medicine David G Harrison, MD is a member of the following medical societies: American College of Cardiology , American Heart Association , American Physiological Society , American Society for Clinical Investigation , Association of American Physicians , Central Society for Clinical and Translational Research , American Federation for Clinical Research , Society for Vascular Medicine Disclosure: Nothing to disclose.
Gary Edward Sander, MD, PhD, FACC, FAHA, FACP, FASH Professor of Medicine, Director of CME Programs, Team Leader, Root Cause Analysis, Tulane University Heart and Vascular Institute; Director of In-Patient Cardiology, Tulane Service, University Hospital; Visiting Physician, Medical Center of Louisiana at New Orleans; Faculty, Pennington Biomedical Research Institute, Louisiana State University; Professor, Tulane University School of Medicine Gary Edward Sander, MD, PhD, FACC, FAHA, FACP, FASH is a member of the following medical societies: Alpha Omega Alpha , American Chemical Society , American College of Cardiology , American College of Chest Physicians , American College of Physicians , American Federation for Clinical Research , American Federation for Medical Research , American Heart Association , American Society for Pharmacology and Experimental Therapeutics , American Society of Hypertension , American Thoracic Society , Heart Failure Society of America , National Lipid Association , Southern Society for Clinical Investigation Disclosure: Nothing to disclose.
Eric H Yang, MD Associate Professor of Medicine, Director of Cardiac Catherization Laboratory and Interventional Cardiology, Mayo Clinic ArizonA Eric H Yang, MD is a member of the following medical societies: Alpha Omega Alpha Disclosure: Nothing to disclose.
Kamran Riaz, MD Clinical Assistant Professor, Department of Internal Medicine, Section of Cardiology, Wright State University, Boonshoft School of Medicine Kamran Riaz, MD is a member of the following medical societies: American College of Cardiology , American College of Physicians , American Society of Echocardiography , Ohio State Medical Association , Royal College of Physicians Disclosure: Nothing to disclose.
Albert W Dreisbach, MD Associate Professor of Medicine, Division of Nephrology, University of Mississippi Medical Center Disclosure: Nothing to disclose.
George R Aronoff, MD Director, Professor, Departments of Internal Medicine and Pharmacology, Section of Nephrology, Kidney Disease Program, University of Louisville School of Medicine
George R Aronoff, MD is a member of the following medical societies: American Federation for Medical Research , American Society of Nephrology , Kentucky Medical Association , and National Kidney Foundation
Disclosure: Nothing to disclose.
Michael S Beeson, MD, MBA, FACEP Professor of Emergency Medicine, Northeastern Ohio Universities College of Medicine and Pharmacy; Attending Faculty, Akron General Medical Center
Michael S Beeson, MD, MBA, FACEP is a member of the following medical societies: American College of Emergency Physicians , Council of Emergency Medicine Residency Directors , National Association of EMS Physicians , and Society for Academic Emergency Medicine
Pamela L Dyne, MD Professor of Clinical Medicine/Emergency Medicine, University of California, Los Angeles, David Geffen School of Medicine; Attending Physician, Department of Emergency Medicine, Olive View-UCLA Medical Center
Pamela L Dyne, MD is a member of the following medical societies: American Academy of Emergency Medicine , American College of Emergency Physicians , and Society for Academic Emergency Medicine
Mert Erogul, MD Assistant Professor of Emergency Medicine, University Hospital of Brooklyn: Consulting Staff, Department of Emergency Medicine, Kings County Hospital Center
Mert Erogul, MD is a member of the following medical societies: American College of Emergency Physicians , American Medical Association , and Society for Academic Emergency Medicine
Allysia M Guy, MD Staff Physician, Department of Emergency Medicine, State University of New York Downstate Medical Center
Dawn C Jung, MD Staff Physician, Department of Emergency Medicine, Suny Downstate Medical Center, Kings County Hospital Center
Dawn C Jung, MD is a member of the following medical societies: American College of Emergency Physicians and Society for Academic Emergency Medicine
Claude Kortas, MD, MEd, FRCP(C) Program Director, Associate Professor, Department of Medicine, University of Western Ontario, Canada
Claude Kortas, MD, Med, FRCP(C) is a member of the following medical societies: American Society of Nephrology, College of Physicians and Surgeons of Ontario, Ontario Medical Association, and Royal College of Physicians and Surgeons of Canada
Stephen C Morris, MD Resident, Section of Emergency Medicine, Department of Surgery, Yale New Haven Hospital
Stephen C Morris, MD is a member of the following medical societies: American College of Emergency Physicians and American Medical Association
L Michael Prisant, MD, FACC, FAHA Cardiologist, Emeritus Professor of Medicine, Medical College of Georgia
L Michael Prisant, MD, FACC, FAHA is a member of the following medical societies: American College of Cardiology , American College of Chest Physicians , American College of Clinical Pharmacology , American College of Forensic Examiners , American College of Physicians , American Heart Association , and American Medical Association
Disclosure: Boehringer-Ingelheim Honoraria Speaking and teaching
Assaad J Sayah, MD Chief, Department of Emergency Medicine, Cambridge Health Alliance
Assaad J Sayah, MD is a member of the following medical societies: National Association of EMS Physicians
Zina Semenovskaya, MD Resident Physician, Department of Emergency Medicine, Kings County Hospital, State University of New York Downstate Medical Center College of Medicine
Sat Sharma, MD, FRCPC Professor and Head, Division of Pulmonary Medicine, Department of Internal Medicine, University of Manitoba; Site Director, Respiratory Medicine, St Boniface General Hospital
Sat Sharma, MD, FRCPC is a member of the following medical societies: American Academy of Sleep Medicine , American College of Chest Physicians , American College of Physicians-American Society of Internal Medicine , American Thoracic Society , Canadian Medical Association , Royal College of Physicians and Surgeons of Canada , Royal Society of Medicine , Society of Critical Care Medicine , and World Medical Association
Mark A Silverberg, MD, MMB, FACEP Assistant Professor, Associate Residency Director, Department of Emergency Medicine, State University of New York Downstate College of Medicine; Consulting Staff, Department of Emergency Medicine, Staten Island University Hospital, Kings County Hospital, University Hospital, State University of New York Downstate Medical Center
Mark A Silverberg, MD, MMB, FACEP is a member of the following medical societies: American College of Emergency Physicians , American Medical Association , Council of Emergency Medicine Residency Directors , and Society for Academic Emergency Medicine
Francisco Talavera, PharmD, PhD Adjunct Assistant Professor, University of Nebraska Medical Center College of Pharmacy; Editor-in-Chief, Medscape Drug Reference
Disclosure: Medscape Salary Employment
Mark Zwanger, MD, MBA Assistant Professor, Department of Emergency Medicine, Jefferson Medical College of Thomas Jefferson University
Mark Zwanger, MD, MBA is a member of the following medical societies: American Academy of Emergency Medicine , American College of Emergency Physicians , and American Medical Association
What would you like to print?
- Print this section
- Print the entire contents of
- Print the entire contents of article

- Epidemiology of Hypertension
- Pathophysiology of Hypertension
- Hypertension and Pregnancy
- Hypertension Medication for Specific Comorbidities
- Labetalol, Nifedipine: Outcome on Pregnancy Hypertension
- Reduce Postpartum Hypertension With Remote Monitoring
- Epistaxis and Hypertension: Reviewing a Complex Relationship

- Drug Interaction Checker
- Pill Identifier
- Calculators

- 2001/viewarticle/999862 Managing Complex Patients With Pulmonary Hypertension and ILD

- 20021928048-overviewDiseases & Conditions Diseases & Conditions Epidemiology of Hypertension


IMAGES
VIDEO
COMMENTS
High blood pressure is a common condition that affects the body's arteries. It's also called hypertension. If you have high blood pressure, the force of the blood pushing against the artery walls is consistently too high.
High blood pressure, also known as hypertension, happens when the force of your blood pushing against the walls of your blood vessels is too high. It can lead to heart attack and stroke.
Hypertension (high blood pressure) is when the pressure in your blood vessels is too high (140/90 mmHg or higher). It is common but can be serious if not treated. People with high blood pressure may not feel symptoms. The only way to know is to get your blood pressure checked.
High blood pressure (hypertension) is diagnosed if the blood pressure reading is equal to or greater than 130/80 millimeters of mercury (mm Hg). A diagnosis of high blood pressure is usually based on the average of two or more readings taken on separate occasions.
The current definition of hypertension (HTN) is systolic blood pressure (SBP) values of 130mmHg or more and/or diastolic blood pressure (DBP) more than 80 mmHg. Persistent BP readings of 140/90mmHg or more should undergo treatment with the usual therapeutic target of 130/80mmHg or less.
High blood pressure (BP), or hypertension, is defined by two levels by the 2017 American College of Cardiology/American Heart Association (ACC/AHA) guidelines [1, 2] : (1) elevated BP, with...
What is high blood pressure or hypertension? The American Heart Association provides information on high blood pressure, low blood pressure, and how to monitor, treat and prevent high blood pressure.
This study aims to determine the association between level and change in physical activity through the adult life course and the onset of hypertension using these 2017 definitions.
High blood pressure, also known as hypertension, is a common condition that can lead to serious complications if untreated. These complications can include stroke, heart failure, heart attack, and kidney damage.
High blood pressure is when the force of blood pushing against your artery walls is consistently too high. This damages your arteries over time and can lead to serious complications like heart attack and stroke. “Hypertension” is another word for this common condition.